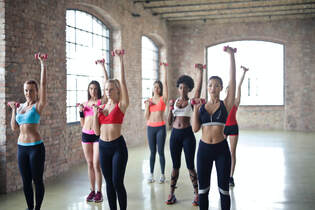|
The benefits of keeping active may seem obvious, yet it can't hurt to be reminded of the many ways exercise can improve your life. Here are a few of our favourite reasons to get moving... 1. Exercise improves energy levels.
Improving your fitness means your body is capable of achieving more for the same energy expenditure. While doing exercise can make you tired in the short term, regular improvements to your fitness will help you get more out of your body each day, with seemingly less effort. 2. Exercise can help to reduce stress. If you are stuck in a state of stress or anxiety, exercise can help you move out of it into a calmer and more relaxed state, improving your mood, concentration and sleep. There are now many studies to support this. 3. Exercise and hobbies can help you build connections and community. Making new friends as an adult can be surprisingly difficult and the importance of connection and community is being recognised more and more as being essential for overall wellbeing. Being part of a team, group or club is a great way to build confidence and meet friends as well as keeping active. 4. Exercise keeps your muscles, tendons, joints and bones healthy. Our bodies are often compared to machinery or car parts. However, there are some crucial differences between our bodies and machines, including the fact that our bodies respond to exercise by becoming stronger and healthier, rather than being worn out. As an example, one of the best ways to prevent osteoporosis is through regular high impact activity, which stimulates bone growth. 5. Exercise can help to reduce injuries. Similar to the previous point, tissues that are used regularly are stronger, more elastic and are less likely to tear or break when under stress. Regular exercise is the best way to keep your body in a healthy state and prevent injuries. Finding the right exercise for you can be tricky, your physiotherapist can help you with suggestions based on your ability and skillset if you need some help.
0 Comments
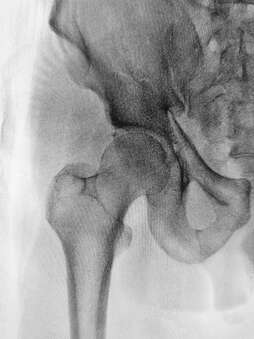
What is a stress fracture? A stress fracture is a microscopic fracture of the bone that is often not picked up on X-ray. If left untreated, a stress fracture can cause significant disability and develop into a full fracture, possibly even requiring surgery. The majority of stress fractures occur in the lower limb, being particularly common in the hip, shins and foot at points where the most force passes through when weight bearing. Most stress fractures are overuse injuries and are common in long distance runners. What are the symptoms?
As with many overuse injuries, the pain of a stress fracture starts gradually, beginning with pain during or after activity or sometimes the morning after. If activity continues without modification, the pain will gradually increase. Eventually most people are unable to maintain their usual activity level. Stress fractures are common in runners and military personnel who are required to march for long periods. A stress fracture will be more likely to occur in a person who has weaker bone strength, such as someone with osteoporosis, which is itself affected by many factors such as adequate calcium intake, vitamin D deficiency and a history of inactivity. How are stress fractures treated and how long will it take to get better? Stress fractures can easily be mistaken for other conditions such as shin splints. As the fracture is often too small to show up on X-ray, definitive diagnosis can be made using MRI, CT or bone scan. After diagnosis, the most important part of treatment will be resting the area to allow the bone to heal before resuming activity. Stress fractures usually need at least 6 weeks to recover fully. Some areas of the body have poor blood supply, which makes healing more complicated. For example, stress fractures of the navicular bone of the foot may need to be kept still and placed in a boot or cast for a period of time to heal properly. Other aspects of treatment will involve correcting any factors that contributed to the original injury. There is some evidence that unsupportive footwear is a risk factor, along with poor biomechanics and weak muscles that provide inadequate support to the skeletal system during activity. Speak to your physiotherapist if you suspect you may have a stress fracture or if you want to know more. Osteoporosis is a widespread condition characterized by low bone mass or density. It is primarily a metabolic disorder related to age and general health with a variety of risk factors and causes. The most common and well known consequence of osteoporosis is weakened bones that can break from small forces that would usually be harmless. In osteoporosis, both the matrix of the bone (similar to scaffolding) and the density of the bone are affected. While bone seems like a static part of our body, it is continuously laid down and removed by our bodies. In osteoporosis, there is an imbalance between the growth and reduction in the bone so it becomes progressively weaker. As such, it is a progressive disorder that worsens with age. While the disease process might begin much earlier, symptoms are usually only noticed over the age of 50. What are the signs and symptoms?
Often called a silent disease, many people with osteoporosis will have no idea that they have it, as there are no visible symptoms. Sometimes the first sign that an individual has osteoporosis is when the first bone breaks. Unfortunately, these bones are also slower to heal than healthy bones which can lead to ongoing complications. Broken bones are not the only symptom of osteoporosis, as bones lose density and strength they can also become compressed and develop wedge fractures under the weight of the body. When the spine is affected by osteoporosis, people may develop a hunched or stooped posture, which can itself lead to respiratory issues and place pressure on the internal organs. Osteoporosis can severely impact a person's mobility and independence, which can have a distressing impact on their overall quality of life. What causes it? As a metabolic disorder, osteoporosis can be caused by any process that interferes with the body's ability to maintain bone density. This includes gastrointestinal conditions that prevent adequate absorption of calcium (which is required for bone growth); lack of dietary calcium or low levels of vitamin D, which are essential for the absorption of calcium. Some medications can contribute to bone loss as an unfortunate side effect, especially if they are taken for a long time or in high doses. An example is the long-term use of steroids which can be prescribed to reduce inflammation. Inactivity can also predispose a person to osteoporosis as bones respond to force and weight bearing by building more bone. Having a sedentary lifestyle or choosing activities with low levels of impact can mean that without the weight bearing stimulus to make bone, bones are less dense over time. Osteoporosis can occur in elite cyclists and swimmers, who are more likely to develop the condition if they don't include weight-bearing activities such as jogging in their training program. How can physiotherapy help? Physiotherapy can help you to improve your overall bone health, and avoid or recover from fractures. Physiotherapy exercises can direct you to safely increase your weight-bearing, which can help build bone mass. Balance training is also an important factor as this can reduce your risk of falls. Your physiotherapist can also help you to adjust your lifestyle, at home or at work, to protect your bones and improve your posture, all of which are helpful in the overall management of osteoporosis. |
Categories
All
|