|
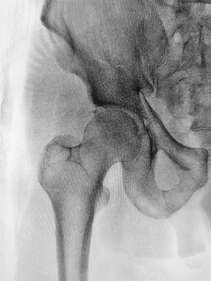
What is the labrum of the hip? The labrum is a fibrous rim of cartilage that covers the edge and seals your hip socket. This lining of cartilage provides stability for the ball of the thigh bone (femur) inside of the hip socket (acetabulum), while also allowing flexibility. How do tears happen?
Labral tears can occur from an injury such as a twist, slip, or from repetitive stress. For example, athletes such as gymnasts and ballet dancers who have to repeatedly pivot or flex their hip are more likely to damage their labrum than those who do not. Over time this repetitive impingement of the hip joint can cause the labrum to tear. Damage to the labrum, if not managed properly, may lead to early degenerative arthritis. What are the symptoms? If you are experiencing pain in the front of your hip or groin, along with clicking, locking or catching of your hip joint you may have a tear of the hip labrum. Prolonged sitting, standing, walking or pivoting can cause pain and it may also cause a limp when walking. Other possible symptoms include joint stiffness or a feeling of instability in your hip. How can Physiotherapy help? If your physiotherapist suspects a labral tear, they will perform a series of tests to rule out any other conditions. It can be difficult to absolutely confirm a diagnosis of a labral tear in the clinic, however if it is suspected it can be confirmed with medical imaging. Once a diagnosis has been confirmed, your physiotherapist will aim to reduce your symptoms and help you return to your pre-injury activity levels. Treatment will include a stretching and strengthening program. We will also address any training errors or neuromuscular imbalances, provide movement re-education and a variety of manual techniques to help reduce pain. Other treatments are available or may be used in conjunction to physiotherapy including medications, corticosteroid injection or arthroscopy. The right treatment course for each case is decided through consultation with your medical team and will be based on your goals for the future.
0 Comments
Osteitis Pubis is a medical term used to describe sports-related groin pain. Osteitis means ‘bone inflammation’, while pubis refers to the specific bone that is affected: the pubic bone. Osteitis pubis is usually an overuse injury that can sometimes be triggered by a specific event. It is characterized by pain deep within the front of the pubic bone, caused by inflammation. The area of the pubic bone affected is specifically known as the pubic symphysis. This type of injury is common in load-bearing athletes such as runners. Other people commonly affected include soccer players and footballers, due to their frequent kicking actions. How does it happen?
Instability around the pelvic region is the primary cause of Osteitis Pubis, particularly if the instability occurs at the connection between the two sides of the pubic bones at the front of the body. The pelvis carries the weight of the upper body and is responsible for providing stability when walking, running and kicking. This means that the joint can become irritated and inflamed. What are the signs and symptoms? Osteitis pubis is aggravated by weight-bearing activities, with running and kicking being the two main culprits. Pain is usually experienced on one side, however both sides can be affected. The pain is usually located at the front of the pelvis and may progress into the hip and groin area as it becomes more severe. Sufferers of Osteitis Pubis may have a history of a previous groin strain, as well as lower back pain. They may also have a history of a sports hernia in the hip area. As with most inflammatory conditions, the pain may be worse when in use, better when resting, and worse overnight into the morning. How can Physio help? Your physiotherapist can help this condition in several ways and will aim to get you back to your pre-injury sporting level. During the assessment, your physio will look at many different things to determine the cause of the condition. Muscle length, muscle strength and muscle control will all be assessed. Your posture in standing, walking and running can also be assessed to determine any irregularities. Your physio will ask you to rest from sports for some time to allow some bony healing to occur. They will then progress you through a rehabilitation program aimed at getting you back to sport. This rehab program will retrain your muscles to stabilise the pelvis when walking, running and kicking. The muscles will also need to have relatively equal flexibility to help stabilize the pelvis. Your physio will give you specific exercises to target the strength and flexibility of these muscles. Finally, your physio will progress you to running or kicking, and allow you to gradually return to sport over a 3 to 6 month period. What is it? The hip adductors are a group of five muscles located on the inside of the thigh that act to move the hip inwards or control hip movements outwards. These muscles also provide stability to the pelvis while standing, walking and running. The muscles attach to the pelvis via the adductor tendon, at the base of the pubic bone. Adductor tendinopathy is a condition affecting the adductor tendon and refers to a typical pattern of pain and stiffness in the groin and inner thigh that accompany this injury. What are the symptoms?
The hallmark of this condition is pain in the groin region with movements of the adductor muscles. There may be a feeling of stiffness or weakness and pain when pressing over the adductor tendon. The pain usually begins gradually and progresses over time. It may build up over a few months and may not go away on its own. In severe cases, the pain may impact day-to-day activities, with pain being present when walking or going up and down stairs. Tendon tears may occur suddenly, however tendinopathy is often already present when this happens. What causes it? Adductor tendinopathy usually occurs due to chronic overuse, particularly for runners and athletes whose sports involve regular changing of directions. Overstretching of the tendon or an increase in training intensity or type often precede the development of adductor tendinopathies. It is thought that excess forces over an extended period of time cause the tendon tissues to degenerate, becoming painful and more prone to tearing. What is the treatment? As many different conditions mimic adductor tendinopathy, accurate diagnosis by a health professional is essential. Certain conditions such as stress fractures of the hip, nerve entrapment or pathologies of the hip joint should first be ruled out. Adductor tendinopathy is treated by first identifying factors that may have led to the development of the condition. Your physiotherapist may recommend a period of rest and suggest that you stop stretching. Common contributing factors are running technique, muscle tightness and/or weakness and training frequency. Your physiotherapist is able to help you maintain your training program to the highest level without aggravating your symptoms and help support tendon healing. They are also able to provide support to unload the tendon along with manual therapy and an exercise program, particularly with eccentric exercises, which have been shown to stimulate tendon regeneration. In most cases, conservative or non-surgical treatment is attempted as the first line of treatment. If this is unsuccessful, cortisone injections can be used to reduce symptoms. In severe cases where the pain persists despite all other attempts at treatment, other medical interventions can be attempted. Once the pain has subsided your physiotherapist is also able to help prevent any further recurrence. |
Categories
All
|