|
Almost everyone will experience lower back and/or neck pain at some point in their lives, even if just in the form of a slight neck twinge after sleeping in an odd position. Spinal pain of the thoracic region (the upper & middle part of your back) is less common, however you might be surprised to discover how important this part of the body can be when it comes to pain and injury. What is it?
The thoracic region refers to the part of the spine that is surrounded by the rib cage. It consists of 12 vertebrae with discs that sit between each of them. The thoracic spine isn’t an area that you might associate much with movement, however, this area can account for a surprising amount of flexibility, particularly in rotation. With joint attachments both between each side of the 12 vertebrae and a rib on either side, the thoracic spine has almost more individual joints than you can count. If each of these joints is not regularly moved through their full range they can tighten up and lose flexibility. This stiffness can become quite significant over time. Why is it important? Many people may not even notice this lack of movement, primarily because the neck and lower back provide much more range and can usually compensate for any loss of thoracic flexibility to complete everyday tasks. When there is no movement occurring in the thoracic region, this means that the structures of the joints in other regions are pushed closer to their limits of range, particularly during rotation. This results in more compression and stress on these joints and the structures surrounding them, such as nerves, blood vessels and muscles. Thoracic stiffness can be a significant risk factor for neck and lower back pain. This can also reduce the mobility of the chest wall, which can result in less efficient breathing mechanics and, in extreme cases, even reduced exercise tolerance. Thoracic spine movement is aslo important for normal shoulder function, as well as maintaining good posture. How can physiotherapy help? Your physiotherapist is able to assess your thoracic mobility and help you with treatments to improve your range, both with manual therapy and home exercises. They may even help improve your thoracic flexibility as part of a treatment plan for neck and lower back pain.
0 Comments
Joint and/or muscle stiffness can be felt in any part of the body. While it may be accompanied by pain, this is not always the case and it can have many different causes. Feelings of stiffness can be easy to ignore, however, they can be a sign that you're at increased risk of injury or pain. Here are a few reasons why you might be feeling a little bit less flexible... Muscle Weakness
Muscle stiffness can be a sign that strength is lacking. Our body will prioritise stability over flexibility if our muscles don't have the ability to provide both. This means that your muscles will be a bit tighter and stiffer to compensate for any weakness. If you are feeling a tight and sore, your physiotherapist can help to identify any muscles that maybe need targeted strengthening to help. Delayed Onset Muscle Soreness (DOMS) Many of us are familiar with post-exercise pain and stiffness. This is a somewhat protective mechanism to help you recover from a bout of increased exercise. This kind of stiffness will be present in muscles that have been used recently and usually lasts for just a day or two. DOMS usually goes away on its own, although it can be quite uncomfortable, it is usually nothing to be too concerned with. Your physiotherapist can help you with tips to avoid DOMS in your regular workouts. Lack of movement Along with muscle weakness, inactivity can lead to joint stiffness. Joints need to move through their full range regularly to maintain their flexibility, as anyone who has kept a joint immobilised in a plaster cast will know! Lack of movement can lead to a reduction of blood flow and nutrients, also impacting joint health. Your physiotherapist can help you to identify any joints that are not moving well and advise you on how to restore joint flexibility. Activities such as Pilates aim to help you move all of your joints through their full range safely and maintain flexibility. Arthritis Stiffness is the hallmark of arthritis, often noticeable as increased stiffness on waking that progresses gradually over time. Pain and stiffness caused by arthritis can often be helped by a targeted muscle strengthening program to help support the joints. Speak to your physio about any tightness or inflexibility and see how they can help you feel your best. For most of us, screen time and sitting go hand in hand and both are only increasing as our lives move more online. While short periods in any posture aren't harmful, a lack of movement combined with long periods spent in hunched positions can lead to spinal pain, headaches, shoulder pain and more. If you're needing to spend more time in front of a screen, here are a few tips that can help you to keep flexible and avoid pain. Set movement breaks
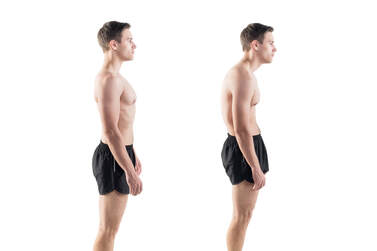
Posture in itself isn't always a problem. Spending long periods of time in these postures without taking breaks is the problem. When your body is so used to one position, muscles may become shorter and joints stiffer, making it harder to move out of this posture without pain and discomfort. You can break up your day by setting a timer to move and take a break every 20-30 minutes. Using these short breaks for movement is a great way to both help focus at work and keep your body more flexible. Setup your work and home environment properly Adjusting your work station or setting up a place to relax at home where to you can avoid a hunched posture can help you to reduce time in the same posture. Your physiotherapist can give you tips for how to setup your home and office environment correctly. Take stock of your time spent sitting Time in the car, time on your computer and time on the couch can all quickly add up without you realising. By accounting for the amount of time you spend sitting, you can find more ways to move. For example, if you notice that you're sitting down as soon as you get home, try swapping out watching an episode on TV to going for a walk while listening to a podcast. Ask your physio for specific stretches If you can identify the posture you spend the most time in, your physio can help you to develop a specific exercise and stretching program to counteract these positions most directly and keep you strong and flexible. For most of us, the hours we spend sleeping are simply a time for rest and recovery. However, you might be surprised to learn that your sleeping position can have a significant impact on your body, particularly if you already have an injury. Here are some tips to help to stay pain free overnight. Back pain tips:
For sufferers of back pain, finding a comfortable position at night can be difficult. The natural curves of the spine need to be maintained and supported throughout the night. Ideally, your body should be held in a position of minimal stress while sleeping. This means that all your joints and muscles are resting in a neutral position A mattress that is too soft might feel comfortable to begin with, but over time will let you sink into it too much, meaning the curve of the lower spine will be lost. Waking up with a stiff or sore back could be a sign that you are using the wrong mattress. A mattress that is too firm can also mean your spine is held in a flattened position, which is both uncomfortable during the night and when you wake up. For many people, sleeping on their side keeps their spine in a more natural alignment than sleeping on their back, especially if they put a pillow between your knees. If you do sleep on your back, placing a pillow under your knees can help to maintain your lumbar spinal curve throughout the night. This can also help to reduce hip and knee pain. Neck pain tips: The neck is often the most vulnerable part of the body if your sleeping setup is not ideal. Side sleepers may let their neck fall excessively to the side with a pillow that is too low or have their neck elevated too much by having their pillows too high. If you find yourself putting your arm under your pillow while you sleep, it is likely that your pillow is too low. Having your shoulder in this position overnight can put unnecessary stress on the structures around the shoulder joint and should be avoided if possible. Stomach sleeping can also put additional pressure on your neck as it is turned to the side for long periods. Hip pain tip: Side sleepers often spend their nights with one leg crossed over their body. This can place extra pressure on the structures on the side of the hip, such as tendons and bursa and can impact the health of these tissues as the compression reduces the blood flow to the area. Placing a pillow under your knee while sleeping on your side in this position can help to maintain a neutral alignment of your hip. Speak to your physiotherapist for more advice on how to improve your sleeping posture and find out if your sleeping setup is right for you. We know that office life can wreak havoc on our body. Even with the best intentions, finding time to reverse the pressures of 8 hours a day sitting in a chair can be difficult. Here are three easy stretches to do daily that focus on common problem areas for office workers. Chest & shoulders stretch (wall angels):
Find a large flat wall and stand facing away from it. You may need to bend your knees slightly or step a few inches forward. Your pelvis, upper back and back of your head should all be in contact with the wall, with small gaps where the curves of your spine are. If you are unable to keep your head to the wall, you may need to use a towel behind your head to make this position comfortable. Tuck your chin in gently, keep your palms facing forward, elbows bent to ninety degrees with the backs of your arms against the wall. Now slide your arms up along the wall, as high as you can while keeping them in contact with the wall, pause for a few seconds and slide them down again. Repeat 5 to 10 times. This will stretch your chest and shoulder muscles which get tight from slouching at a desk, as well as help you to develop a sense of head position alignment with your body. Hip flexor stretch (lunge): Kneel on one knee, place your other foot on the floor in front of you and keep your knee bent to 90 degrees. Keeping your hips even, shift your pelvis forward but keep your shoulders back until you feel a stretch at the front of your hip of the kneeling leg. Hold for 30 to 45 seconds and then swap legs. Repeat 2 to 3 times. This will stretch your hip flexor muscles which are often tight from sitting for long periods. Seated hamstring stretch: Sit on the floor with one leg straight out in front of you. Bend your other leg and tuck your foot in towards your inner thigh. Reach forward with both hands and stretch towards your foot on the straightened leg, bending at your hips as much as possible. You should feel a stretch at the back of your thigh, if you feel a pull behind your knee you can point your toes or bend your knee slightly. Hold for 30 seconds and slowly come back up, change legs and repeat 2 to 3 times on each leg. Check with your physiotherapist if there are other stretches that may benefit you. What is Ankylosing Spondylitis? Ankylosing Spondylitis (AS) is a type of inflammatory, autoimmune arthritis that primarily affects the spine. It is characterised by intermittent pain and progressive stiffness due to the inflammation and eventual hardening of the ligaments that surround the spine. The classic early symptoms of AS are pain and stiffness of the sacroiliac joints, the joints connecting the pelvic bones to the sacrum in the lower back. In the more severe, final stages of the disease, the entire spine can become fused and rigid, often in a flexed, forward posture. As this is an inflammatory disorder, many other systems and joints can also affected. A significant number of people with AS also suffer from irritable bowel syndrome and inflammation of the eye. What causes it?
The cause of Ankylosing Spondylitis is not clear, however there are markers and predisposing factors that may contribute to the development of the condition. Genetics, chronic stress and frequent gastrointestinal infections are among the predisposing factors. Men are affected more often than women and symptoms usually begin between the ages of 17 and 45 years. What are the signs and symptoms? Intermittent back pain and progressive stiffness are the two most common symptoms of Ankylosing Spondylitis. Other tendons and ligaments may be affected, including those in the hands, feet and ribs. Symptoms tend to be worse following periods of rest, particularly first thing in the morning and improve following periods of activity. It is common for people to experience “flare-ups” and “remissions” of symptoms. Some people with AS may experience mild discomfort in the spine from time to time, while others may experience severe and debilitating symptoms at frequent intervals with minimal time in remission. Long term issues with AS include breathing difficulties due to thoracic and rib cage stiffness and severe spinal pain and immobility. Medical treatment focuses on reducing inflammation and slowing the disease process. How can physiotherapy help? Physiotherapy treatment aims to manage pain during flare-ups and maintain optimal posture as the disease progresses. Your physiotherapist will assess your spinal movement and posture as well as strength. If your hands, feet, hips or shoulders are affected, they will also provide you with specific exercises to help maintain mobility and strength in those joints. Many studies have proven the positive benefits of exercise for those with Ankylosing Spondylitis, such as improved rib cage expansion when breathing, and improved posture of the upper back and neck. While pain and stiffness often go together, joint stiffness can occur on its own. Joint stiffness can limit your ability to perform usual tasks, such as turning your head to check behind you while driving. Stiffness can also be a warning sign that a part of the body is vulnerable to future injury. There are many different causes of stiffness and below are some of the reasons why you might not be feeling as flexible as normal. 1. Disuse and lack of movement
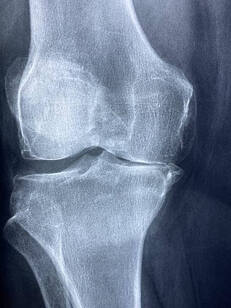
Our bodies are designed to move. When we're not regularly moving our joints through their full range, they can begin to feel ‘tight’. This can be caused by a combination of the capsule that surrounds the joint tightening up and the muscles around the joint shortening and losing flexibility. Stiff and tight muscles can cause you to feel as though your joints are stiff, even if it is only the muscle length that is restricting the movement. Joint mobilizations, manipulation and muscle stretches or massage can have a significant effect in improving the symptoms. The most effective way to maintain full movement is to regularly move joints through their full range, which also helps to keep muscles and joints healthy. Your physiotherapist can advise you on how to best approach this with a targeted set of exercises. 2. Osteoarthritis (OA) OA is a degenerative disease, characterized by a breakdown of the joint surface cartilage and the growth of bony osteophytes around areas of stress. While OA is increasingly common as we age, it is thought that the primary cause is abnormal load and stress to joint surfaces and not simply aging itself. As the space between two joint surfaces become uneven, joints affected by OA can feel stiff or even ‘blocked’. A person with OA will often feel stiff for around 15-20 minutes after being still. Physiotherapy programs to strengthen the muscles surrounding the joints, to help absorb weight-bearing forces, has been shown to have positive results with OA symptoms. 3. Inflammatory Related Stiffness The inflammatory process is characterized by swelling and pain around a specific area. Usually this is a response to damage by the body. As an area swells, this will allow less space for movement and a sensation of stiffness, as anyone who has had sprained an ankle can attest to. Acute inflammation will cause swelling that increases over 24-48 hours and subsides gradually. Autoimmune disorders can cause the body to mistakenly have an inflammatory reaction where there has been no injury, with resulting pain and stiffness. Rheumatoid arthritis and ankylosing spondylitis are two examples of such disorders. Stiffness caused by inflammatory disorders is characterized by a feeling of stiffness after rest, particularly in the morning, that can take longer than 30 minutes to subside. Inflammatory disorders unrelated to injuries are complex in cause and require collaboration with medical teams for best treatment outcomes. Acute injuries are best managed by following RICE protocols (Rest, Ice, Compression, Elevation). |
Categories
All
|