|
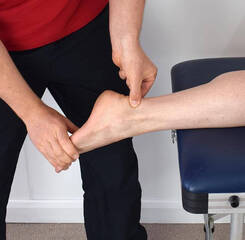
What is Sever’s Disease? Sever’s disease is a condition that causes pain in the heel of children and adolescents. While it can be quite painful, it is a self-limiting condition that doesn’t usually cause any long-term problems. Sever’s disease is quite common and is the leading cause of heel pain in children and young adolescents. Also known as calcaneal apophysitis, Sever’s disease is an inflammation of the growth plate of the heel. A growth plate is the area of bone where new bone is produced in the growing skeleton and is often weaker than other bony areas. Repeated or excessive stress on this area can cause it to become and inflamed and painful. What are the symptoms?
Children might complain of heel pain that is worse when walking, running or jumping. This may be present following an increase in activity or after a growth spurt. Pain may also be felt when walking on heels. Why does this happen? The achilles tendon attaches to the back of the heel, just next to the growth plate and puts force through this area during movement. If this force becomes too great, the growth plate can become irritated, starting a painful inflammatory process. While increased activity is a predisposing factor, other things may also contribute, such as reduced movement of the ankle, abnormal foot movements when walking and tight calf muscles. It is also possible that Sever’s disease can appear with no obvious cause. What is the treatment? While this is a self-limiting disorder that will go away on its own as the skeletal system completes growth, it can be quite painful and this may impact your child’s activity levels and gait pattern. To prevent any long-term issues from adaptations or changes in activity levels, your physiotherapist can work with your child to find solutions that allow maximum movement with minimum pain. Most of the time, simple education and relative rest or ceasing of aggravating activities are effective. Studies have also found that properly fitted orthotics can help reduce pain while maintaining activity. Physiotherapists can also address any factors which may have caused excess stress in this region, such as abnormally tight muscles or poor gait patterns. They can also advise of pain-relieving treatments and alternative forms of exercise if necessary. None of this information is a replacement for proper medical advice. Always see a medical professional for advice on your injury.
0 Comments
What is a stress fracture? A stress fracture is a microscopic fracture of the bone that is often not picked up on X-ray. If left untreated, a stress fracture can cause significant disability and develop into a full fracture, possibly even requiring surgery. The majority of stress fractures occur in the lower limb, being particularly common in the hip, shins and foot at points where the most force passes through when weight bearing. Most stress fractures are overuse injuries and are common in long distance runners. What are the symptoms?
As with many overuse injuries, the pain of a stress fracture starts gradually, beginning with pain during or after activity or sometimes the morning after. If activity continues without modification, the pain will gradually increase. Eventually most people are unable to maintain their usual activity level. Stress fractures are common in runners and military personnel who are required to march for long periods. A stress fracture will be more likely to occur in a person who has weaker bone strength, such as someone with osteoporosis, which is itself affected by many factors such as adequate calcium intake, vitamin D deficiency and a history of inactivity. How are stress fractures treated and how long will it take to get better? Stress fractures can easily be mistaken for other conditions such as shin splints. As the fracture is often too small to show up on X-ray, definitive diagnosis can be made using MRI, CT or bone scan. After diagnosis, the most important part of treatment will be resting the area to allow the bone to heal before resuming activity. Stress fractures usually need at least 6 weeks to recover fully. Some areas of the body have poor blood supply, which makes healing more complicated. For example, stress fractures of the navicular bone of the foot may need to be kept still and placed in a boot or cast for a period of time to heal properly. Other aspects of treatment will involve correcting any factors that contributed to the original injury. There is some evidence that unsupportive footwear is a risk factor, along with poor biomechanics and weak muscles that provide inadequate support to the skeletal system during activity. Speak to your physiotherapist if you suspect you may have a stress fracture or if you want to know more. |
Categories
All
|