|
What is it? The hip adductors are a group of five muscles located on the inside of the thigh that act to move the hip inwards or control hip movements outwards. These muscles also provide stability to the pelvis while standing, walking and running. The muscles attach to the pelvis via the adductor tendon, at the base of the pubic bone. Adductor tendinopathy is a condition affecting the adductor tendon and refers to a typical pattern of pain and stiffness in the groin and inner thigh that accompany this injury. What are the symptoms?
The hallmark of this condition is pain in the groin region with movements of the adductor muscles. There may be a feeling of stiffness or weakness and pain when pressing over the adductor tendon. The pain usually begins gradually and progresses over time. It may build up over a few months and may not go away on its own. In severe cases, the pain may impact day-to-day activities, with pain being present when walking or going up and down stairs. Tendon tears may occur suddenly, however tendinopathy is often already present when this happens. What causes it? Adductor tendinopathy usually occurs due to chronic overuse, particularly for runners and athletes whose sports involve regular changing of directions. Overstretching of the tendon or an increase in training intensity or type often precede the development of adductor tendinopathies. It is thought that excess forces over an extended period of time cause the tendon tissues to degenerate, becoming painful and more prone to tearing. What is the treatment? As many different conditions mimic adductor tendinopathy, accurate diagnosis by a health professional is essential. Certain conditions such as stress fractures of the hip, nerve entrapment or pathologies of the hip joint should first be ruled out. Adductor tendinopathy is treated by first identifying factors that may have led to the development of the condition. Your physiotherapist may recommend a period of rest and suggest that you stop stretching. Common contributing factors are running technique, muscle tightness and/or weakness and training frequency. Your physiotherapist is able to help you maintain your training program to the highest level without aggravating your symptoms and help support tendon healing. They are also able to provide support to unload the tendon along with manual therapy and an exercise program, particularly with eccentric exercises, which have been shown to stimulate tendon regeneration. In most cases, conservative or non-surgical treatment is attempted as the first line of treatment. If this is unsuccessful, cortisone injections can be used to reduce symptoms. In severe cases where the pain persists despite all other attempts at treatment, other medical interventions can be attempted. Once the pain has subsided your physiotherapist is also able to help prevent any further recurrence.
0 Comments
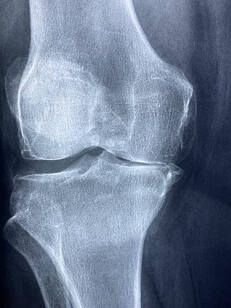
Osteoarthritis (OA) is a common degenerative joint disease that affects many of the joints of the body. The knees are some of the most commonly affected joints, with many people experiencing at least a small degree of osteoarthritis over the age of 40. The disease is characterized by degradation of the cartilage that lines the surfaces of the joint, growth of osteophytes or bony spurs, pain, stiffness and swelling. What are the symptoms?
Stiffness in the morning, pain with movement, clicking, crepitus, swelling and a generalized reduction in joint range of motion are all common symptoms of osteoarthritis. As OA is a progressive disease, the condition is categorized into stages to help describe symptoms and guide treatment. Early stages of OA may have only mild symptoms, however as the disease progresses or in more severe case, a joint replacement may be required. What causes it? While ageing is the most significant risk factor for the development of OA, it’s not an inevitable consequence of growing older. Other factors that may predict the development of OA are obesity, family history, previous joint injury, high impact sporting activities and peripheral neuropathy. It is thought that abnormal wear and tear or stress on the joint is the primary cause of OA. It is also important to note that many people will have changes on X-Ray that show OA, but will have no symptoms – which indicates that simply having OA is not a guarantee of persistent pain. What is the treatment? Your physiotherapist is first able to help diagnosis and differentiate OA from other conditions that may have similar symptoms. An X-Ray can confirm the diagnosis and can be helpful in determining the best course of treatment to follow. While OA is a progressive disorder, there is often a significant improvement that can be made simply by addressing lifestyle factors and any biomechanical factors that may be contributing to pain. How can physio help? Your physiotherapist is able to guide you with strengthening exercises to support the joints, advice for adapting your exercise routine and can even help you to lose weight, all of which have been shown to have a positive impact on the symptoms of OA. If surgery becomes the right course for you, your physiotherapist is able to guide you through this treatment pathway, helping you to prepare and recover from surgery to get the best outcome possible. |
Categories
All
|
|
The Physio Nook
197A Scarborough Beach Road Doubleview WA 6018 08 9446 7017 doubleview@thephysionook.com.au |