|
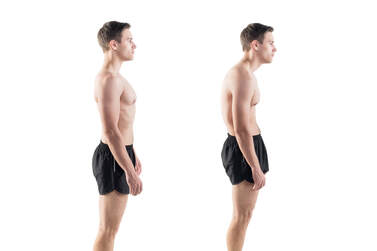
Low back pain is one of the most common conditions treated by physiotherapists and if you are unlucky enough to have been a sufferer, you know that severe back pain can take over your life. With improved understanding, health professionals have come to identify some common myths about back pain that are inaccurate, misleading or even counterproductive... Myth #1 – Discs can ‘slip’ out of place
Sitting between the vertebrae of the spine are soft discs that provide flexibility and shock absorption to the spine. In the past, many health professionals have told patients that these discs had ‘slipped’ as a way of explaining their pain to them. This is not entirely accurate, as these discs are actually very secure and rarely, if ever 'slip' out of place. Discs may bulge slightly or in some cases tear, however more often than not these injuries will heal without any permanent damage and exist in many people without causing any pain at all. Incorrectly thinking that a part of your spine has permanently ‘slipped’ out of place can cause you to move differently, which can create more pain and dysfunction in itself. Myth #2 – If you have low back pain, you should stay in bed When back pain strikes, our natural instinct is to rest, avoid movement and wait for the pain to pass. However, studies have shown that being active and performing targeted and gentle exercises can help improve low back pain. In fact, our impulse to stop moving and protect our spines can actually cause abnormal movement patterns and stress, leading to ongoing pain after the original injury has healed. If you are unsure of what kind of exercises you should be doing, your physiotherapist can help guide you with a targeted exercise program. Myth #3 – Severe pain means severe damage Pain that is severe, strikes suddenly and without warning can be a very scary experience. If this happens to you, you could be forgiven for assuming you must have sustained a very serious injury. The fact is, however, that the spine, being surrounded by nerves, is a particularly sensitive area of the body and pain in this area can be very strong without significant damage. A small ligament sprain or a muscle spasm can actually cause a large amount of pain, but it is common for intense symptoms to settle down quickly, even disappearing within a few days. In many cases, symptoms that last for longer than 2-3 weeks are caused by changes to your movement patterns in response to this pain and not the original injury itself. If you are suffering from back pain, the best person to see is your physiotherapist. They can help you to recover without any complications or side effects and help you safely return to your usual activities while also ruling out any serious damage that might need further investigation.
0 Comments
Almost everyone will experience lower back and/or neck pain at some point in their lives, even if just in the form of a slight neck twinge after sleeping in an odd position. Spinal pain of the thoracic region (the upper & middle part of your back) is less common, however you might be surprised to discover how important this part of the body can be when it comes to pain and injury. What is it?
The thoracic region refers to the part of the spine that is surrounded by the rib cage. It consists of 12 vertebrae with discs that sit between each of them. The thoracic spine isn’t an area that you might associate much with movement, however, this area can account for a surprising amount of flexibility, particularly in rotation. With joint attachments both between each side of the 12 vertebrae and a rib on either side, the thoracic spine has almost more individual joints than you can count. If each of these joints is not regularly moved through their full range they can tighten up and lose flexibility. This stiffness can become quite significant over time. Why is it important? Many people may not even notice this lack of movement, primarily because the neck and lower back provide much more range and can usually compensate for any loss of thoracic flexibility to complete everyday tasks. When there is no movement occurring in the thoracic region, this means that the structures of the joints in other regions are pushed closer to their limits of range, particularly during rotation. This results in more compression and stress on these joints and the structures surrounding them, such as nerves, blood vessels and muscles. Thoracic stiffness can be a significant risk factor for neck and lower back pain. This can also reduce the mobility of the chest wall, which can result in less efficient breathing mechanics and, in extreme cases, even reduced exercise tolerance. Thoracic spine movement is aslo important for normal shoulder function, as well as maintaining good posture. How can physiotherapy help? Your physiotherapist is able to assess your thoracic mobility and help you with treatments to improve your range, both with manual therapy and home exercises. They may even help improve your thoracic flexibility as part of a treatment plan for neck and lower back pain. If you've been unlucky enough to suffer from chronic or persistent back pain, chances are that at some stage you've had scans to capture what is happening inside your spine. Magnetic resonance imaging (MRI) is an incredible technology that can provide valuable insights into tissues that otherwise can't be seen. Unfortunately, there are some common misconceptions around what that information means, which can sometimes be unhelpful and even harmful to recovery. Here are a few things you might not realise that can help you understand your MRI... Not all tissues show up on every scan.
Muscle, fascia, or other irritable tissues may not show up on your scan, meaning you may experience a lot of pain but have a completely normal scan. Not all parts of your anatomy will show up from every scan's perspective and some tissue changes might only be evident in certain postures. Age-related changes are normal and may not be related to your pain. Results such as arthritis, disc bulges, and small tears can be concerning. However, it's helpful to note that people who have no painful symptoms can have similar, if not more, age-related changes and these signs may not be related to your pain at all. Severe pain may not be related to severe changes on MRI. Pain is a complex experience, influenced by multiple factors including the sensitivity of the tissues involved, what the brain believes about the pain and what it means, and how long it has been present. MRI is helpful for ruling out severe pathology such as infection, fracture, or malignancy, but it is not always an accurate guide to the source of symptoms. The results of an MRI should always be taken into account as a small part of a bigger clinical picture when guiding treatment. Talk to your physiotherapist for advice on any imaging results you have and what they might mean for your treatment and prognosis. None of the information in this article is a replacement for professional medical advice. Always consult a medical professional for advice on your condition. Travel can be one of the most enjoyable aspects of life. However if a trip away comes with the risk of increased pain and soreness, the excitement can be thoroughly diminished. Some people may avoid travel altogether if their symptoms are exacerbated too much by long periods of sitting in a car or aeroplane. If you are unlucky enough to fall into this category, here are a few tips from your physiotherapist that might help make long trips a little more comfortable, particularly if you tend to suffer from lower back pain... 1. Adjust the seat angle.
If you are able, tilt the seat slightly down towards your feet, not towards your hips. Ideally, your knees should be level with your hips, or even slightly lower. A footrest to lift your knees can also help. 2. Lift the height of the whole seat. This will assist with tip number 1 by lifting the whole body away from the floor. When your hips are less flexed, it is easier for your back to sit comfortably in an upright position. 3. Use a lower back support. Many cars nowadays come equipped with in-built lumbar supports. Often this support is a generic design and not fitted for your specific shape or height. A proper lumbar pillow, or even a rolled towel in the small of the back, can be more effective in maintaining the natural arch of your spine. This eases pressure on your intervertebral discs, spinal ligaments and muscles. Neck discomfort is easier to improve when tips for lower back are implemented first. Some other simple tips to reduce neck pain are as follows... 1. Use a travel pillow. If travelling on an aeroplane, try wearing the pillow backwards or sideways. This assists in supporting the head in a slightly better position when you rest or sleep, which helps to reduce the stress placed on the muscles, ligaments and joints of the neck. 2. Every hour, perform 10 chin tucks. This is easiest to perform correctly if you sit tall and press your chin straight backwards, lengthening the back of your neck. Do not tuck the chin to the chest. This exercise stretches the small postural muscles at the base of the skull, helping to relax them. If you find these tips helpful, continue performing them throughout your travels and enjoy your time away! For most of us, screen time and sitting go hand in hand and both are only increasing as our lives move more online. While short periods in any posture aren't harmful, a lack of movement combined with long periods spent in hunched positions can lead to spinal pain, headaches, shoulder pain and more. If you're needing to spend more time in front of a screen, here are a few tips that can help you to keep flexible and avoid pain. Set movement breaks
Posture in itself isn't always a problem. Spending long periods of time in these postures without taking breaks is the problem. When your body is so used to one position, muscles may become shorter and joints stiffer, making it harder to move out of this posture without pain and discomfort. You can break up your day by setting a timer to move and take a break every 20-30 minutes. Using these short breaks for movement is a great way to both help focus at work and keep your body more flexible. Setup your work and home environment properly Adjusting your work station or setting up a place to relax at home where to you can avoid a hunched posture can help you to reduce time in the same posture. Your physiotherapist can give you tips for how to setup your home and office environment correctly. Take stock of your time spent sitting Time in the car, time on your computer and time on the couch can all quickly add up without you realising. By accounting for the amount of time you spend sitting, you can find more ways to move. For example, if you notice that you're sitting down as soon as you get home, try swapping out watching an episode on TV to going for a walk while listening to a podcast. Ask your physio for specific stretches If you can identify the posture you spend the most time in, your physio can help you to develop a specific exercise and stretching program to counteract these positions most directly and keep you strong and flexible. For most of us, the hours we spend sleeping are simply a time for rest and recovery. However, you might be surprised to learn that your sleeping position can have a significant impact on your body, particularly if you already have an injury. Here are some tips to help to stay pain free overnight. Back pain tips:
For sufferers of back pain, finding a comfortable position at night can be difficult. The natural curves of the spine need to be maintained and supported throughout the night. Ideally, your body should be held in a position of minimal stress while sleeping. This means that all your joints and muscles are resting in a neutral position A mattress that is too soft might feel comfortable to begin with, but over time will let you sink into it too much, meaning the curve of the lower spine will be lost. Waking up with a stiff or sore back could be a sign that you are using the wrong mattress. A mattress that is too firm can also mean your spine is held in a flattened position, which is both uncomfortable during the night and when you wake up. For many people, sleeping on their side keeps their spine in a more natural alignment than sleeping on their back, especially if they put a pillow between your knees. If you do sleep on your back, placing a pillow under your knees can help to maintain your lumbar spinal curve throughout the night. This can also help to reduce hip and knee pain. Neck pain tips: The neck is often the most vulnerable part of the body if your sleeping setup is not ideal. Side sleepers may let their neck fall excessively to the side with a pillow that is too low or have their neck elevated too much by having their pillows too high. If you find yourself putting your arm under your pillow while you sleep, it is likely that your pillow is too low. Having your shoulder in this position overnight can put unnecessary stress on the structures around the shoulder joint and should be avoided if possible. Stomach sleeping can also put additional pressure on your neck as it is turned to the side for long periods. Hip pain tip: Side sleepers often spend their nights with one leg crossed over their body. This can place extra pressure on the structures on the side of the hip, such as tendons and bursa and can impact the health of these tissues as the compression reduces the blood flow to the area. Placing a pillow under your knee while sleeping on your side in this position can help to maintain a neutral alignment of your hip. Speak to your physiotherapist for more advice on how to improve your sleeping posture and find out if your sleeping setup is right for you. What is Ankylosing Spondylitis? Ankylosing Spondylitis (AS) is a type of inflammatory, autoimmune arthritis that primarily affects the spine. It is characterised by intermittent pain and progressive stiffness due to the inflammation and eventual hardening of the ligaments that surround the spine. The classic early symptoms of AS are pain and stiffness of the sacroiliac joints, the joints connecting the pelvic bones to the sacrum in the lower back. In the more severe, final stages of the disease, the entire spine can become fused and rigid, often in a flexed, forward posture. As this is an inflammatory disorder, many other systems and joints can also affected. A significant number of people with AS also suffer from irritable bowel syndrome and inflammation of the eye. What causes it?
The cause of Ankylosing Spondylitis is not clear, however there are markers and predisposing factors that may contribute to the development of the condition. Genetics, chronic stress and frequent gastrointestinal infections are among the predisposing factors. Men are affected more often than women and symptoms usually begin between the ages of 17 and 45 years. What are the signs and symptoms? Intermittent back pain and progressive stiffness are the two most common symptoms of Ankylosing Spondylitis. Other tendons and ligaments may be affected, including those in the hands, feet and ribs. Symptoms tend to be worse following periods of rest, particularly first thing in the morning and improve following periods of activity. It is common for people to experience “flare-ups” and “remissions” of symptoms. Some people with AS may experience mild discomfort in the spine from time to time, while others may experience severe and debilitating symptoms at frequent intervals with minimal time in remission. Long term issues with AS include breathing difficulties due to thoracic and rib cage stiffness and severe spinal pain and immobility. Medical treatment focuses on reducing inflammation and slowing the disease process. How can physiotherapy help? Physiotherapy treatment aims to manage pain during flare-ups and maintain optimal posture as the disease progresses. Your physiotherapist will assess your spinal movement and posture as well as strength. If your hands, feet, hips or shoulders are affected, they will also provide you with specific exercises to help maintain mobility and strength in those joints. Many studies have proven the positive benefits of exercise for those with Ankylosing Spondylitis, such as improved rib cage expansion when breathing, and improved posture of the upper back and neck. Why are workplace injuries so common? The nature of work is that we are often required to complete the same task for hours. We can also find ourselves faced with time constraints and deadlines that lead to poor postures and taking shortcuts, simply to get the job done. How can they be prevented?
Workplace injuries can happen suddenly, through an accident like a fall or by lifting something too heavy. However, just as many workplace injuries occur over time due to repetitive tasks. Often these conditions begin slowly and take many months to resolve. Here are a few tips to keep yourself pain free in the workplace. Moving Items: It's important to assess any risk before you start. Do you need to ask for help or use an assistive device? Your legs are the strongest part of your body, so ideally you should use them to power your movement, rather than your arms or back. Bending and twisting when lifting is also a common mechanism for injury. It is much safer to lift, then step to turn before putting an object down again rather than twisting on the spot. Also, pushing is a more efficient movement than pulling and is always preferable if you have a choice. Try to push at waist height and keep resistance as close to your body as possible. Office Work: Overuse injuries can occur by always using the same side of your body rather than alternating sides. Practise using both left and right hands for taking phone calls and using your mouse. Be aware of your posture. Good posture isn’t just about having a rigid and upright spine, it’s about being able to let your spine sit comfortably in its natural curves and be able to move in and out of this easily. Stretching can help to counteract positions you find yourself in for long periods, and remember, there's no substitute for regular movement. Set an alarm on your computer or phone every 30 to 45 minutes to stand up and move. A physiotherapist is a great person to speak to about preventing injuries in your workplace, be it about heavy manual work or repetitive, sedentary office work. Back pain is such a common experience that it is estimated up to 80% of adults will have at least one severe episode of lower back pain in their lifetime. For many people, the pain quickly resolves and things go back to normal. However the first time this happens to you it can be scary, particularly as severe pain can occur suddenly and without warning. Statistics however are on your side. Most of the time, acute low back pain resolves without consequence and doesn’t recur. If you happen to be in the middle of an episode though, here are a few tips to help you get through.
While this may seem obvious, there are a few people who will always try to push through the pain. The expression "no pain, no gain" is in many cases outdated and if your work requires heavy lifting, it is more than reasonable to take a few days off. 2. Avoid too much rest. On the other hand, lying in bed all day is bad for you as well. If you have severe back pain, gentle movement under the advice of a physiotherapist is much better for you than complete rest. 3. Avoid long car or plane trips If possible, now is the time to avoid long distance travel. If you absolutely must travel, speak to your physiotherapist about how to manage your pain during the trip. 4. Avoid listening to horror stories There are always stories about pain that never went away, requiring surgery, which only made it worse. While worst case scenarios can happen, they are rare, and being fearful can negatively impact your recovery. That terrible story is probably not going to happen to you and hearing these stories is only going to worry you and make you feel worse! 5. Avoid delaying treatment While your pain may go away on its own, it is important to have a professional assess your condition to screen for any serious injuries and advise you on how to best manage your pain while you are getting better. They can also help you recover as quickly as possible, as well as give you advice on how to avoid future episodes. 6. Don’t expect a miracle cure Back pain is complicated and a single treatment that works for everyone simply does not exist. It is important to follow the directions of your therapist and work with them to set reasonable and realistic goals for your recovery. None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual injury. What Are They? Trigger points are what are often thought of as muscle "knots" and can feel like painful, hard lumps located in your muscles. These points can both be painful to touch and refer pain to surrounding areas. It is thought that trigger points form when a portion of muscle contracts abnormally, compressing the blood supply to this area, which in turn causes this part of the muscle to become extra sensitive. Trigger points are a common source of pain around the neck, shoulders, hips and lower back. What Causes Trigger Points?
Many factors can cause trigger points to develop. Repetitive stress, injuries, overuse and excessive loads are common examples. Inflammation, stress, nutritional deficiencies and prolonged unhealthy postures may also contribute to the formation of these painful areas. Generally speaking, muscular overload, where the demands placed on the muscle mean that the fibres are unable to function optimally, is thought to be the primary cause of trigger points. This is why you might notice trigger points in weaker muscles or after starting a new training program. Signs and Symptoms Pain caused by trigger points can often be mistaken for joint or nerve-related pain as it can be felt in a different location to the site of the trigger point. Trigger points feel like hard lumps in the muscles and may cause tightness, heaviness, aching pain and general discomfort. They can cause the length of the affected tissues to shorten, which may be why trigger points can increase the symptoms of arthritis, tennis elbow, tendonitis and bursitis. How Can Physiotherapy Help? Your physiotherapist will first assess and diagnose whether trigger points are contributing to your pain. If they feel that treatment will be beneficial, there are a variety of techniques that can help, including dry needling, manual therapy, electrical stimulation, mechanical vibration, stretching and strengthening exercises. While these techniques may be effective in treating trigger points, it is important to address any biomechanical faults that contribute to their development so they don't keep recurring. Your physiotherapist is able to identify causative factors such as poor training technique, posture and biomechanics and will prescribe an exercise program to address any muscle weaknesses and imbalances. If you have any questions about how trigger points might be affecting you, don’t hesitate to ask your physiotherapist. |
Categories
All
|