|
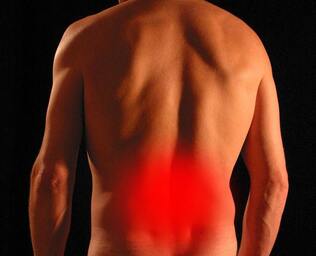
Back pain is such a common experience that it is estimated up to 80% of adults will have at least one severe episode of lower back pain in their lifetime. For many people, the pain quickly resolves and things go back to normal. However the first time this happens to you it can be scary, particularly as severe pain can occur suddenly and without warning. Statistics however are on your side. Most of the time, acute low back pain resolves without consequence and doesn’t recur. If you happen to be in the middle of an episode though, here are a few tips to help you get through.
While this may seem obvious, there are a few people who will always try to push through the pain. The expression "no pain, no gain" is in many cases outdated and if your work requires heavy lifting, it is more than reasonable to take a few days off. 2. Avoid too much rest. On the other hand, lying in bed all day is bad for you as well. If you have severe back pain, gentle movement under the advice of a physiotherapist is much better for you than complete rest. 3. Avoid long car or plane trips If possible, now is the time to avoid long distance travel. If you absolutely must travel, speak to your physiotherapist about how to manage your pain during the trip. 4. Avoid listening to horror stories There are always stories about pain that never went away, requiring surgery, which only made it worse. While worst case scenarios can happen, they are rare, and being fearful can negatively impact your recovery. That terrible story is probably not going to happen to you and hearing these stories is only going to worry you and make you feel worse! 5. Avoid delaying treatment While your pain may go away on its own, it is important to have a professional assess your condition to screen for any serious injuries and advise you on how to best manage your pain while you are getting better. They can also help you recover as quickly as possible, as well as give you advice on how to avoid future episodes. 6. Don’t expect a miracle cure Back pain is complicated and a single treatment that works for everyone simply does not exist. It is important to follow the directions of your therapist and work with them to set reasonable and realistic goals for your recovery. None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual injury.
3 Comments
Referred pain is one of the most complicated processes in the human body. You may have experienced this if you ever saw a physiotherapist for pain in one part of your body, and they started to treat an entirely different area. The complexity of pain is one of the reason's why physiotherapists conduct such a thorough interview with you and physical examination before being able to determine the exact source of your pain. Why is pain so complicated?
Unfortunately, we still don't understand everything about the way pain is processed. Usually, when an injury or damage occurs to body tissues, a signal is sent to the brain, which begins to interpret this signal and creates the sensation of pain. Pain is thought to be a warning signal to let you know to avoid danger and pay attention to the injured body part. Occasionally this system goes a little haywire, and pain signals are sent when there is no damage or the location of the pain is misdirected. Referred pain is the term used when pain is felt at a different location to the source of the problem that is sending the pain signal. There are many kinds of referred pain, and some are easier to explain than others. What are the different types of referred pain? In some cases, if it is a nerve that is sending the pain signal, then pain can be felt all along the length of the nerve. This may be described as a sharp burning pain along the skin. One of the most common examples of this is "sciatica", where the large nerve that runs down the back of the leg is irritated around the lower back or buttock. The source of the pain signal is near the spine. However, that pain follows a distinctive pattern down the leg. In other cases, it is the muscles and not the nerves that are referring pain elsewhere. Muscular trigger points are taut bands that develop within muscle tissue that is undergoing abnormal stress. Poor posture, lack of movement, and overuse can cause muscles to develop areas of dysfunction. These trigger points can cause pain that radiates out in distinctive patterns. Trigger points are diagnosed as the source of pain if symptoms are reproduced when a therapist presses on a specific point. If that wasn't confusing enough, we know that our internal organs can also refer pain. Pain referred by internal organs may be described as a deep ache, and usually not influenced by movements of the limbs or back. Organs often distribute pain in patterns that are very obscure and sometimes don't even create any pain at their own location. For example, kidney pain can feel like lower back pain. There are many other fascinating aspects to pain and understanding how it works is an important part of managing your symptoms. To understand how referred pain may be affecting you, talk to your physiotherapist who can help with any questions. None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual injury. |
Categories
All
|