|
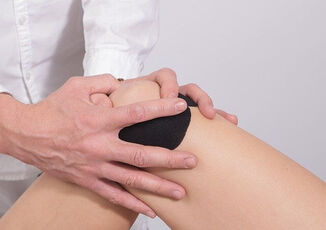
What is it? Our knees are complex hinge joints, designed to provide stability from side to side and smooth movement forwards and back as you walk, kick and run. The patella, or kneecap, is a small bone embedded in the tendon of the quadriceps muscle that protects the knee and also provides extra leverage to the quadriceps, amplifying their strength. The patella moves up and down in a groove at the front of the knee as the knee bends and straightens. Usually this movement is smooth, with little friction, however, if something causes the patella to move in a dysfunctional way, the soft tissue between the kneecap and the knee can become irritated, causing pain in a typical pattern. This condition is often referred to as ‘runner’s knee’, PFJ syndrome or patellofemoral pain syndrome (PFPS). What causes it?
The patella usually sits in a balanced position in the shallow groove at the front of the knee and moves easily without friction. The patella is attached to the quadriceps muscle at the top and connected to the lower leg via the patella tendon at the bottom. When the quadriceps contracts, this pulls on the patella and acts to straighten the knee. If one side of the quadriceps is stronger or tighter than the other, it can cause the kneecap to pull to one side and over time become irritated. There can be many factors that cause a muscle imbalance or weakness on one side of the quadriceps. In most people, the outer aspect of the quadriceps tends to be stronger and tighter than the inner muscle. Certain postures and leg positions require the outer muscles to work harder and the inside muscles to become less active. Lack of arch support in your feet or simply a physical abnormality of the knee can also place stress on the movement of the patella. What are the symptoms? This condition is characterized by pain felt on the inside or behind the patella with activities that require repetitive bending of the knee. There may be a sensation of crunching, clicking or grinding and some people report that their knee suddenly gives way. The pain is commonly felt when running, going up and down stairs or when doing squats and is generally relieved with rest. The pain may start as a small niggle and gradually become worse over time. How can physiotherapy help? The first step in effective treatment is to exclude any other conditions and have a physiotherapist confirm the diagnosis. Your physiotherapist is able to determine which factors are contributing to this condition, which could include poor posture, a lack of arch support in your feet or poor running technique. Once these factors have been identified, you will be provided with a specific treatment program to best approach your condition. PFJ syndrome usually responds well to biomechanical analysis and correction of any muscular weakness and imbalance. Having the correct shoes and orthotics can also make a huge difference. There are some short-term treatments, such as patella taping, dry needling, trigger point therapy and ultrasound, which may help alleviate symptoms quickly and keep you active while you address the other factors contributing to your pain.
0 Comments
There’s no doubt that doing the right thing for your health can be difficult. Whether that involves eating healthier, exercising more, flossing your teeth or even doing your physio exercises, the best choice is not always the most comfortable. Once a habit has formed and become part of your routine, making the right decision for yourself can become a lot more straightforward. Getting to that point is easier said than done. Here are a few tips to help you reach your health goals...
1. Choose a friend to join you for accountability. One way to guarantee that you show up for an early morning gym session is to have a friend who you partner with. You might be comfortable sleeping in for yourself, but not so much when you have someone else you’re letting down. Sharing difficult tasks with a friend can make them more enjoyable and you can also set up competitions with them if you need a little extra motivation. 2. Combine tasks with an activity that you do like. Love a true crime podcast? The gym can be the time to catch the latest episode or even stream your favourite show. Anything you do that helps to increase the enjoyment of the activity you’re avoiding is going to help you get started. 3. Batch tasks to be more efficient. Are you trying to drink more water, floss and also complete your physio exercises? Why not do all three in the same sitting? Combining tasks can be a surprisingly effective use of time and a way to remind yourself to complete them. 3. Use positive reinforcement for good behaviour, rather than punishments. Many people will feel bad when they fail to reach their goals and try to restrict themselves in another area to compensate. It can be a much more effective motivation strategy to reward yourself after completing a task, rather than punish yourself for not doing it. 4. Get your foot in the door. Putting your shoes on can be the hardest part of going for a run. If you’re struggling to complete a task, sometimes all you have to do is tell yourself you only need to do five minutes. Once you’ve started quite often you’ll want to do more, but setting small goals can be the trick to getting started. Once a habit is in place, the easy part is to increase the intensity or length of time you’re doing it. It's believed that it takes 21 days of completing a task for a habit to be formed, where you will then do it automatically as part of your routine. For more tips and tricks on how to reach your health goals, speak to your physiotherapist. What are they? The calf muscles refer to a group of muscles at the back of the lower leg that act to point the foot and toes down, away from the body. They play an important role in walking and running. A tear or strain of these muscles occurs when some or all of the muscle fibres are torn or overstretched. This is a common injury that can affect anyone from elite athletes to recreational exercisers. How do injuries happen?
Calf tears are often caused by sudden, forceful movements or overuse of the calf muscles, leading to the rupture or strain of muscle fibers. Common mechanisms of injury are a quick take off during sports or simply going for a long walk when not accustomed. Factors that may increase the risk of a calf tear are previous calf tears that have not been fully rehabilitated, tight or weak calf muscles, poor balance and poorly fitting footwear. What are the symptoms? Typical symptoms of a calf tear are sharp pain over the site of the tear, especially with movement, swelling, bruising, and difficulty walking or standing. The severity of the injury can range from mild muscle strain to a complete tear, which will determine the appropriate treatment approach. How can physiotherapy help? The first step in managing calf tears is accurate diagnosis by a medical professional, who is able to rule out other conditions that might mimic a calf tear. They can determine the extent of the damage and create a personalised treatment plan based on your specific needs. This ensures that the rehabilitation process addresses the root cause of the injury, leading to better outcomes. Reducing pain and inflammation is important in the first one to two days following the injury. The muscle may need support during this time, depending on the severity. Over time as the swelling and inflammation subsides, your physiotherapist will help to address any factors that contributed to the injury such as muscle weakness or imbalances. Calf tears often lead to stiffness and limited range of motion in the affected leg if not fully rehabilitated. Physiotherapists implement targeted stretching and range of motion exercises to restore flexibility and prevent the formation of scar tissue that may impede recovery. Gradually, the patient can regain the ability to move the calf muscle without pain or discomfort. Rehabilitation past this point will progressively challenge the calf muscles without causing further damage. Strengthening these muscles not only aids in the healing process but also reduces the risk of future calf tears. What is it? Shin splints are a painful condition of the lower leg, also known as Medial Tibial Stress Syndrome (MTSS), it is an overuse injury that causes pain along the inside of the tibia (shin bone). It occurs most commonly in runners, hikers and soldiers who march long distances. What are the symptoms?
Shin splints are typified by persistent leg pain, usually the inside of the shin, halfway down the lower leg. The pain might be felt during exercise or directly after. Some people experience a dull ache over their shin that lasts for quite a while after exercise stops, while for others the pain may be sharp and fade quickly. The pain is often progressive, becoming worse with shorter distances. Eventually, shin splints can severely impact activity levels as the pain becomes too severe to continue exercising. Shin splints can be extremely painful and very disruptive to activity levels. As the pain usually starts gradually and progresses many people find themselves unable to continue training. Shin splints may progress to stress fractures if not diagnosed early and managed effectively. How does it happen? Shin splints are predominantly seen in runners who increase their distances quickly, often while training for an event. Activities that require repetitive weight-bearing of any kind, such as marching or high impact sports have also been shown to cause shin splints. Although the pathology of shin splints is unclear, studies have been able to identify certain risk factors that may predispose someone to shin splints. These include... · An quick increase in activity level; · Improper footwear and support; · Higher BMI; · Training on hard or uneven surfaces; · Tight calf muscles; · Flat feet; · Increased external rotation range of the hips; · Females are more likely to develop shin splints than males; · Prior history of shin splints. How can physiotherapy help? The first step for your physiotherapist will be to address any contributing factors to your injury and help to adapt your training program to a level that is optimum for you. A period of relative rest may be recommended along with a targeted strengthening and stretching program for any weak or tight muscles. Switching to low-impact activities such as swimming, cycling and yoga may also help to maintain fitness during recovery. Your running technique may be analyzed and any training errors corrected. When getting back into your training routine, it is usually recommended that distances are not increased by more than 10% per week as this allows the tissues of the body to react to the increased demands and adapt accordingly. Running is a great way to stay in shape, manage stress and increase your overall health. However, it’s not without potential drawbacks. While generally being a low-risk activity, there are a few injuries that commonly affect runners. As running is a repetitive impact activity, injuries can develop slowly and if left too long, then be difficult to treat. Here are three of the most common conditions faced by runners... 1. Runner’s Knee:
Runner's knee is a persistent pain on the inside of the knee caused by the dysfunctional movement of the knee-cap during movement. The knee-cap ideally sits in the centre of the knee and glides smoothly up and down as the knee bends and straightens, in a process described as tracking. If something causes the kneecap to track abnormally, the surface underneath can become worn, irritated and painful. The pain might be small to start with, however left untreated, can make running too painful to continue. 2. Shin Splints: Shin splints (medial tibial stress syndrome) is a common condition characterised by a recurring pain on the inside of the shin. While the cause of this condition is not always clear, it is usually due to repeated stress where the calf muscles attach to the tibia (shin bone). Why this becomes painful is likely due to a combination of factors that can be identified by your physiotherapist to help you get back on track as soon as possible. 3. Achilles Tendonitis (tendinopathy): The achilles tendon is the thick tendon at the back of the ankle that attaches the calf muscles to the heel bone. The amount of force that this tendon can absorb is impressive and is vital in providing the propulsive force needed for running. If the stresses placed on the tendon exceed its strength, the tendon begins to break down and become painful. Your physiotherapist is able to assess any factors that may contribute to this issue, including footwear, training errors and any biomechanical concerns. Osteitis Pubis is a medical term used to describe sports-related groin pain. Osteitis means ‘bone inflammation’, while pubis refers to the specific bone that is affected: the pubic bone. Osteitis pubis is usually an overuse injury that can sometimes be triggered by a specific event. It is characterized by pain deep within the front of the pubic bone, caused by inflammation. The area of the pubic bone affected is specifically known as the pubic symphysis. This type of injury is common in load-bearing athletes such as runners. Other people commonly affected include soccer players and footballers, due to their frequent kicking actions. How does it happen?
Instability around the pelvic region is the primary cause of Osteitis Pubis, particularly if the instability occurs at the connection between the two sides of the pubic bones at the front of the body. The pelvis carries the weight of the upper body and is responsible for providing stability when walking, running and kicking. This means that the joint can become irritated and inflamed. What are the signs and symptoms? Osteitis pubis is aggravated by weight-bearing activities, with running and kicking being the two main culprits. Pain is usually experienced on one side, however both sides can be affected. The pain is usually located at the front of the pelvis and may progress into the hip and groin area as it becomes more severe. Sufferers of Osteitis Pubis may have a history of a previous groin strain, as well as lower back pain. They may also have a history of a sports hernia in the hip area. As with most inflammatory conditions, the pain may be worse when in use, better when resting, and worse overnight into the morning. How can Physio help? Your physiotherapist can help this condition in several ways and will aim to get you back to your pre-injury sporting level. During the assessment, your physio will look at many different things to determine the cause of the condition. Muscle length, muscle strength and muscle control will all be assessed. Your posture in standing, walking and running can also be assessed to determine any irregularities. Your physio will ask you to rest from sports for some time to allow some bony healing to occur. They will then progress you through a rehabilitation program aimed at getting you back to sport. This rehab program will retrain your muscles to stabilise the pelvis when walking, running and kicking. The muscles will also need to have relatively equal flexibility to help stabilize the pelvis. Your physio will give you specific exercises to target the strength and flexibility of these muscles. Finally, your physio will progress you to running or kicking, and allow you to gradually return to sport over a 3 to 6 month period. What are they? The hamstrings are a large group of muscles located at the back of the thigh. Their job is to bend the knee, extend the hip backwards and stabilise the leg. The muscles can be injured at any point along their length but are most vulnerable where the tendon and muscle fibres join together. This is a common injury for players of all sports that involve running, and particularly those that involve quick movements and kicking. What are the causes?
As the hamstrings cross two large joints (the hip and the knee), they need to perform complicated movements, often activating suddenly and with great force. They are often stretched during a fall, a powerful kick of a ball or a sudden take-off. Factors that increase the chance of a tear include poor flexibility, strength or neural mobility. Other factors that contribute to hamstring injuries are muscle imbalances, abnormal lower limb biomechanics, fatigue, and inadequate warm-up. The biggest predictor of a future hamstring tear though, is a previous hamstring injury. What are the symptoms? The most common symptom of a strained or torn hamstring is a sharp pain at the back of the thigh, often immediately after intense activity. There may also be swelling, bruising, difficulty walking and pain with knee movements. Your physiotherapist can confirm that the pain is due to injured hamstrings rather than any other issues, and tell you how bad the strain or tear is. Although not usually required, diagnosis can be confirmed by having an MRI or ultrasound scan. How can physiotherapy help? Once a diagnosis has been made, the first step is to follow the R.I.C.E protocol (Rest, Ice, Compression, Elevation). During the first 48 hours, you should apply ice for 20 minutes every one to two hours to reduce swelling and bruising. Consultation with your physio will include advice about your recovery, and when it is appropriate to return to sport. Your physiotherapist has many techniques that can promote healing and reduce scar tissue formation, which may include ultrasound, deep tissue therapy, electrotherapy and dry needling. Crucially, they will also prescribe you an exercise program to return strength, flexibility and control to your muscles, getting you back to your sport quickly and safely. Due to the high chance of recurrence, rehabilitation is very important and usually takes 6-12 weeks. If the muscle is completely torn, surgery may be required before rehabilitation can start. Your physiotherapist will work with you to help you set goals to get you back to your favourite activities as soon as possible. There is more to distance running than you may think. In this article, we offer some words of wisdom from our physiotherapists to help you get the most out of your training and avoid injuries. 1. Choose your shoes carefully:
Repeated stress from running long distances will show up any biomechanical flaws in your body relatively quickly. Choosing the wrong shoes can exacerbate an existing problem causing pain and injury. Your physiotherapist or podiatrist can guide you on what style of shoe will best suit you. 2. Don't neglect your upper body: While running can appear to be a purely leg based activity, increasing the strength and mobility of your upper body can have a surprisingly big impact on your posture, running style, breathing and overall performance. 3. Find time to train strength as well as endurance: Your body is great at finding ways to compensate for weak muscles. However, over time this can lead to overuse injuries of tendons and muscles. Identifying any areas of weakness early and specifically strengthening these muscles can both improve your running technique and efficiency, as well as help keep you injury free. 4. Pace your progress: Entering an event is a great way to set a specific goal and keep you motivated. While trying to increase distances and speed, it is easy to forget to include rest days as a part of your routine. Your body needs time to recover and restore itself just as much as it needs the active portions of your training program. Increasing your speed and distances gradually also allows your body to adapt to new demands without breaking down. 5. Enjoy your training and listen to your body: Your body will often guide you as to when you need to rest and when you can push a little further. Training will be more enjoyable when you are well rested and pain free. Most importantly, if you are able to enjoy your runs, this will help you maintain motivation over a longer period of time, so you can continue for many years to come. Ask your physiotherapist for more tips on how to reach your running goals while staying injury-free. The knees function as hinges, allowing your legs to swing forwards and backwards smoothly as you walk, kick and run. The knee cap (the patella) sits at the front of the knee and has a variety of functions, including guiding the muscles that straighten the knee, protecting the knee joint and absorbing forces when the knee is bent. When something goes wrong and the patella doesn’t glide up and down smoothly, the soft tissue between the kneecap and the knee can become irritated, causing pain. This is called patellofemoral pain syndrome (PFPS), sometimes also referred to as PFJ syndrome, patella maltracking or runner's knee. Pain is usually felt on the inside of the kneecap when running, squatting, jumping, bending, using stairs or hopping. Sitting for long periods of time or keeping your knees bent can also result in pain. What Causes It?
The patella sits in a shallow groove at the front of the knee and usually moves up and down as the knee bends and straightens without too much trouble. The quadriceps muscles located at the front of the thigh contract and pull on the kneecap, which then attaches to the shin bone and acts to straighten the knee. If one side of the quadriceps is stronger or tighter than the other, it can cause the kneecap to pull more to one side and over time become irritated. The cause of muscle imbalance or weakness can be varied. In general, the outer muscles of the thigh tend to be stronger and tighter than the inner muscles. If you have poor posture and hip position, this can cause the outer muscles to work harder and the inside muscles to become weaker. Lack of arch support in your feet or a physical anomaly of the knees can also contribute to this condition. How Can Physiotherapy Help? Diagnosing patellofemoral pain syndrome correctly is important because pain on the inside of the knee can also be caused by other injuries, dislocations, inflammation, arthritis and a variety of other less common conditions. With that in mind, it is helpful to know that your physiotherapist can diagnosis PFPS accurately and identify its likely causes. Whether it is due to poor posture, a lack of arch support in your feet, or poor running technique, your physiotherapist will assess the problem and provide a specific treatment program to best approach your condition. PFPS usually responds well to biomechanical analysis and correction of any muscular weakness and imbalance. Having the correct shoes and orthotics can also make a huge difference. There are some short-term treatments, such as patella taping, dry needling, massage, trigger point therapy and ultrasound, which may help alleviate symptoms quickly and keep you active while you address the other factors contributing to your pain. In the rare case that your condition is not helped by physiotherapy, surgery may be considered as a last resort. For more information, please ask your physiotherapist. What is a stress fracture? A stress fracture is a microscopic fracture of the bone that is often not picked up on X-ray. If left untreated, a stress fracture can cause significant disability and develop into a full fracture, possibly even requiring surgery. The majority of stress fractures occur in the lower limb, being particularly common in the hip, shins and foot at points where the most force passes through when weight bearing. Most stress fractures are overuse injuries and are common in long distance runners. What are the symptoms?
As with many overuse injuries, the pain of a stress fracture starts gradually, beginning with pain during or after activity or sometimes the morning after. If activity continues without modification, the pain will gradually increase. Eventually most people are unable to maintain their usual activity level. Stress fractures are common in runners and military personnel who are required to march for long periods. A stress fracture will be more likely to occur in a person who has weaker bone strength, such as someone with osteoporosis, which is itself affected by many factors such as adequate calcium intake, vitamin D deficiency and a history of inactivity. How are stress fractures treated and how long will it take to get better? Stress fractures can easily be mistaken for other conditions such as shin splints. As the fracture is often too small to show up on X-ray, definitive diagnosis can be made using MRI, CT or bone scan. After diagnosis, the most important part of treatment will be resting the area to allow the bone to heal before resuming activity. Stress fractures usually need at least 6 weeks to recover fully. Some areas of the body have poor blood supply, which makes healing more complicated. For example, stress fractures of the navicular bone of the foot may need to be kept still and placed in a boot or cast for a period of time to heal properly. Other aspects of treatment will involve correcting any factors that contributed to the original injury. There is some evidence that unsupportive footwear is a risk factor, along with poor biomechanics and weak muscles that provide inadequate support to the skeletal system during activity. Speak to your physiotherapist if you suspect you may have a stress fracture or if you want to know more. |
Categories
All
|