|
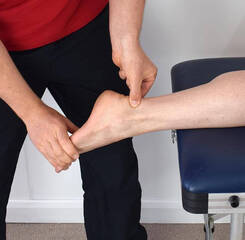
What is Carpal Tunnel Syndrome? The carpal tunnel is a small space where the wrist meets the base of the hand. This space is covered by a thick ligament and creates a small tunnel where various nerves, arteries and tendons pass through from the forearm into the hand. If anything causes this space to be reduced, these structures can become compressed or damaged, particularly the median nerve. This condition is referred to as Carpal Tunnel Syndrome. What are the symptoms?
The hallmark symptoms of carpal tunnel syndrome are pain, tingling or numbness in the hand, usually following a typical pattern over the thumb, index and middle finger. There can also be a reduction in grip strength and wasting of the thumb muscles. Symptoms are usually worse on waking or with repetitive hand movements. Patients might also report difficulty holding items, writing or doing up their buttons. How does it happen? Carpal tunnel syndrome can be caused by anything that reduces the space in the carpal tunnel, including arthritis, the growth of a cyst or compression from everyday activities. The median nerve is particularly vulnerable to compression and is of the most concern as prolonged compression can cause nerve damage and permanent weakness of the hand. How is it treated? There are a few different treatment options for carpal tunnel syndrome. Non-surgical treatment is recommended first, which could include physiotherapy, wearing a splint, cortisone or plasma rich platelet injections to promote nerve healing. The effectiveness of physiotherapy will depend on the cause of your syndrome. If the space of the tunnel has been reduced permanently, such as with arthritis, then surgery is likely to be the most effective treatment. Carpal tunnel surgery is an operation to widen and release the carpal tunnel allowing decompression. This is a common procedure but is not without risks or complications and requires a period of time off work for recovery. For non-surgical cases, altered biomechanics of the arm, the mobility of the median nerve and muscle tightness may all be contributing to symptoms. In this case, physiotherapy can be highly effective, along with a period of rest, possibly splinting and a change in your daily activities.
1 Comment
What is it? The scaphoid is a small bone in the wrist that connects the radius bone in the forearm to the hand, situated near the thumb. Scaphoid fractures are a relatively common wrist injury and are commonly misdiagnosed, as the pain can be similar to a sprained wrist, even when the bone has been broken. Scaphoid fractures are notorious for complications in healing due to low blood supply to the area and how easily their diagnosis can be missed. How does it happen?
A scaphoid fracture is often caused by a fall on an outstretched hand (FOOSH) or a direct blow to the wrist. It is more common in young adults than in children and the elderly. What are the symptoms? Symptoms of a broken scaphoid include wrist pain, swelling, bruising or discolouration of the skin over the injured area and difficulty moving the wrist or hand. As the swelling subsides you might notice pain at the base of the thumb when opening jars or gripping objects. There may also be a deep, dull ache in the wrist that doesn't settle easily. How is it diagnosed? If you suspect that you have a scaphoid fracture, you should consult your physiotherapist or GP who will refer you for an X-ray to confirm if the bone is broken. Occasionally scaphoid fractures will not show up on an X-ray, so if the findings are negative yet your medical team still suspect a fracture, they may wait a week then X-ray again or send you for an MRI or CT scan to double-check. Though these fractures can often be treated without surgery, doctors may recommend surgical intervention for more severe cases or if the bone is not healing well enough on its own. How can physiotherapy help? If you have a scaphoid fracture, your doctor will likely prescribe a splint or cast to ensure the wrist is kept still until healing is complete, usually for a minimum of six weeks. Healing times will vary depending on which part of the bone has been broken. Following the removal of the cast or splint, there is often residual pain, stiffness and muscle weakness. Your physiotherapist can help you restore any deficits as well as resolve any other aches or pains that may have resulted from altered biomechanics. Tendons, the connective tissues that join muscles to bone are known for being notoriously difficult to treat once injured. The reason for this is that often they are injured through stress or overuse, and compared to muscles they can have relatively poor blood flow, which is essential for healing. Tendons and muscles work together to move your joints and together are called a contractile unit. As muscles are exercised and gain strength, the attaching tendons are also placed under tension and adapt to this to become stronger. If the load placed on the tissues exceeds their capacity, the tendon fibres can begin to break down and become stiff and painful. Is my pain related to a tendon injury?
For an accurate diagnosis, you will need to be assessed by a physiotherapist. However, some signs that your pain might be coming from an in issue with a tendon are; · The pain is quite specific and can be felt over the tendon itself; · The pain is worse when under stress and improves when rested; · The pain improves after exercise has started, but it might be worse once you cool down; · The area around the tendon may feel stiff after periods of rest, particularly in the morning. How are tendon injuries treated? When it comes to recovery, tendons are often treated differently to other injuries. While each tendon injury is unique and will require assessment and intervention by a physiotherapist, there are a few general approaches that usually help with all tendon injuries. Reducing your activity to a comfortable level is the first step to recovery. Complete rest can actually delay healing as the tendon simply becomes weaker and less able to cope with subsequent loads. Your physiotherapist can provide you with a targeted exercise program to aid your recovery. Eccentric exercises, which are exercises that work alongside gravity, have been shown to stimulate tendon healing and strength. Stretching may aggravate your injury and should be used with caution. Assessment of any biomechanical faults or stresses that are placing undue load on the tendon is also a central component of treatment. Your physiotherapist is able to guide you with your recovery and return to sport to avoid aggravating any injury. What is a wrist sprain? Wrist sprains are a general term used to describe any injury to the wrist that doesn’t include a fracture, but is most likely to be a ligament injury. While this can indicate that they are not serious injuries, wrist sprains can be complicated injuries that require supervision and treatment to recover fully. The wrist refers to the area where the bones of the forearm, the radius and ulna, meet and join the bones of the hand. The wrist is able to twist on itself and allows the hand to move to face palm up (supination) or palm down (pronation). The hand is also able to move up and down (flexion/extension) and side to side (abduction/adduction). To allow such complicated movements, the joint surfaces of the wrist are held together by a series of ligaments. When a wrist is sprained, it is usually these ligaments that have been damaged. What are the symptoms?
The primary symptom of a sprained wrist is pain with movement of the joint or when taking load, such as when holding a heavy object. Ligament injuries are given a grading scale to indicate their severity, which can help to guide treatment. Grade 1 refers to a stretching or laxity of the ligament fibres and injuries of this grade usually heal with rest within 2-3 weeks. A grade 2 classification signifies that there has been a partial tear of the ligament fibres and will often need more time and treatment for recovery. Grade 3 tears refer to a full thickness rupture of a ligament and may require splinting or even surgery. The most common cause of a wrist sprain is a fall onto an outstretched hand. Ligament injuries can also happen gradually through over use, although this is less common. What is the treatment? Your physiotherapist is able to help diagnosis a wrist sprain and can help to rule out a fracture. An X-ray might be required and your physiotherapist will perform special tests to help identify exactly which structure has been injured, also giving the injury a grade, to help guide treatment. How can physio help? The key to effective recovery for a wrist sprain is ensuring that the right treatment protocols are in place for your particular injury. Grade 1 sprains will recover best with gentle exercises and early strengthening while Grade 2 to 3 injuries may require splinting or even a surgical consultation for repair. If surgery is the right course for you, your physiotherapist is able to guide you through this treatment pathway, helping you to prepare and recover from surgery to get the best outcome possible. |
Categories
All
|