|
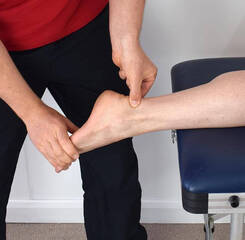
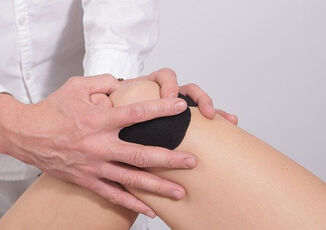
What is it? Our knees are complex hinge joints, designed to provide stability from side to side and smooth movement forwards and back as you walk, kick and run. The patella, or kneecap, is a small bone embedded in the tendon of the quadriceps muscle that protects the knee and also provides extra leverage to the quadriceps, amplifying their strength. The patella moves up and down in a groove at the front of the knee as the knee bends and straightens. Usually this movement is smooth, with little friction, however, if something causes the patella to move in a dysfunctional way, the soft tissue between the kneecap and the knee can become irritated, causing pain in a typical pattern. This condition is often referred to as ‘runner’s knee’, PFJ syndrome or patellofemoral pain syndrome (PFPS). What causes it?
The patella usually sits in a balanced position in the shallow groove at the front of the knee and moves easily without friction. The patella is attached to the quadriceps muscle at the top and connected to the lower leg via the patella tendon at the bottom. When the quadriceps contracts, this pulls on the patella and acts to straighten the knee. If one side of the quadriceps is stronger or tighter than the other, it can cause the kneecap to pull to one side and over time become irritated. There can be many factors that cause a muscle imbalance or weakness on one side of the quadriceps. In most people, the outer aspect of the quadriceps tends to be stronger and tighter than the inner muscle. Certain postures and leg positions require the outer muscles to work harder and the inside muscles to become less active. Lack of arch support in your feet or simply a physical abnormality of the knee can also place stress on the movement of the patella. What are the symptoms? This condition is characterized by pain felt on the inside or behind the patella with activities that require repetitive bending of the knee. There may be a sensation of crunching, clicking or grinding and some people report that their knee suddenly gives way. The pain is commonly felt when running, going up and down stairs or when doing squats and is generally relieved with rest. The pain may start as a small niggle and gradually become worse over time. How can physiotherapy help? The first step in effective treatment is to exclude any other conditions and have a physiotherapist confirm the diagnosis. Your physiotherapist is able to determine which factors are contributing to this condition, which could include poor posture, a lack of arch support in your feet or poor running technique. Once these factors have been identified, you will be provided with a specific treatment program to best approach your condition. PFJ syndrome usually responds well to biomechanical analysis and correction of any muscular weakness and imbalance. Having the correct shoes and orthotics can also make a huge difference. There are some short-term treatments, such as patella taping, dry needling, trigger point therapy and ultrasound, which may help alleviate symptoms quickly and keep you active while you address the other factors contributing to your pain.
0 Comments
One of the most impressive healthcare developments in history is the joint replacement. Many people are able to take out a joint that is extremely painful and dysfunctional and give it a whole new lease on life with a surgically inserted prosthesis. The improvements in this type of surgery over recent years have meant that success rates for joint replacement surgery, particularly hip and knee replacements are higher than ever. If you are struggling with joint pain related to arthritis, it can be difficult to know when to start thinking seriously about surgery. Here are a few things to consider before going for that surgical opinion... Don't assume pain is permanent once you hear the word arthritis
Pain is complex and is often not caused by one single thing. Most people will have some amount of arthritis in their joints past the age of 50, whether or not this is what is causing your pain will be unclear without first seeking assessment and treatment. Many people have some level of degeneration in their joints without experiencing much discomfort at all, as a normal part of the ageing process. It's possible that a combination of strengthening and manual therapy could improve your symptoms significantly, even if osteoarthritis is present. A trial of physiotherapy is recommended before surgery in most cases. Pre-surgical strength and fitness are important This means two things. First of all, your strength before surgery will set you up for much better post-operative results. The second thing is that choosing when to have the surgery means not necessarily waiting until the pain is unbearable before going ahead, as time spent in significant pain can reduce your overall strength and fitness while also putting more stress on other joints. Research the risks and side effects While surgical outcomes are continually improving, no surgery comes without risks and some people will have ongoing pain and stiffness even after their operation. It is important to make an informed decision about when and if you should have a joint replacement. If you are considering a joint replacement, speak to your physiotherapist about all the ways they can support you through your journey and help you come to an informed decision about what is right for you. A diagnosis of osteoarthritis (OA) for joint pain can be a cause of distress. Many people believe that if you have arthritis your pain is not able to improve and will deteriorate until a joint replacement needs to be performed. The truth is much more complicated, due in part to our bodies’ incredible ability to adapt and change. Physiotherapists have always known that the pain and disability that comes with arthritis can be improved with a targeted exercise program. In some cases, the pain that is attributed to OA is actually due to a different, entirely treatable cause. In other cases, strengthening the musculature around the painful joint can have a significant effect by providing the joint with extra support.
The way we move is often affected negatively by pain and this in itself can create changes to biomechanics that can further contribute to pain. In some cases, surgical intervention is the best choice for treatment and can have incredible results. However, there is a strong case for seeking physiotherapy treatment first to see if you can achieve the same results without surgery. Even if you do choose to go ahead with surgery, working with a physiotherapist beforehand can provide better outcomes. Physiotherapists are highly skilled at identifying exactly what is causing your pain and helping you reach the highest level of function. While exercise is a very powerful treatment, it’s not just any exercise that will take away your pain. To be effective, you will need to have a full assessment and a personalised treatment program created by your physiotherapist. This can involve identifying weak muscles, limitations in flexibility, finding painful trigger points, restoring movement to stiff joints and providing a biomechanical assessment to make a combination of changes that can make a large difference to your pain and activity levels. Your physiotherapist can also identify any other external factors that may be contributing to your pain such as unsupportive footwear, workplace set up etc. Talk to us to see how we can help you manage your osteoarthritis. Running is a great way to stay in shape, manage stress and increase your overall health. However, it’s not without potential drawbacks. While generally being a low-risk activity, there are a few injuries that commonly affect runners. As running is a repetitive impact activity, injuries can develop slowly and if left too long, then be difficult to treat. Here are three of the most common conditions faced by runners... 1. Runner’s Knee:
Runner's knee is a persistent pain on the inside of the knee caused by the dysfunctional movement of the knee-cap during movement. The knee-cap ideally sits in the centre of the knee and glides smoothly up and down as the knee bends and straightens, in a process described as tracking. If something causes the kneecap to track abnormally, the surface underneath can become worn, irritated and painful. The pain might be small to start with, however left untreated, can make running too painful to continue. 2. Shin Splints: Shin splints (medial tibial stress syndrome) is a common condition characterised by a recurring pain on the inside of the shin. While the cause of this condition is not always clear, it is usually due to repeated stress where the calf muscles attach to the tibia (shin bone). Why this becomes painful is likely due to a combination of factors that can be identified by your physiotherapist to help you get back on track as soon as possible. 3. Achilles Tendonitis (tendinopathy): The achilles tendon is the thick tendon at the back of the ankle that attaches the calf muscles to the heel bone. The amount of force that this tendon can absorb is impressive and is vital in providing the propulsive force needed for running. If the stresses placed on the tendon exceed its strength, the tendon begins to break down and become painful. Your physiotherapist is able to assess any factors that may contribute to this issue, including footwear, training errors and any biomechanical concerns. What is it? Your knee moves freely backwards and forwards; however, the thought of it moving from side to side probably makes you cringe. This is because the knee joint has sturdy ligaments either side of it that prevent sideways movement and we instinctively know that a lot of force would be required to shift it in this direction. The ligaments on either side of the knee are called the collateral ligaments and they each work to provide stability and restrict the knee’s movement into a sideways direction. The medial collateral ligament (MCL) is found on the inside of the knee and acts to prevent the knee bending inwards towards your other leg. How does this injury occur?
The typical mechanism for this injury is a force that drives the lower leg inwards. This can occur from an awkward landing from a height, or when twisting with a foot fixed on the ground or from an external force hitting the outside of the knee, such as with a football or rugby tackle. What are the symptoms? MCL tears typically create pain and swelling quite specifically on the inside of the knee. The severity of the pain and swelling will be related to the amount of ligament fibres damaged. Larger tears may also make the knee feel unstable or loose. A grading system is used to classify the severity of the injury and help to guide treatment. Grade 1 indicates that a few ligament fibres have been torn and grade 3 is used for a complete tear of the ligament with associated joint laxity. Very severe MCL tears may also involve injury to the medial meniscus and anterior cruciate ligament (ACL) and can require surgical repair. However, most MCL sprains can be managed well with physiotherapy. Grade 1 and 2 MCL sprains take between 3-8 weeks to fully heal and a complete rehabilitation program is strongly recommended to prevent future injury. How can physiotherapy help? In the early stages of the injury, treatment is focused on pain and swelling management, while allowing the body to start the healing process. This is best managed thought the R.I.C.E. principles (Rest, Ice, Compression and Elevation). Following any injury, it is natural for muscles to waste a little and the damaged tissues to lose what we call proprioception, the ability to sense their position in space. This loss of muscle strength and proprioception can contribute to future injury if not restored with a proper rehabilitation program. Physiotherapy also aims to restore movement to the joint and support the ligament while healing to ensure that it is strong and healthy, and the scar tissue forms in an organized fashion, which makes the new ligament as strong as it can be and protects against future tears. A serious injury of the knee is a tearing of the ACL (Anterior Cruciate Ligament). This ligament is important for stability of the knee and may need to be repaired surgically. The primary function of the ACL is to keep the bottom surface of the knee joint from sliding forwards during movement. An unrepaired knee may feel unstable or give way suddenly. Not all ACL injuries require surgery and some may heal well with proper rehabilitation, however for those who do need surgery, there is a significant rehabilitation period afterwards. What does the surgery consist of?
Each surgeon will have a slightly different technique for surgery. The most common approach is the arthroscopic approach, which uses a small camera and allows the surgeon to make only small incisions into the knee. They will then replace the torn ligament with either a graft from a tendon or ligament at another part of the body or using a synthetic graft. How long does rehabilitation take? Full rehabilitation following surgery can take 9 to 12 months and is divided into different stages. As surgeons can have different protocols for their approaches to surgery, time frames will vary for everyone. Initially after surgery, the graft will be quite weak while a new blood supply is being established. It can take up to 12 weeks before the graft is at its strongest point and evidence suggests that it may never have the strength of the original ligament. In the early stages, rehabilitation will be focused on restoring movement to the joint and strengthening the muscles around the knee without putting any undue stress on the graft. As the graft begins to heal and strengthen, rehabilitation can progress to include stability and control exercises and gradually build up to a complex program that prepares the knee for a full return to sport. The path to full rehabilitation from a knee reconstruction can be a long and bumpy one, however, there are high success rates with this surgery, particularly when followed up with full physiotherapy rehabilitation. The knees function as hinges, allowing your legs to swing forwards and backwards smoothly as you walk, kick and run. The knee cap (the patella) sits at the front of the knee and has a variety of functions, including guiding the muscles that straighten the knee, protecting the knee joint and absorbing forces when the knee is bent. When something goes wrong and the patella doesn’t glide up and down smoothly, the soft tissue between the kneecap and the knee can become irritated, causing pain. This is called patellofemoral pain syndrome (PFPS), sometimes also referred to as PFJ syndrome, patella maltracking or runner's knee. Pain is usually felt on the inside of the kneecap when running, squatting, jumping, bending, using stairs or hopping. Sitting for long periods of time or keeping your knees bent can also result in pain. What Causes It?
The patella sits in a shallow groove at the front of the knee and usually moves up and down as the knee bends and straightens without too much trouble. The quadriceps muscles located at the front of the thigh contract and pull on the kneecap, which then attaches to the shin bone and acts to straighten the knee. If one side of the quadriceps is stronger or tighter than the other, it can cause the kneecap to pull more to one side and over time become irritated. The cause of muscle imbalance or weakness can be varied. In general, the outer muscles of the thigh tend to be stronger and tighter than the inner muscles. If you have poor posture and hip position, this can cause the outer muscles to work harder and the inside muscles to become weaker. Lack of arch support in your feet or a physical anomaly of the knees can also contribute to this condition. How Can Physiotherapy Help? Diagnosing patellofemoral pain syndrome correctly is important because pain on the inside of the knee can also be caused by other injuries, dislocations, inflammation, arthritis and a variety of other less common conditions. With that in mind, it is helpful to know that your physiotherapist can diagnosis PFPS accurately and identify its likely causes. Whether it is due to poor posture, a lack of arch support in your feet, or poor running technique, your physiotherapist will assess the problem and provide a specific treatment program to best approach your condition. PFPS usually responds well to biomechanical analysis and correction of any muscular weakness and imbalance. Having the correct shoes and orthotics can also make a huge difference. There are some short-term treatments, such as patella taping, dry needling, massage, trigger point therapy and ultrasound, which may help alleviate symptoms quickly and keep you active while you address the other factors contributing to your pain. In the rare case that your condition is not helped by physiotherapy, surgery may be considered as a last resort. For more information, please ask your physiotherapist. Tendons, the connective tissues that join muscles to bone are known for being notoriously difficult to treat once injured. The reason for this is that often they are injured through stress or overuse, and compared to muscles they can have relatively poor blood flow, which is essential for healing. Tendons and muscles work together to move your joints and together are called a contractile unit. As muscles are exercised and gain strength, the attaching tendons are also placed under tension and adapt to this to become stronger. If the load placed on the tissues exceeds their capacity, the tendon fibres can begin to break down and become stiff and painful. Is my pain related to a tendon injury?
For an accurate diagnosis, you will need to be assessed by a physiotherapist. However, some signs that your pain might be coming from an in issue with a tendon are; · The pain is quite specific and can be felt over the tendon itself; · The pain is worse when under stress and improves when rested; · The pain improves after exercise has started, but it might be worse once you cool down; · The area around the tendon may feel stiff after periods of rest, particularly in the morning. How are tendon injuries treated? When it comes to recovery, tendons are often treated differently to other injuries. While each tendon injury is unique and will require assessment and intervention by a physiotherapist, there are a few general approaches that usually help with all tendon injuries. Reducing your activity to a comfortable level is the first step to recovery. Complete rest can actually delay healing as the tendon simply becomes weaker and less able to cope with subsequent loads. Your physiotherapist can provide you with a targeted exercise program to aid your recovery. Eccentric exercises, which are exercises that work alongside gravity, have been shown to stimulate tendon healing and strength. Stretching may aggravate your injury and should be used with caution. Assessment of any biomechanical faults or stresses that are placing undue load on the tendon is also a central component of treatment. Your physiotherapist is able to guide you with your recovery and return to sport to avoid aggravating any injury. Running is a great way to stay in shape, manage stress, and increase your overall wellbeing. However, it's not without its drawbacks. While being a low-risk activity, there are a few injuries that commonly affect runners. As running is a repetitive impact activity, most running injuries develop slowly and can be challenging to get on top of. Here are three of the most common conditions faced by runners, all of which can be helped by your physiotherapist. 1. Runner's Knee:
Runner's knee (patellofemoral pain syndrome) is a persistent pain at the front or inside of the knee caused by the dysfunctional movement of the kneecap during movement. The kneecap sits in a small groove at the centre of the knee and glides smoothly up and down as the knee bends and straightens. If something causes the kneecap to move abnormally, such as muscle imbalance or poor footwear, the surface underneath can become damaged, irritated, and painful. The pain might be mild to start with, but left untreated, runner's knee can make running too painful to continue. 2. Shin Splints: Shin splints (also known as medial tibial stress syndrome) is a common condition characterised by a recurring pain on the inside of the shin. While the cause of this condition is not always clear, it is usually due to repeated stress where the calf muscles attach to the tibia (shin bone). Why this becomes painful is likely due to a combination of factors that can be identified by your physiotherapist to help you get back on track as soon as possible. 3. Achilles Tendonitis/Tendinopathy: The Achilles tendon is the thick tendon at the back of the ankle that attaches the calf muscles to the heel bone. The amount of force that this tendon can absorb is impressive. It is vital in providing the forward propulsive force needed for running. If the stresses placed on the tendon exceed its strength, the tissues begin to breakdown and become painful. Treatment is focused on helping the healthy tendon tissues to strengthen and adapt to new forces while allowing the damaged tissue to heal and regenerate. What is an ACL tear and how does it occur? The ACL, or anterior cruciate ligament, is a strong piece of connective tissue which helps attach the thigh bone (femur) to your shin bone (tibia). The ACL provides stability to the knee joint as it prevents the tibia from sliding forward relative to the femur. ACL tears are a common sporting injury, however they can also occur from everyday activities. The most typical mechanisms of injury are landing awkwardly from a jump, twisting the knee, or suddenly stopping while running. The ACL may also be injured during knee hyperextension, or getting hit on the outside of the knee. Often, other tissues surrounding the knee are also damaged, including the medial collateral ligament, meniscus, joint cartilage and bone surfaces. The ligament can be stretched, partially damaged or completely torn. What are the signs and symptoms?
Many people report hearing a “pop” in the knee along with immediate pain and swelling. Decreased range of movement of the knee is common and the injured knee is typically unable to take full weight when standing or walking. The knee may also feel unstable, with a sensation of “giving way”. Poor balance and coordination may also be experienced. Smaller tears of the ligament may have only mild symptoms, however, more severe tears will have more significant pain, swelling and instability. Is surgery necessary? Traditionally, surgery was thought to be necessary for all full-thickness ACL tears. A series of recent studies have shown however, that outcomes are often the same for people who chose surgery and those who didn’t, both in terms of recovery and future risk of osteoarthritis. Individual circumstances will impact this decision. Elite athletes and cases with additional meniscal tears may do better with surgery. Generally speaking however, with time and full rehabilitation, many people can return to their previous levels of activity without surgery. How can physiotherapy help? For both surgical and non-surgical recovery from ACL tears, physiotherapy rehabilitation is essential for a full recovery. Your physiotherapist will assist you with improving your knee range of movement, lower limb strength, balance, stability and coordination. You will re-learn the tasks of walking, using stairs, and negotiating obstacles with retraining of your balance and control. Early in rehabilitation, the RICE protocol (rest, ice, compression, elevation) is used in conjunction with static resistance type exercises to improve muscle contraction in the leg and increase blood flow to the area. Throughout your rehabilitation program, you will progress through a variety of strength and mobility exercises targeted towards your individual needs, with goals of returning to your favourite sport or hobby as soon and as safely as possible. |
Categories
All
|