|
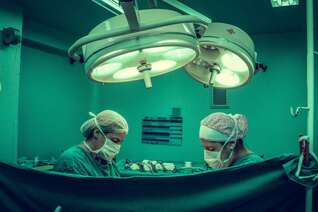
Bursae are small sacs of fluid found throughout the body. These bursae produce synovial fluid and reduce friction between muscles, tendons, ligaments and bones as they move over each other. Bursae are located at strategic points, typically where there are higher points of stress. If a bursa is injured or irritated, it can become inflamed and painful, a condition referred to as bursitis. One bursa that can be affected is the olecranon bursa, which sits just over the hard bony process at the back of the elbow. Olecranon bursitis refers to inflammation of the bursa at this point and is a common condition, particularly in men between the ages of 30-60, though anyone can be affected. What causes it?
Olecranon bursitis has a few possible causes including trauma, overuse and infection. A sharp blow to the elbow, through a fall or hit, might damage the bursa leading to bursitis. In other cases, the bursa can be infected by bacteria, which enter the body through a small skin tear. Bursitis can also develop slowly through friction of the nearby muscles that cause the bursa to become irritated and inflamed. What are the symptoms? The hallmark of this condition is a painful, red, swollen area at the back of the elbow. Typically pain is worst when resting on the tip of the elbow or with elbow movements, particularly when bending or straightening the elbow fully. The pain may last a few months and not go away on its own. The pain can build up gradually, or come on suddenly, depending on the cause. Bursitis caused by infection (septic bursitis) may also be associated with general feelings of illness such as fatigue, fever and body aches. What is the treatment? As there are many different causes of this condition, accurate diagnosis is essential. Your physiotherapist is able to distinguish between olecranon bursitis and similar conditions such as rheumatoid arthritis. Septic bursitis will need to be treated by a medical professional who will determine the best course of action, likely including antibiotics. All types of bursitis can be managed initially with a RICE protocol to reduce pain and swelling (Rest, ice, compression and elevation). Mechanical causes of bursitis can require more in depth identification of the factors that may have led to the development of this condition. Your physio is able to address these factors and possibly provide taping support to unload the bursa along with manual therapy and an exercise program. If this is unsuccessful, cortisone injections are often used to reduce pain and inflammation. In severe cases where the pain persists despite all other attempts at treatment, the bursa can be surgically removed in a procedure called a bursectomy. Once the pain has subsided your physiotherapist is also able to help prevent any further recurrence.
0 Comments
There are many reasons to choose a form of cycling as a sport. Commuting to work by bike can help you conveniently find time for exercise, save money on transport costs and is a great way to exercise if you need to avoid excessive weightbearing. Biking injuries are quite common, but in many cases preventable. Here are a few tips from us to help you prevent cycling injuries and improve your performance. Don't neglect your upper body strength and trunk stability.
While cycling is a sport that predominantly uses the legs, it's a mistake to think that leg strength is the only thing that matters when it comes to biking performance. Increasing the strength, flexibility and balance of your upper body and trunk can actually reduce the amount of effort used to cycle and improve the efficiency of your pedalling. Focusing on your whole body fitness can both improve your riding performance and help to prevent the neck, back and shoulder pain that can come as a result of maintaining postures for extended periods. Yoga and Pilates are great complementary activities to help build upper body strength and stability while also counteracting the effects of prolonged flexed postures of the bike. Don't skimp on your helmet. A good quality helmet can mean the difference between a sore head and a life-changing injury. Helmets become less effective with each hit, as they can lose their shock-absorbing capacity even if they don't appear to be damaged. If in doubt after a crash, make sure you replace your helmet as it may help to save your life. Address aches and pains early. Due to the repetitive nature of cycling, overuse injuries are common. Ensuring your bike is set up correctly to minimise stress on your body while riding and paying attention to small niggles before they become bigger problems can help to identify and resolve issues early so that you can keep cycling without discomfort. Speak to your physiotherapist for more information on how to improve your performance and stay injury-free while biking. Many people know the value that physiotherapy brings to their life and some have even been visiting their physiotherapist since quite early in life. However, for those who have never been to see a physiotherapist before, there can be a question mark over exactly what it is that physiotherapists do. In fact, this is one of the most common questions we as physiotherapists are asked. What is the main job of a physiotherapist?
The answer is tricky, because physiotherapists do so much. Primarily, we might be described as pain management experts, as we work to reduce the pain of our patients, from those who have suffered a new injury, to those who have had pain for several years. We first identify the cause of the pain and then provide manual therapy techniques, education and management strategies to help our patient understand, manage and reduce their pain. While pain is usually the first thing that brings patients to see a physiotherapist, this pain has often caused patients to give up activities that they love and can even be getting in the way of everyday tasks. Many of us reduce our activity levels to reduce pain without even realising it. Physiotherapists are able to identify which areas you are struggling in and why this is occurring. By identifying the cause of your symptoms, we can help to get you back to full function. Physiotherapists are able to do this for everyone including elite athletes and those dealing with serious disabilities. In fact, physiotherapists have a role to play at practically every stage of life. Specialised paediatric physiotherapists can assess infants to monitor their motor skills development and as they grow we help them deal with the pains and vulnerabilities of a growing body. Among other things, we can help improve the function of athletes, assist in preventing injuries, help those with pelvic floor dysfunction and work to prevent falls in the elderly. Not just exercises and massage. Physiotherapists offer a range of treatments, from targeted stretches and strengthening exercises, manual therapies, dry needling, lots of advice on activity modification and massage. Physiotherapists are also committed educators and take our role as such seriously. A huge part of recovering from pain and injury comes from understanding what is happening and how to best manage these issues. Rather than create a dependency on their therapist, we aim to empower our patients to improve their health independently as much as possible. Physiotherapists aim to improve your quality of life and remove any barriers to full participation, whether these barriers are due to pain, weakness or stiffness. The decision to have surgery following an injury is a serious and complicated one. It can be difficult when navigating the minefield of information you receive to know what is the right pathway for you. Unfortunately, the answer is not always obvious which can be confusing. To ensure that surgery is right for you, here are a few questions it pays to ask yourself and your medical team before making a decision. How much will surgery cost and will I need to take time off work?
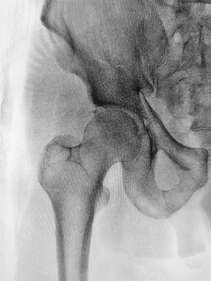
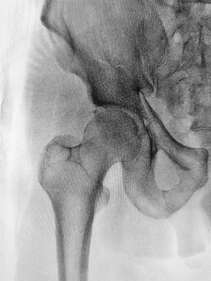
One of the major downsides of surgery is that you will often need to take time off work to recover, resulting in lost income. The cost of the surgery itself may not be completely covered by your insurance, particularly for elective procedures and you will often need to have physiotherapy afterwards. The cost of surgery can really add up, and if you can achieve similar results with physiotherapy alone, you might find yourself in a much better financial situation. What are the potential complications and success rates for your surgery? All surgeries come with risks and potential complications, the probability of these will vary depending on the type of surgery, your age and general health. It is also important to compare the success rates of surgery with a period of physiotherapy treatment. Optimal surgical outcomes still often depend on effective post-surgery management, which can be an argument for considering physiotherapy first. In some cases, however, healing simply will not occur without surgical intervention and physiotherapy will have little success in resolving the issue. What are your post-surgical goals? Not everyone wants to ski down a mountain, but for some, being able to push and trust their bodies is important for both their income and quality of life. Surgery that aims to repair damaged structures might be the right decision for someone who has high demands on their body, but not for another person who isn't very active. Setting your goals for your body can help to guide your decision making process. Before making any major decisions, it is important to consult your medical, surgical and physiotherapy team to ensure you are well educated in all the risks and rewards of undergoing surgery. What is the labrum of the hip? The labrum is a fibrous rim of cartilage that covers the edge and seals your hip socket. This lining of cartilage provides stability for the ball of the thigh bone (femur) inside of the hip socket (acetabulum), while also allowing flexibility. How do tears happen?
Labral tears can occur from an injury such as a twist, slip, or from repetitive stress. For example, athletes such as gymnasts and ballet dancers who have to repeatedly pivot or flex their hip are more likely to damage their labrum than those who do not. Over time this repetitive impingement of the hip joint can cause the labrum to tear. Damage to the labrum, if not managed properly, may lead to early degenerative arthritis. What are the symptoms? If you are experiencing pain in the front of your hip or groin, along with clicking, locking or catching of your hip joint you may have a tear of the hip labrum. Prolonged sitting, standing, walking or pivoting can cause pain and it may also cause a limp when walking. Other possible symptoms include joint stiffness or a feeling of instability in your hip. How can Physiotherapy help? If your physiotherapist suspects a labral tear, they will perform a series of tests to rule out any other conditions. It can be difficult to absolutely confirm a diagnosis of a labral tear in the clinic, however if it is suspected it can be confirmed with medical imaging. Once a diagnosis has been confirmed, your physiotherapist will aim to reduce your symptoms and help you return to your pre-injury activity levels. Treatment will include a stretching and strengthening program. We will also address any training errors or neuromuscular imbalances, provide movement re-education and a variety of manual techniques to help reduce pain. Other treatments are available or may be used in conjunction to physiotherapy including medications, corticosteroid injection or arthroscopy. The right treatment course for each case is decided through consultation with your medical team and will be based on your goals for the future. For most of us, screen time and sitting go hand in hand and both are only increasing as our lives move more online. While short periods in any posture aren't harmful, a lack of movement combined with long periods spent in hunched positions can lead to spinal pain, headaches, shoulder pain and more. If you're needing to spend more time in front of a screen, here are a few tips that can help you to keep flexible and avoid pain. Set movement breaks
Posture in itself isn't always a problem. Spending long periods of time in these postures without taking breaks is the problem. When your body is so used to one position, muscles may become shorter and joints stiffer, making it harder to move out of this posture without pain and discomfort. You can break up your day by setting a timer to move and take a break every 20-30 minutes. Using these short breaks for movement is a great way to both help focus at work and keep your body more flexible. Setup your work and home environment properly Adjusting your work station or setting up a place to relax at home where to you can avoid a hunched posture can help you to reduce time in the same posture. Your physiotherapist can give you tips for how to setup your home and office environment correctly. Take stock of your time spent sitting Time in the car, time on your computer and time on the couch can all quickly add up without you realising. By accounting for the amount of time you spend sitting, you can find more ways to move. For example, if you notice that you're sitting down as soon as you get home, try swapping out watching an episode on TV to going for a walk while listening to a podcast. Ask your physio for specific stretches If you can identify the posture you spend the most time in, your physio can help you to develop a specific exercise and stretching program to counteract these positions most directly and keep you strong and flexible. Can prolonged stress affect your pain and healing? There's a strong suggestion that it can, particularly with chronic pain. If you suffer from ongoing pain you may have noticed this relationship yourself. Many people know that their pain is worse when they are stressed but they don't know why. Stress activates your sympathetic nervous system, this is the state where we move into 'fight, flight or freeze' mode. This part of our nervous system is responsible for keeping us safe when we are in danger, however it can be activated for prolonged periods due to life stressors and many of us lack skills to return control to our parasympathetic nervous system, which is responsible for helping us to rest and digest.
How would this affect pain? During this state, muscles become tensed and ready for action, the nervous system is extra sensitive to stimulus, blood pressure is raised and we are more likely to notice and have negative thoughts. Tense muscles can become tired and painful or put extra stress on other structures, causing pain and irritation. Quite often when in a stressed state, our breathing becomes shallow and rapid, particularly when doing work of low exertion, such as while sitting in an office. Use your breathing to recover. An effective way to help your body return control to the parasympathetic nervous system is to consciously change your breathing. One method is to hold your breath for as long as you can, then let it all out slowly. Once you exhale, your body senses that a threat has passed and can return to a more relaxed state. Another commonly used technique is box breathing. To do this, breathe in for four seconds, hold for four, breathe out for four, hold again for four and repeat. Do this for a few minutes until you start to feel more relaxed and calm. Show your body that you are safe. Other activities that can help your body to relax include yoga, going for a swim or having a shower, or doing some intense exercise where your heart rate is raised. What is it? Shin splints are a painful condition of the lower leg, also known as Medial Tibial Stress Syndrome (MTSS), it is an overuse injury that causes pain along the inside of the tibia (shin bone). It occurs most commonly in runners, hikers and soldiers who march long distances. What are the symptoms?
Shin splints are typified by persistent leg pain, usually the inside of the shin, halfway down the lower leg. The pain might be felt during exercise or directly after. Some people experience a dull ache over their shin that lasts for quite a while after exercise stops, while for others the pain may be sharp and fade quickly. The pain is often progressive, becoming worse with shorter distances. Eventually, shin splints can severely impact activity levels as the pain becomes too severe to continue exercising. Shin splints can be extremely painful and very disruptive to activity levels. As the pain usually starts gradually and progresses many people find themselves unable to continue training. Shin splints may progress to stress fractures if not diagnosed early and managed effectively. How does it happen? Shin splints are predominantly seen in runners who increase their distances quickly, often while training for an event. Activities that require repetitive weight-bearing of any kind, such as marching or high impact sports have also been shown to cause shin splints. Although the pathology of shin splints is unclear, studies have been able to identify certain risk factors that may predispose someone to shin splints. These include... · An quick increase in activity level; · Improper footwear and support; · Higher BMI; · Training on hard or uneven surfaces; · Tight calf muscles; · Flat feet; · Increased external rotation range of the hips; · Females are more likely to develop shin splints than males; · Prior history of shin splints. How can physiotherapy help? The first step for your physiotherapist will be to address any contributing factors to your injury and help to adapt your training program to a level that is optimum for you. A period of relative rest may be recommended along with a targeted strengthening and stretching program for any weak or tight muscles. Switching to low-impact activities such as swimming, cycling and yoga may also help to maintain fitness during recovery. Your running technique may be analyzed and any training errors corrected. When getting back into your training routine, it is usually recommended that distances are not increased by more than 10% per week as this allows the tissues of the body to react to the increased demands and adapt accordingly. A diagnosis of osteoarthritis (OA) for joint pain can be a cause of distress. Many people believe that if you have arthritis your pain is not able to improve and will deteriorate until a joint replacement needs to be performed. The truth is much more complicated, due in part to our bodies’ incredible ability to adapt and change. Physiotherapists have always known that the pain and disability that comes with arthritis can be improved with a targeted exercise program. In some cases, the pain that is attributed to OA is actually due to a different, entirely treatable cause. In other cases, strengthening the musculature around the painful joint can have a significant effect by providing the joint with extra support.
The way we move is often affected negatively by pain and this in itself can create changes to biomechanics that can further contribute to pain. In some cases, surgical intervention is the best choice for treatment and can have incredible results. However, there is a strong case for seeking physiotherapy treatment first to see if you can achieve the same results without surgery. Even if you do choose to go ahead with surgery, working with a physiotherapist beforehand can provide better outcomes. Physiotherapists are highly skilled at identifying exactly what is causing your pain and helping you reach the highest level of function. While exercise is a very powerful treatment, it’s not just any exercise that will take away your pain. To be effective, you will need to have a full assessment and a personalised treatment program created by your physiotherapist. This can involve identifying weak muscles, limitations in flexibility, finding painful trigger points, restoring movement to stiff joints and providing a biomechanical assessment to make a combination of changes that can make a large difference to your pain and activity levels. Your physiotherapist can also identify any other external factors that may be contributing to your pain such as unsupportive footwear, workplace set up etc. Talk to us to see how we can help you manage your osteoarthritis. Ankle sprains are extremely common, however this doesn’t make them easy to cope with when they happen to you. If you’ve ever spent two weeks hobbling around on crutches after a bad twist, you’ll understand just how painful and difficult they can be. What are they?
An ankle sprain refers to an overstretch or tear to the ligaments of the ankle. Commonly, a person will roll their ankle inwards and tear the ligament on the outside. Occasionally, the ankle will twist outwards and the ligaments on the inside of the ankle are torn and even less commonly, the fibres of the ligament that hold the two bones of the lower leg together can tear (this is a "high ankle sprain"). A sprained ankle will usually be painful, swollen, bruised, difficult to walk on and in some cases unstable. How does it happen? Ankle sprains can occur from something as simple as putting weight onto your leg when you think your foot is flat even though it’s not. The most typical pattern is of a person jumping and landing on the outside of their foot or simply slipping and twisting their ankle. A sprained or twisted ankle is one of the most common injuries presented to hospital emergency departments around the world. A medical or health professional should assess any ankle sprain. However, there are some guidelines to help decide if a sprained ankle needs an X-ray... 1. You are unable to put weight on the ankle immediately after the injury. 2. You are unable to take more than 4 steps immediately after the injury. 3. You have pain on the bony edges of the outer foot and ankle. How long do sprains take to heal? Depending on the severity of the tear, from one to six weeks. Your physiotherapist is able to help with recovery and ensure nothing slows down the healing process. Following any injury, joints may remain a little stiff and lose strength and control. Even though the injured tissues have healed, the ankle doesn’t move quite the way it used to. This means that your risk of twisting it again is higher than before the injury. How can physiotherapy help? Correct rehabilitation can help to speed up your recovery and prevent recurring injuries. As well as providing support to the unstable ankle, your physiotherapist will help you to strengthen any weak muscles and restore balance and control through exercise. They are also able to correct any abnormal movement of the joint following the injury. |
Categories
All
|
|
The Physio Nook
197A Scarborough Beach Road Doubleview WA 6018 08 9446 7017 doubleview@thephysionook.com.au |