|
One of the most impressive healthcare developments in history is the joint replacement. Many people are able to take out a joint that is extremely painful and dysfunctional and give it a whole new lease on life with a surgically inserted prosthesis. The improvements in this type of surgery over recent years have meant that success rates for joint replacement surgery, particularly hip and knee replacements are higher than ever. If you are struggling with joint pain related to arthritis, it can be difficult to know when to start thinking seriously about surgery. Here are a few things to consider before going for that surgical opinion... Don't assume pain is permanent once you hear the word arthritis
Pain is complex and is often not caused by one single thing. Most people will have some amount of arthritis in their joints past the age of 50, whether or not this is what is causing your pain will be unclear without first seeking assessment and treatment. Many people have some level of degeneration in their joints without experiencing much discomfort at all, as a normal part of the ageing process. It's possible that a combination of strengthening and manual therapy could improve your symptoms significantly, even if osteoarthritis is present. A trial of physiotherapy is recommended before surgery in most cases. Pre-surgical strength and fitness are important This means two things. First of all, your strength before surgery will set you up for much better post-operative results. The second thing is that choosing when to have the surgery means not necessarily waiting until the pain is unbearable before going ahead, as time spent in significant pain can reduce your overall strength and fitness while also putting more stress on other joints. Research the risks and side effects While surgical outcomes are continually improving, no surgery comes without risks and some people will have ongoing pain and stiffness even after their operation. It is important to make an informed decision about when and if you should have a joint replacement. If you are considering a joint replacement, speak to your physiotherapist about all the ways they can support you through your journey and help you come to an informed decision about what is right for you.
0 Comments
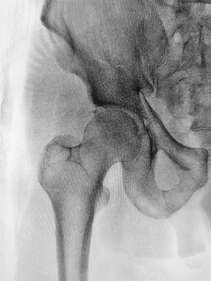
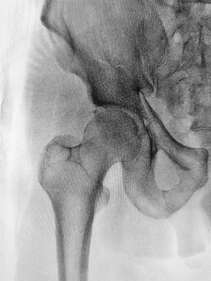
What is the labrum of the hip? The labrum is a fibrous rim of cartilage that covers the edge and seals your hip socket. This lining of cartilage provides stability for the ball of the thigh bone (femur) inside of the hip socket (acetabulum), while also allowing flexibility. How do tears happen?
Labral tears can occur from an injury such as a twist, slip, or from repetitive stress. For example, athletes such as gymnasts and ballet dancers who have to repeatedly pivot or flex their hip are more likely to damage their labrum than those who do not. Over time this repetitive impingement of the hip joint can cause the labrum to tear. Damage to the labrum, if not managed properly, may lead to early degenerative arthritis. What are the symptoms? If you are experiencing pain in the front of your hip or groin, along with clicking, locking or catching of your hip joint you may have a tear of the hip labrum. Prolonged sitting, standing, walking or pivoting can cause pain and it may also cause a limp when walking. Other possible symptoms include joint stiffness or a feeling of instability in your hip. How can Physiotherapy help? If your physiotherapist suspects a labral tear, they will perform a series of tests to rule out any other conditions. It can be difficult to absolutely confirm a diagnosis of a labral tear in the clinic, however if it is suspected it can be confirmed with medical imaging. Once a diagnosis has been confirmed, your physiotherapist will aim to reduce your symptoms and help you return to your pre-injury activity levels. Treatment will include a stretching and strengthening program. We will also address any training errors or neuromuscular imbalances, provide movement re-education and a variety of manual techniques to help reduce pain. Other treatments are available or may be used in conjunction to physiotherapy including medications, corticosteroid injection or arthroscopy. The right treatment course for each case is decided through consultation with your medical team and will be based on your goals for the future. A diagnosis of osteoarthritis (OA) for joint pain can be a cause of distress. Many people believe that if you have arthritis your pain is not able to improve and will deteriorate until a joint replacement needs to be performed. The truth is much more complicated, due in part to our bodies’ incredible ability to adapt and change. Physiotherapists have always known that the pain and disability that comes with arthritis can be improved with a targeted exercise program. In some cases, the pain that is attributed to OA is actually due to a different, entirely treatable cause. In other cases, strengthening the musculature around the painful joint can have a significant effect by providing the joint with extra support.
The way we move is often affected negatively by pain and this in itself can create changes to biomechanics that can further contribute to pain. In some cases, surgical intervention is the best choice for treatment and can have incredible results. However, there is a strong case for seeking physiotherapy treatment first to see if you can achieve the same results without surgery. Even if you do choose to go ahead with surgery, working with a physiotherapist beforehand can provide better outcomes. Physiotherapists are highly skilled at identifying exactly what is causing your pain and helping you reach the highest level of function. While exercise is a very powerful treatment, it’s not just any exercise that will take away your pain. To be effective, you will need to have a full assessment and a personalised treatment program created by your physiotherapist. This can involve identifying weak muscles, limitations in flexibility, finding painful trigger points, restoring movement to stiff joints and providing a biomechanical assessment to make a combination of changes that can make a large difference to your pain and activity levels. Your physiotherapist can also identify any other external factors that may be contributing to your pain such as unsupportive footwear, workplace set up etc. Talk to us to see how we can help you manage your osteoarthritis. For most of us, the hours we spend sleeping are simply a time for rest and recovery. However, you might be surprised to learn that your sleeping position can have a significant impact on your body, particularly if you already have an injury. Here are some tips to help to stay pain free overnight. Back pain tips:
For sufferers of back pain, finding a comfortable position at night can be difficult. The natural curves of the spine need to be maintained and supported throughout the night. Ideally, your body should be held in a position of minimal stress while sleeping. This means that all your joints and muscles are resting in a neutral position A mattress that is too soft might feel comfortable to begin with, but over time will let you sink into it too much, meaning the curve of the lower spine will be lost. Waking up with a stiff or sore back could be a sign that you are using the wrong mattress. A mattress that is too firm can also mean your spine is held in a flattened position, which is both uncomfortable during the night and when you wake up. For many people, sleeping on their side keeps their spine in a more natural alignment than sleeping on their back, especially if they put a pillow between your knees. If you do sleep on your back, placing a pillow under your knees can help to maintain your lumbar spinal curve throughout the night. This can also help to reduce hip and knee pain. Neck pain tips: The neck is often the most vulnerable part of the body if your sleeping setup is not ideal. Side sleepers may let their neck fall excessively to the side with a pillow that is too low or have their neck elevated too much by having their pillows too high. If you find yourself putting your arm under your pillow while you sleep, it is likely that your pillow is too low. Having your shoulder in this position overnight can put unnecessary stress on the structures around the shoulder joint and should be avoided if possible. Stomach sleeping can also put additional pressure on your neck as it is turned to the side for long periods. Hip pain tip: Side sleepers often spend their nights with one leg crossed over their body. This can place extra pressure on the structures on the side of the hip, such as tendons and bursa and can impact the health of these tissues as the compression reduces the blood flow to the area. Placing a pillow under your knee while sleeping on your side in this position can help to maintain a neutral alignment of your hip. Speak to your physiotherapist for more advice on how to improve your sleeping posture and find out if your sleeping setup is right for you. Osteitis Pubis is a medical term used to describe sports-related groin pain. Osteitis means ‘bone inflammation’, while pubis refers to the specific bone that is affected: the pubic bone. Osteitis pubis is usually an overuse injury that can sometimes be triggered by a specific event. It is characterized by pain deep within the front of the pubic bone, caused by inflammation. The area of the pubic bone affected is specifically known as the pubic symphysis. This type of injury is common in load-bearing athletes such as runners. Other people commonly affected include soccer players and footballers, due to their frequent kicking actions. How does it happen?
Instability around the pelvic region is the primary cause of Osteitis Pubis, particularly if the instability occurs at the connection between the two sides of the pubic bones at the front of the body. The pelvis carries the weight of the upper body and is responsible for providing stability when walking, running and kicking. This means that the joint can become irritated and inflamed. What are the signs and symptoms? Osteitis pubis is aggravated by weight-bearing activities, with running and kicking being the two main culprits. Pain is usually experienced on one side, however both sides can be affected. The pain is usually located at the front of the pelvis and may progress into the hip and groin area as it becomes more severe. Sufferers of Osteitis Pubis may have a history of a previous groin strain, as well as lower back pain. They may also have a history of a sports hernia in the hip area. As with most inflammatory conditions, the pain may be worse when in use, better when resting, and worse overnight into the morning. How can Physio help? Your physiotherapist can help this condition in several ways and will aim to get you back to your pre-injury sporting level. During the assessment, your physio will look at many different things to determine the cause of the condition. Muscle length, muscle strength and muscle control will all be assessed. Your posture in standing, walking and running can also be assessed to determine any irregularities. Your physio will ask you to rest from sports for some time to allow some bony healing to occur. They will then progress you through a rehabilitation program aimed at getting you back to sport. This rehab program will retrain your muscles to stabilise the pelvis when walking, running and kicking. The muscles will also need to have relatively equal flexibility to help stabilize the pelvis. Your physio will give you specific exercises to target the strength and flexibility of these muscles. Finally, your physio will progress you to running or kicking, and allow you to gradually return to sport over a 3 to 6 month period. What is Trochanteric Bursitis? The muscles that surround the hips have a complicated role to play. They work to keep the pelvis level and control one of the most flexible joints of the body. They are organized in layers, and the deeper muscles are separated from the outer muscles by sheets of connective tissue, to allow easy gliding, as they interact with each other. With all the layers of muscles working together, some points in the body are more prone to experiencing tension and friction during movement. Small sacs called bursa release a natural lubricant to allow gliding and sliding of different muscular layers and are scattered around the body at points of increased stress. They are found all over the body and usually are quite inconspicuous, which is why most people have never heard of them. However, occasionally something goes wrong, and they become irritated and painful. This will usually happen in a few typical places in the body and one of them this over the greater trochanter, the bony part of the outer hip. What Are The Symptoms?
The most common symptom of trochanteric bursitis is pain on the outside of your hip, which may radiate down to the knee. You can experience pain with a number of activities such as walking, jogging, climbing stairs and cycling or simply lying on the affected side. How Does It Happen? The most common cause for this is a combination poor biomechanics and overuse. When you have poor biomechanics, the structures around the bursa become tighter and can begin to irritate the bursa. Some things that contribute to poor biomechanics around the hip are weak, uncontrolled muscles, tight muscles, flat feet with unsupportive footwear, a difference in leg length, incorrect exercise equipment and scoliosis. These can all lead to irritation of the bursa around the hip. How Can Physiotherapy Help? As there are many other conditions that can cause pain at the outer hip, correct diagnosis is essential. Once diagnosis is confirmed, the first phase of treatment is to reduce pain and irritation. This can be done with muscle release techniques, ice or heat (depending on the case), rest, fitting you with orthotics and advice for modification to your lifestyle. Your physiotherapist will also evaluate the causes of the irritation and prescribe a suitable rehabilitation program to change your biomechanics. Serious cases can be treated with corticosteroid injection or even surgery, but with thorough physiotherapy treatment, these are rarely needed. What is it? The hip adductors are a group of five muscles located on the inside of the thigh that act to move the hip inwards or control hip movements outwards. These muscles also provide stability to the pelvis while standing, walking and running. The muscles attach to the pelvis via the adductor tendon, at the base of the pubic bone. Adductor tendinopathy is a condition affecting the adductor tendon and refers to a typical pattern of pain and stiffness in the groin and inner thigh that accompany this injury. What are the symptoms?
The hallmark of this condition is pain in the groin region with movements of the adductor muscles. There may be a feeling of stiffness or weakness and pain when pressing over the adductor tendon. The pain usually begins gradually and progresses over time. It may build up over a few months and may not go away on its own. In severe cases, the pain may impact day-to-day activities, with pain being present when walking or going up and down stairs. Tendon tears may occur suddenly, however tendinopathy is often already present when this happens. What causes it? Adductor tendinopathy usually occurs due to chronic overuse, particularly for runners and athletes whose sports involve regular changing of directions. Overstretching of the tendon or an increase in training intensity or type often precede the development of adductor tendinopathies. It is thought that excess forces over an extended period of time cause the tendon tissues to degenerate, becoming painful and more prone to tearing. What is the treatment? As many different conditions mimic adductor tendinopathy, accurate diagnosis by a health professional is essential. Certain conditions such as stress fractures of the hip, nerve entrapment or pathologies of the hip joint should first be ruled out. Adductor tendinopathy is treated by first identifying factors that may have led to the development of the condition. Your physiotherapist may recommend a period of rest and suggest that you stop stretching. Common contributing factors are running technique, muscle tightness and/or weakness and training frequency. Your physiotherapist is able to help you maintain your training program to the highest level without aggravating your symptoms and help support tendon healing. They are also able to provide support to unload the tendon along with manual therapy and an exercise program, particularly with eccentric exercises, which have been shown to stimulate tendon regeneration. In most cases, conservative or non-surgical treatment is attempted as the first line of treatment. If this is unsuccessful, cortisone injections can be used to reduce symptoms. In severe cases where the pain persists despite all other attempts at treatment, other medical interventions can be attempted. Once the pain has subsided your physiotherapist is also able to help prevent any further recurrence. |
Categories
All
|