|
Joint and/or muscle stiffness can be felt in any part of the body. While it may be accompanied by pain, this is not always the case and it can have many different causes. Feelings of stiffness can be easy to ignore, however, they can be a sign that you're at increased risk of injury or pain. Here are a few reasons why you might be feeling a little bit less flexible... Muscle Weakness
Muscle stiffness can be a sign that strength is lacking. Our body will prioritise stability over flexibility if our muscles don't have the ability to provide both. This means that your muscles will be a bit tighter and stiffer to compensate for any weakness. If you are feeling a tight and sore, your physiotherapist can help to identify any muscles that maybe need targeted strengthening to help. Delayed Onset Muscle Soreness (DOMS) Many of us are familiar with post-exercise pain and stiffness. This is a somewhat protective mechanism to help you recover from a bout of increased exercise. This kind of stiffness will be present in muscles that have been used recently and usually lasts for just a day or two. DOMS usually goes away on its own, although it can be quite uncomfortable, it is usually nothing to be too concerned with. Your physiotherapist can help you with tips to avoid DOMS in your regular workouts. Lack of movement Along with muscle weakness, inactivity can lead to joint stiffness. Joints need to move through their full range regularly to maintain their flexibility, as anyone who has kept a joint immobilised in a plaster cast will know! Lack of movement can lead to a reduction of blood flow and nutrients, also impacting joint health. Your physiotherapist can help you to identify any joints that are not moving well and advise you on how to restore joint flexibility. Activities such as Pilates aim to help you move all of your joints through their full range safely and maintain flexibility. Arthritis Stiffness is the hallmark of arthritis, often noticeable as increased stiffness on waking that progresses gradually over time. Pain and stiffness caused by arthritis can often be helped by a targeted muscle strengthening program to help support the joints. Speak to your physio about any tightness or inflexibility and see how they can help you feel your best.
0 Comments
One of the most impressive healthcare developments in history is the joint replacement. Many people are able to take out a joint that is extremely painful and dysfunctional and give it a whole new lease on life with a surgically inserted prosthesis. The improvements in this type of surgery over recent years have meant that success rates for joint replacement surgery, particularly hip and knee replacements are higher than ever. If you are struggling with joint pain related to arthritis, it can be difficult to know when to start thinking seriously about surgery. Here are a few things to consider before going for that surgical opinion... Don't assume pain is permanent once you hear the word arthritis
Pain is complex and is often not caused by one single thing. Most people will have some amount of arthritis in their joints past the age of 50, whether or not this is what is causing your pain will be unclear without first seeking assessment and treatment. Many people have some level of degeneration in their joints without experiencing much discomfort at all, as a normal part of the ageing process. It's possible that a combination of strengthening and manual therapy could improve your symptoms significantly, even if osteoarthritis is present. A trial of physiotherapy is recommended before surgery in most cases. Pre-surgical strength and fitness are important This means two things. First of all, your strength before surgery will set you up for much better post-operative results. The second thing is that choosing when to have the surgery means not necessarily waiting until the pain is unbearable before going ahead, as time spent in significant pain can reduce your overall strength and fitness while also putting more stress on other joints. Research the risks and side effects While surgical outcomes are continually improving, no surgery comes without risks and some people will have ongoing pain and stiffness even after their operation. It is important to make an informed decision about when and if you should have a joint replacement. If you are considering a joint replacement, speak to your physiotherapist about all the ways they can support you through your journey and help you come to an informed decision about what is right for you. The decision to have surgery following an injury is a serious and complicated one. It can be difficult when navigating the minefield of information you receive to know what is the right pathway for you. Unfortunately, the answer is not always obvious which can be confusing. To ensure that surgery is right for you, here are a few questions it pays to ask yourself and your medical team before making a decision. How much will surgery cost and will I need to take time off work?
One of the major downsides of surgery is that you will often need to take time off work to recover, resulting in lost income. The cost of the surgery itself may not be completely covered by your insurance, particularly for elective procedures and you will often need to have physiotherapy afterwards. The cost of surgery can really add up, and if you can achieve similar results with physiotherapy alone, you might find yourself in a much better financial situation. What are the potential complications and success rates for your surgery? All surgeries come with risks and potential complications, the probability of these will vary depending on the type of surgery, your age and general health. It is also important to compare the success rates of surgery with a period of physiotherapy treatment. Optimal surgical outcomes still often depend on effective post-surgery management, which can be an argument for considering physiotherapy first. In some cases, however, healing simply will not occur without surgical intervention and physiotherapy will have little success in resolving the issue. What are your post-surgical goals? Not everyone wants to ski down a mountain, but for some, being able to push and trust their bodies is important for both their income and quality of life. Surgery that aims to repair damaged structures might be the right decision for someone who has high demands on their body, but not for another person who isn't very active. Setting your goals for your body can help to guide your decision making process. Before making any major decisions, it is important to consult your medical, surgical and physiotherapy team to ensure you are well educated in all the risks and rewards of undergoing surgery. The "socket" of the shoulder joint is surrounded by a ring of flexible connective tissue, known as a labrum. This labrum increases the stability of the shoulder while allowing the joint to stay flexible. The long head of the biceps tendon has an attachment directly into the labrum, which is often a point where injuries occur. A tear of the labrum can occur in many locations, however the most common is at the point where the biceps tendon attaches. Usually, this tear follows a typical pattern and is referred to as a superior labrum tear, anterior to posterior (SLAP tear). How do they happen?
SLAP tears can be caused by trauma such as a fall onto an outstretched hand or can develop over time through repeated stress. Repetitive overhead activities such as throwing or painting can also gradually weaken the labrum over time and lead to a tear. What are the symptoms? Often if a SLAP tear develops over time, patients can be unaware they have sustained an injury at all and there is no significant impact on their pain or function. Pre-existing SLAP tears can however place more tension on the long head of the biceps tendon, leading to overuse disorders of that tendon as a secondary complication. When the tear occurs through a sudden action or trauma, symptoms can be more noticeable. Patients often notice pain deep in the shoulder joint with overhead shoulder movements, a feeling of weakness or a loss of power or accuracy with throwing activities. Some people may feel a popping or clicking sensation and occasionally the shoulder feels like it "gives way". In severe tears, the shoulder might feel unstable and be at increased risk of dislocation. How can physiotherapy help? Your physiotherapist can help diagnose a SLAP tear and send you for scans if needed. SLAP tears are graded by severity from 1 to 4 as a way to guide treatment. Physiotherapy is usually recommended as a trial for all tears before considering surgical repair and in many cases can effectively help patients return to their previous activities, symptom free. If physiotherapy is unsuccessful, surgical repair with a full rehabilitation program is then recommended. Surgery will either repair the tear or reattach the biceps tendon to the humerus (tenodesis). Following surgery, a period of rest in a sling is required before rehabilitation can begin. What is Ankylosing Spondylitis? Ankylosing Spondylitis (AS) is a type of inflammatory, autoimmune arthritis that primarily affects the spine. It is characterised by intermittent pain and progressive stiffness due to the inflammation and eventual hardening of the ligaments that surround the spine. The classic early symptoms of AS are pain and stiffness of the sacroiliac joints, the joints connecting the pelvic bones to the sacrum in the lower back. In the more severe, final stages of the disease, the entire spine can become fused and rigid, often in a flexed, forward posture. As this is an inflammatory disorder, many other systems and joints can also affected. A significant number of people with AS also suffer from irritable bowel syndrome and inflammation of the eye. What causes it?
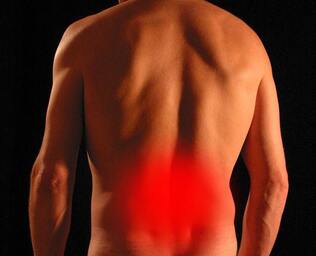
The cause of Ankylosing Spondylitis is not clear, however there are markers and predisposing factors that may contribute to the development of the condition. Genetics, chronic stress and frequent gastrointestinal infections are among the predisposing factors. Men are affected more often than women and symptoms usually begin between the ages of 17 and 45 years. What are the signs and symptoms? Intermittent back pain and progressive stiffness are the two most common symptoms of Ankylosing Spondylitis. Other tendons and ligaments may be affected, including those in the hands, feet and ribs. Symptoms tend to be worse following periods of rest, particularly first thing in the morning and improve following periods of activity. It is common for people to experience “flare-ups” and “remissions” of symptoms. Some people with AS may experience mild discomfort in the spine from time to time, while others may experience severe and debilitating symptoms at frequent intervals with minimal time in remission. Long term issues with AS include breathing difficulties due to thoracic and rib cage stiffness and severe spinal pain and immobility. Medical treatment focuses on reducing inflammation and slowing the disease process. How can physiotherapy help? Physiotherapy treatment aims to manage pain during flare-ups and maintain optimal posture as the disease progresses. Your physiotherapist will assess your spinal movement and posture as well as strength. If your hands, feet, hips or shoulders are affected, they will also provide you with specific exercises to help maintain mobility and strength in those joints. Many studies have proven the positive benefits of exercise for those with Ankylosing Spondylitis, such as improved rib cage expansion when breathing, and improved posture of the upper back and neck. While pain and stiffness often go together, joint stiffness can occur on its own. Joint stiffness can limit your ability to perform usual tasks, such as turning your head to check behind you while driving. Stiffness can also be a warning sign that a part of the body is vulnerable to future injury. There are many different causes of stiffness and below are some of the reasons why you might not be feeling as flexible as normal. 1. Disuse and lack of movement
Our bodies are designed to move. When we're not regularly moving our joints through their full range, they can begin to feel ‘tight’. This can be caused by a combination of the capsule that surrounds the joint tightening up and the muscles around the joint shortening and losing flexibility. Stiff and tight muscles can cause you to feel as though your joints are stiff, even if it is only the muscle length that is restricting the movement. Joint mobilizations, manipulation and muscle stretches or massage can have a significant effect in improving the symptoms. The most effective way to maintain full movement is to regularly move joints through their full range, which also helps to keep muscles and joints healthy. Your physiotherapist can advise you on how to best approach this with a targeted set of exercises. 2. Osteoarthritis (OA) OA is a degenerative disease, characterized by a breakdown of the joint surface cartilage and the growth of bony osteophytes around areas of stress. While OA is increasingly common as we age, it is thought that the primary cause is abnormal load and stress to joint surfaces and not simply aging itself. As the space between two joint surfaces become uneven, joints affected by OA can feel stiff or even ‘blocked’. A person with OA will often feel stiff for around 15-20 minutes after being still. Physiotherapy programs to strengthen the muscles surrounding the joints, to help absorb weight-bearing forces, has been shown to have positive results with OA symptoms. 3. Inflammatory Related Stiffness The inflammatory process is characterized by swelling and pain around a specific area. Usually this is a response to damage by the body. As an area swells, this will allow less space for movement and a sensation of stiffness, as anyone who has had sprained an ankle can attest to. Acute inflammation will cause swelling that increases over 24-48 hours and subsides gradually. Autoimmune disorders can cause the body to mistakenly have an inflammatory reaction where there has been no injury, with resulting pain and stiffness. Rheumatoid arthritis and ankylosing spondylitis are two examples of such disorders. Stiffness caused by inflammatory disorders is characterized by a feeling of stiffness after rest, particularly in the morning, that can take longer than 30 minutes to subside. Inflammatory disorders unrelated to injuries are complex in cause and require collaboration with medical teams for best treatment outcomes. Acute injuries are best managed by following RICE protocols (Rest, Ice, Compression, Elevation). |
Categories
All
|