|
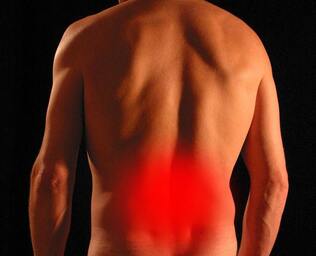
Have you ever woken up with a stiff and painful neck that will only turn to one side? You might have been suffering from acute wry neck, a painful condition following a typical pattern of symptoms. Most wry necks are classified as one of two different types – facet (joint) or discogenic wry neck. Facetogenic Wry Neck:
Facet joints are found on either side of the spine and allow controlled rotation and side bending of the neck. An awkward or sudden movement of the neck can cause a part of the joint capsule to strain, tear or get caught in the joint, making it feel locked. The muscles around the area can also become tight and spasm, which amplifies the pain. The pain is usually sharp and can be pinpointed quite accurately to the part of the neck causing the problem, and the pain rarely travels down into the arm. It is usually possible to find a resting position where the pain goes away completely, only having pain when turning in specific directions. The good news about facetogenic wry neck is that your physiotherapist is usually able to help you ‘unlock’ the neck quite quickly with gentle mobilisations. Most of the time, a full recovery can be expected within a week. Discogenic Wry Neck: The vertebrae of the neck are separated from each other by fibrous discs, filled with a gelatinous centre. These discs provide support, flexibility and shock absorption. When placed under pressure, these discs may bulge or tear, and the resulting swelling can cause pain and muscle spasm in the surrounding area. It is important to note that in an area as sensitive as the neck, a small amount of damage can result in a large amount of pain. The development of discogenic wry neck is usually due to a combination of factors, including neck stiffness, poor posture and biomechanics than can contribute to the disc being vulnerable prior to the injury. In these cases, it can be challenging to find a comfortable position, and it is more likely for pain or tingling to travel into the arm. Treatment of discogenic wry neck is focused on reducing pain and muscle spasm with massage, taping, heat and postural education. Further treatment aims to reduce any stress that is being placed on the disc, mobilise any stiff spinal segments and correct any muscle imbalances. While the initial symptoms may settle down quite quickly, it can take up to six weeks to fully recover from discogenic wry neck. In this condition, it is also essential to address all the factors that may cause a recurrence of the issue.
0 Comments
What Are They? Trigger points are what are often thought of as muscle "knots" and can feel like painful, hard lumps located in your muscles. These points can both be painful to touch and refer pain to surrounding areas. It is thought that trigger points form when a portion of muscle contracts abnormally, compressing the blood supply to this area, which in turn causes this part of the muscle to become extra sensitive. Trigger points are a common source of pain around the neck, shoulders, hips and lower back. What Causes Trigger Points?
Many factors can cause trigger points to develop. Repetitive stress, injuries, overuse and excessive loads are common examples. Inflammation, stress, nutritional deficiencies and prolonged unhealthy postures may also contribute to the formation of these painful areas. Generally speaking, muscular overload, where the demands placed on the muscle mean that the fibres are unable to function optimally, is thought to be the primary cause of trigger points. This is why you might notice trigger points in weaker muscles or after starting a new training program. Signs and Symptoms Pain caused by trigger points can often be mistaken for joint or nerve-related pain as it can be felt in a different location to the site of the trigger point. Trigger points feel like hard lumps in the muscles and may cause tightness, heaviness, aching pain and general discomfort. They can cause the length of the affected tissues to shorten, which may be why trigger points can increase the symptoms of arthritis, tennis elbow, tendonitis and bursitis. How Can Physiotherapy Help? Your physiotherapist will first assess and diagnose whether trigger points are contributing to your pain. If they feel that treatment will be beneficial, there are a variety of techniques that can help, including dry needling, manual therapy, electrical stimulation, mechanical vibration, stretching and strengthening exercises. While these techniques may be effective in treating trigger points, it is important to address any biomechanical faults that contribute to their development so they don't keep recurring. Your physiotherapist is able to identify causative factors such as poor training technique, posture and biomechanics and will prescribe an exercise program to address any muscle weaknesses and imbalances. If you have any questions about how trigger points might be affecting you, don’t hesitate to ask your physiotherapist. Referred pain is one of the most complicated processes in the human body. You may have experienced this if you ever saw a physiotherapist for pain in one part of your body, and they started to treat an entirely different area. The complexity of pain is one of the reason's why physiotherapists conduct such a thorough interview with you and physical examination before being able to determine the exact source of your pain. Why is pain so complicated?
Unfortunately, we still don't understand everything about the way pain is processed. Usually, when an injury or damage occurs to body tissues, a signal is sent to the brain, which begins to interpret this signal and creates the sensation of pain. Pain is thought to be a warning signal to let you know to avoid danger and pay attention to the injured body part. Occasionally this system goes a little haywire, and pain signals are sent when there is no damage or the location of the pain is misdirected. Referred pain is the term used when pain is felt at a different location to the source of the problem that is sending the pain signal. There are many kinds of referred pain, and some are easier to explain than others. What are the different types of referred pain? In some cases, if it is a nerve that is sending the pain signal, then pain can be felt all along the length of the nerve. This may be described as a sharp burning pain along the skin. One of the most common examples of this is "sciatica", where the large nerve that runs down the back of the leg is irritated around the lower back or buttock. The source of the pain signal is near the spine. However, that pain follows a distinctive pattern down the leg. In other cases, it is the muscles and not the nerves that are referring pain elsewhere. Muscular trigger points are taut bands that develop within muscle tissue that is undergoing abnormal stress. Poor posture, lack of movement, and overuse can cause muscles to develop areas of dysfunction. These trigger points can cause pain that radiates out in distinctive patterns. Trigger points are diagnosed as the source of pain if symptoms are reproduced when a therapist presses on a specific point. If that wasn't confusing enough, we know that our internal organs can also refer pain. Pain referred by internal organs may be described as a deep ache, and usually not influenced by movements of the limbs or back. Organs often distribute pain in patterns that are very obscure and sometimes don't even create any pain at their own location. For example, kidney pain can feel like lower back pain. There are many other fascinating aspects to pain and understanding how it works is an important part of managing your symptoms. To understand how referred pain may be affecting you, talk to your physiotherapist who can help with any questions. None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your individual injury. If you are experiencing regular neck pain that just won’t go away, it’s possible that parts of your daily routine are contributing without you realizing. Here are a few common everyday activities that might be making your neck pain worse... 1. Your sleeping position
It’s easy to underestimate the impact your sleeping position can have on you. However, spending hours in one position will undoubtedly have an effect on your body. Pillows that are too high or too flat can mean your cervical (neck) joints are sitting at the end of their range in too much flexion or extension. Similarly, sleeping on your stomach often means your thoracic (upper/mid back) spine is locked into extension and your neck is fully rotated. In simpler terms, this means your joints are under more stress than necessary. Ideal sleeping posture allows your spine to maintain its natural curves. 2. Your daily commute Many of us make sure our work stations are ergonomically set up to reduce stress and strain throughout the day. Few of us take the same consideration when it comes to driving. In fact, the set up of your car can be just as important as your work desk, particularly if you are driving more than 30 minutes every day. The correct setup in your car can mean you use less effort to drive and turn your head less often to check traffic. Ensuring that your steering wheel, seat and mirrors are set up correctly could make a difference to your posture and perhaps reduce neck pain and headaches. If you find that driving is still affecting your pain after making these changes, try catching public transport or riding a bike on alternative days if that's possible for you. 3. Your downtime Many of us unwind by watching TV or our laptops at the end of the day. Your position during this time can be something you don't really consider. However, looking up to view a screen mounted on a wall or looking down at a small screen or laptop can put pressure on the structures of the neck. Take a few minutes to consider what posture you’re sitting in before settling down to binge watch a series and see if you can either lower the height of your screen or raise it slightly so your neck can be in a more neutral position. 4. Your exercise routine Any activity that requires sustained positions or repetitive neck movements can contribute to neck pain. Cyclists can be stuck in neck extension while looking ahead and breast stroke swimmers can also have excess neck extension. Freestyle swimmers with reduced thoracic or neck rotation can have difficulty achieving rotation when breathing which can cause pain and discomfort over time. Your physiotherapist is able to identify any daily habits or activities that might be contributing to your neck pain. Come and see us for an appointment to see how we can help. |
Categories
All
|
|
The Physio Nook
197A Scarborough Beach Road Doubleview WA 6018 08 9446 7017 doubleview@thephysionook.com.au |