|
Running is a great way to stay in shape, manage stress and increase your overall health. However, it’s not without potential drawbacks. While generally being a low-risk activity, there are a few injuries that commonly affect runners. As running is a repetitive impact activity, injuries can develop slowly and if left too long, then be difficult to treat. Here are three of the most common conditions faced by runners... 1. Runner’s Knee:
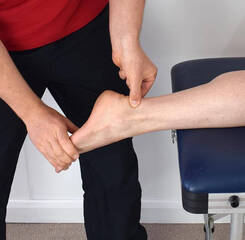
Runner's knee is a persistent pain on the inside of the knee caused by the dysfunctional movement of the knee-cap during movement. The knee-cap ideally sits in the centre of the knee and glides smoothly up and down as the knee bends and straightens, in a process described as tracking. If something causes the kneecap to track abnormally, the surface underneath can become worn, irritated and painful. The pain might be small to start with, however left untreated, can make running too painful to continue. 2. Shin Splints: Shin splints (medial tibial stress syndrome) is a common condition characterised by a recurring pain on the inside of the shin. While the cause of this condition is not always clear, it is usually due to repeated stress where the calf muscles attach to the tibia (shin bone). Why this becomes painful is likely due to a combination of factors that can be identified by your physiotherapist to help you get back on track as soon as possible. 3. Achilles Tendonitis (tendinopathy): The achilles tendon is the thick tendon at the back of the ankle that attaches the calf muscles to the heel bone. The amount of force that this tendon can absorb is impressive and is vital in providing the propulsive force needed for running. If the stresses placed on the tendon exceed its strength, the tendon begins to break down and become painful. Your physiotherapist is able to assess any factors that may contribute to this issue, including footwear, training errors and any biomechanical concerns.
0 Comments
If you have ever suffered from a tendon injury you will know that the recovery can be frustratingly long. Tendons are important tissues of the body, connecting muscles to bones and come in many different shapes and sizes. There are many reasons why tendon injuries can be difficult to treat, as we explain below. Tendon injuries often develop gradually.
Tendons need to be able to transmit forces from muscles to the bones that they attach, however they respond to changes in strength more slowly than muscles do. As muscles become stronger or take on more load, the tendons can fail to keep up with this increased demand becoming painful and damaged. This process can take a while to occur and often changes to tendon tissue has begun long before the pain is noticed. This means that there are likely to be multiple factors to be assessed, including biomechanics and training regimes before the problem can be resolved. Tendons have limited blood supply. Tendons do have their own blood supply, however, it is not abundant as muscles and this can be a factor with healing as all tissues require nutrients for health and to heal. Any condition that compromises circulation, such as diabetes, can predispose tendons to injury and delayed healing. Rest and stretching may not necessarily help. Our instincts in response to tendon pain may not help with recovery. In some cases, stretching can aggravate symptoms and while rest may reduce symptoms, it will not necessarily help with recovery. The best evidence for promoting healthy tendon growth is through addressing poor biomechanics and a tailored strength and loading program. Recovery often relies on adherence to a specific rehab program. One of the biggest barriers to healing tendon pain is that exercises can be easy to do in theory, but hard to do in practice. They can take time and discipline. Your physiotherapist can also help you to find strategies to fit your exercises into your daily routine if you are finding this difficult. Ask your physiotherapist for more information about tendon pain! What is Sever’s Disease? Sever’s disease is a condition that causes pain in the heel of children and adolescents. While it can be quite painful, it is a self-limiting condition that doesn’t usually cause any long-term problems. Sever’s disease is quite common and is the leading cause of heel pain in children and young adolescents. Also known as calcaneal apophysitis, Sever’s disease is an inflammation of the growth plate of the heel. A growth plate is the area of bone where new bone is produced in the growing skeleton and is often weaker than other bony areas. Repeated or excessive stress on this area can cause it to become and inflamed and painful. What are the symptoms?
Children might complain of heel pain that is worse when walking, running or jumping. This may be present following an increase in activity or after a growth spurt. Pain may also be felt when walking on heels. Why does this happen? The achilles tendon attaches to the back of the heel, just next to the growth plate and puts force through this area during movement. If this force becomes too great, the growth plate can become irritated, starting a painful inflammatory process. While increased activity is a predisposing factor, other things may also contribute, such as reduced movement of the ankle, abnormal foot movements when walking and tight calf muscles. It is also possible that Sever’s disease can appear with no obvious cause. What is the treatment? While this is a self-limiting disorder that will go away on its own as the skeletal system completes growth, it can be quite painful and this may impact your child’s activity levels and gait pattern. To prevent any long-term issues from adaptations or changes in activity levels, your physiotherapist can work with your child to find solutions that allow maximum movement with minimum pain. Most of the time, simple education and relative rest or ceasing of aggravating activities are effective. Studies have also found that properly fitted orthotics can help reduce pain while maintaining activity. Physiotherapists can also address any factors which may have caused excess stress in this region, such as abnormally tight muscles or poor gait patterns. They can also advise of pain-relieving treatments and alternative forms of exercise if necessary. None of this information is a replacement for proper medical advice. Always see a medical professional for advice on your injury. Tendons, the connective tissues that join muscles to bone are known for being notoriously difficult to treat once injured. The reason for this is that often they are injured through stress or overuse, and compared to muscles they can have relatively poor blood flow, which is essential for healing. Tendons and muscles work together to move your joints and together are called a contractile unit. As muscles are exercised and gain strength, the attaching tendons are also placed under tension and adapt to this to become stronger. If the load placed on the tissues exceeds their capacity, the tendon fibres can begin to break down and become stiff and painful. Is my pain related to a tendon injury?
For an accurate diagnosis, you will need to be assessed by a physiotherapist. However, some signs that your pain might be coming from an in issue with a tendon are; · The pain is quite specific and can be felt over the tendon itself; · The pain is worse when under stress and improves when rested; · The pain improves after exercise has started, but it might be worse once you cool down; · The area around the tendon may feel stiff after periods of rest, particularly in the morning. How are tendon injuries treated? When it comes to recovery, tendons are often treated differently to other injuries. While each tendon injury is unique and will require assessment and intervention by a physiotherapist, there are a few general approaches that usually help with all tendon injuries. Reducing your activity to a comfortable level is the first step to recovery. Complete rest can actually delay healing as the tendon simply becomes weaker and less able to cope with subsequent loads. Your physiotherapist can provide you with a targeted exercise program to aid your recovery. Eccentric exercises, which are exercises that work alongside gravity, have been shown to stimulate tendon healing and strength. Stretching may aggravate your injury and should be used with caution. Assessment of any biomechanical faults or stresses that are placing undue load on the tendon is also a central component of treatment. Your physiotherapist is able to guide you with your recovery and return to sport to avoid aggravating any injury. Running is a great way to stay in shape, manage stress, and increase your overall wellbeing. However, it's not without its drawbacks. While being a low-risk activity, there are a few injuries that commonly affect runners. As running is a repetitive impact activity, most running injuries develop slowly and can be challenging to get on top of. Here are three of the most common conditions faced by runners, all of which can be helped by your physiotherapist. 1. Runner's Knee:
Runner's knee (patellofemoral pain syndrome) is a persistent pain at the front or inside of the knee caused by the dysfunctional movement of the kneecap during movement. The kneecap sits in a small groove at the centre of the knee and glides smoothly up and down as the knee bends and straightens. If something causes the kneecap to move abnormally, such as muscle imbalance or poor footwear, the surface underneath can become damaged, irritated, and painful. The pain might be mild to start with, but left untreated, runner's knee can make running too painful to continue. 2. Shin Splints: Shin splints (also known as medial tibial stress syndrome) is a common condition characterised by a recurring pain on the inside of the shin. While the cause of this condition is not always clear, it is usually due to repeated stress where the calf muscles attach to the tibia (shin bone). Why this becomes painful is likely due to a combination of factors that can be identified by your physiotherapist to help you get back on track as soon as possible. 3. Achilles Tendonitis/Tendinopathy: The Achilles tendon is the thick tendon at the back of the ankle that attaches the calf muscles to the heel bone. The amount of force that this tendon can absorb is impressive. It is vital in providing the forward propulsive force needed for running. If the stresses placed on the tendon exceed its strength, the tissues begin to breakdown and become painful. Treatment is focused on helping the healthy tendon tissues to strengthen and adapt to new forces while allowing the damaged tissue to heal and regenerate. |
Categories
All
|