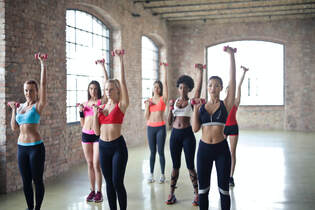|
Can prolonged stress affect your pain and healing? Research now suggests that it can, particularly with chronic pain. If you suffer from ongoing pain you may have noticed this relationship yourself. Many people know that their pain is worse when they are stressed but they don't know why. Stress activates your sympathetic nervous system, this is the where we can move into "fight, flight or freeze" mode. The sympathetic nervous system is responsible for keeping us safe when we are in danger, however it can be activated for prolonged periods and many of us lack the skills to return control to our parasympathetic nervous system, which is responsible for helping us to "rest and digest".
How would this affect pain? During this state muscles become tense and ready for action, the nervous system is extra sensitive to stimulus, blood pressure is raised and we are more likely to notice and have negative thoughts. Tense muscles can become tired and sore or put extra stress on other structures, causing pain and irritation. Often when in a stressed state our breathing becomes shallow and rapid, even when not really exerting ourselves, such as while sitting in an office. Use your breathing to recover. An effective way to help your body return control to the parasympathetic nervous system is to consciously change your breathing. One method is to hold your breath for as long as you can, once you relieve your breath your body senses that a threat has passed and can return to a more relaxed state. Another commonly used technique is box breathing. To do this, breathe in for four seconds, hold for four, breathe out for four, hold again for four and repeat. Do this for a few minutes until you start to feel more relaxed and calm. Show your body that you are safe. Other activities that can help your body to relax include yoga, going for a swim or having a shower, or doing some intense exercise where your heart rate is raised. Speak to your physiotherapist for more information on this topic and tips to help you relax during the day.
0 Comments
The benefits of keeping active may seem obvious, yet it can't hurt to be reminded of the many ways exercise can improve your life. Here are a few of our favourite reasons to get moving... 1. Exercise improves energy levels.
Improving your fitness means your body is capable of achieving more for the same energy expenditure. While doing exercise can make you tired in the short term, regular improvements to your fitness will help you get more out of your body each day, with seemingly less effort. 2. Exercise can help to reduce stress. If you are stuck in a state of stress or anxiety, exercise can help you move out of it into a calmer and more relaxed state, improving your mood, concentration and sleep. There are now many studies to support this. 3. Exercise and hobbies can help you build connections and community. Making new friends as an adult can be surprisingly difficult and the importance of connection and community is being recognised more and more as being essential for overall wellbeing. Being part of a team, group or club is a great way to build confidence and meet friends as well as keeping active. 4. Exercise keeps your muscles, tendons, joints and bones healthy. Our bodies are often compared to machinery or car parts. However, there are some crucial differences between our bodies and machines, including the fact that our bodies respond to exercise by becoming stronger and healthier, rather than being worn out. As an example, one of the best ways to prevent osteoporosis is through regular high impact activity, which stimulates bone growth. 5. Exercise can help to reduce injuries. Similar to the previous point, tissues that are used regularly are stronger, more elastic and are less likely to tear or break when under stress. Regular exercise is the best way to keep your body in a healthy state and prevent injuries. Finding the right exercise for you can be tricky, your physiotherapist can help you with suggestions based on your ability and skillset if you need some help. What is it? Fibromyalgia is a chronic condition characterised by widespread pain throughout the body along with fatigue, memory problems, sleep and mood disorders. Sufferers of fibromyalgia often spend years trying to find a diagnosis that fits their symptoms and fluctuate between periods of having high energy and ‘crashes’ of fatigue and pain. In severe cases, fibromyalgia can cause significant lifestyle disruptions, including reduced activity, unemployment and depression. The underlying mechanism that creates the symptoms of fibromyalgia has been shown to be increased pain amplification by the central nervous system and reduced activation of the sympathetic nervous system. Essentially this means that small pain signals in the body are processed as large pain signals by the central nervous system. What causes it?
Fibromyalgia is a complicated condition that is poorly understood. This can be very frustrating for sufferers, who often find themselves being shuffled between health practitioners looking for answers and long term relief. While the pain generally feels muscular, usually little to no muscular damage or injury can be found on physical assessment or investigations. The symptoms can also mimic those of an infectious illness or other chronic diseases. Often a diagnosis of fibromyalgia is reached after other diseases and causes have been ruled out. The cause of fibromyalgia is as yet unknown. It was initially thought that the depression and reduced activity that are often associated with fibromyalgia could be causative, however it has been shown that these are symptoms of fibromyalgia rather than causes. Other significant signs are a lack of REM (good quality) sleep in sufferers and a positive result of more than 11 out of 18 muscular trigger points. What is the treatment? Following a diagnosis of fibromyalgia, the primary strategy is to understand and manage your symptoms. This can involve pacing activities and exercise so as to reduce ‘crashes’ and pain cycles that lead to frustration. Identifying activity, employment and a routine that doesn’t exacerbate symptoms can have a significant impact on quality of life for someone with fibromyalgia. Having psychological support can also be very important to help deal with the emotional distress of a complex chronic condition that has no outward physical signs. Treatments that have been shown to help reduce symptoms are TENS (electrical stimulation) which produces an endorphin response and can reduce pain; certain medications may be helpful when prescribed by a doctor; and education and understanding of this condition, helping to manage and maintain some control over your symptoms. Physiotherapists can have a large role in education and helping patients find a routine and activity level that helps them manage their condition as best as possible, as well as providing symptomatic relief during pain cycles with manual therapy, stretching and massage techniques. It is always best to see a medical professional for advice on your individual injury or condition. |
Categories
All
|