|
We know that office life can wreak havoc on our body. Even with the best intentions, finding time to reverse the pressures of 8 hours a day sitting in a chair can be difficult. Here are three easy stretches to do daily that focus on common problem areas for office workers. Chest & shoulders stretch (wall angels):
Find a large flat wall and stand facing away from it. You may need to bend your knees slightly or step a few inches forward. Your pelvis, upper back and back of your head should all be in contact with the wall, with small gaps where the curves of your spine are. If you are unable to keep your head to the wall, you may need to use a towel behind your head to make this position comfortable. Tuck your chin in gently, keep your palms facing forward, elbows bent to ninety degrees with the backs of your arms against the wall. Now slide your arms up along the wall, as high as you can while keeping them in contact with the wall, pause for a few seconds and slide them down again. Repeat 5 to 10 times. This will stretch your chest and shoulder muscles which get tight from slouching at a desk, as well as help you to develop a sense of head position alignment with your body. Hip flexor stretch (lunge): Kneel on one knee, place your other foot on the floor in front of you and keep your knee bent to 90 degrees. Keeping your hips even, shift your pelvis forward but keep your shoulders back until you feel a stretch at the front of your hip of the kneeling leg. Hold for 30 to 45 seconds and then swap legs. Repeat 2 to 3 times. This will stretch your hip flexor muscles which are often tight from sitting for long periods. Seated hamstring stretch: Sit on the floor with one leg straight out in front of you. Bend your other leg and tuck your foot in towards your inner thigh. Reach forward with both hands and stretch towards your foot on the straightened leg, bending at your hips as much as possible. You should feel a stretch at the back of your thigh, if you feel a pull behind your knee you can point your toes or bend your knee slightly. Hold for 30 seconds and slowly come back up, change legs and repeat 2 to 3 times on each leg. Check with your physiotherapist if there are other stretches that may benefit you.
1 Comment
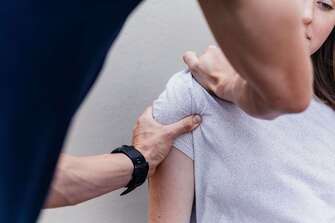
Many people already know the value that physiotherapy brings to their life, they may have had a physiotherapist with them through the highs and lows of injury and recovery more than once! However, for those who have never been to see a physiotherapist before, there can be a question mark over exactly what it is that physiotherapists do. What is it that physiotherapists do?
The answer is tricky because physiotherapists do so much. We might be described as pain management experts, as we work to reduce the pain of our clients, from those who have suffered a new injury to those who have had pain for several years. We first identify the cause of the pain and then provide manual therapy techniques, education, exercise and self-management strategies to help our patients understand, manage and reduce their symptoms. The pain or injury that motivates people to come and see us has often made them give up activities or sports that they love and can even be getting in the way of everyday tasks. By identifying the cause of your symptoms, we can help to get you back to full function. Physiotherapists are able to do this for people at all activity levels, including the general public, elite athletes and those dealing with serious disabilities. In fact, physiotherapists have a role to play at practically every stage of life. We can assess infants to monitor their motor skills development and as they grow we help them deal with the pains and vulnerabilities of a growing body. Among other things, we can help to prevent injuries, improve pelvic floor dysfunction and work to prevent falls in the elderly. Not just exercises and massage. Physiotherapists offer a range of treatments, from self-management strategies, stretches, manual therapies, dry needling, exercises and massage, to name a few. A huge part of recovering from pain and injury comes from understanding what is happening to you and how to best manage your issues. Rather than create a dependency on your therapist, we aim to empower our patients to improve their health independently as much as possible as well. A physiotherapist's primary goal is to improve your quality of life and remove any barriers to full function and participation in whatever you desire, whether these barriers are due to pain, weakness or stiffness. Can prolonged stress affect your pain and healing? Research now suggests that it can, particularly with chronic pain. If you suffer from ongoing pain you may have noticed this relationship yourself. Many people know that their pain is worse when they are stressed but they don't know why. Stress activates your sympathetic nervous system, this is the where we can move into "fight, flight or freeze" mode. The sympathetic nervous system is responsible for keeping us safe when we are in danger, however it can be activated for prolonged periods and many of us lack the skills to return control to our parasympathetic nervous system, which is responsible for helping us to "rest and digest".
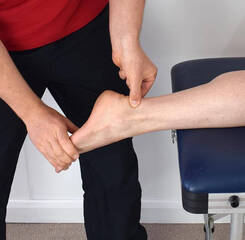
How would this affect pain? During this state muscles become tense and ready for action, the nervous system is extra sensitive to stimulus, blood pressure is raised and we are more likely to notice and have negative thoughts. Tense muscles can become tired and sore or put extra stress on other structures, causing pain and irritation. Often when in a stressed state our breathing becomes shallow and rapid, even when not really exerting ourselves, such as while sitting in an office. Use your breathing to recover. An effective way to help your body return control to the parasympathetic nervous system is to consciously change your breathing. One method is to hold your breath for as long as you can, once you relieve your breath your body senses that a threat has passed and can return to a more relaxed state. Another commonly used technique is box breathing. To do this, breathe in for four seconds, hold for four, breathe out for four, hold again for four and repeat. Do this for a few minutes until you start to feel more relaxed and calm. Show your body that you are safe. Other activities that can help your body to relax include yoga, going for a swim or having a shower, or doing some intense exercise where your heart rate is raised. Speak to your physiotherapist for more information on this topic and tips to help you relax during the day. Essentially, the ankle consists of three bones, the tibia, fibula and talus, all held together by thick fibrous ligaments. The bottom parts of the tibia and fibula (shin bones) join together and surround the talus in such a way that it is able to rock forwards and back while providing stability and restricting the side-to-side movements. The ligaments holding the tibia and fibula together are large and thick, forming a syndesmosis. An injury to this area is known as a high ankle sprain. How do they happen?
A high ankle sprain can occur when your lower leg twists inwards while your foot is planted on the ground. The foot is typically pushed back and rotated outwards, putting excess pressure on the ligaments that hold the lower leg bones (tibia and fibula) together. This force can cause the syndesmosis to tear resulting in a gapping of the two bones, which can lead to significant instability of the ankle. This can happen simply from a fall, but more commonly while playing sports that involve running and jumping. This is also a common injury for downhill skiers. You are often unable to walk on your toes after this type of injury. What is the difference between a high and a low ankle sprain? A "normal" or low ankle sprain is a tear of the ligaments connecting the ankle to the foot, a syndesmosis tear (between the bottom of the tibia and fibula) is called a “high” ankle sprain. High ankle sprains are much less common than lower ankle sprains, accounting for only 1-11% of all ankle injuries. It can initially be difficult to tell the two injuries apart. To complicate things, a fracture of the ankle will also have similar symptoms. Your physiotherapist has a set of physical tests they can perform if they suspect a high ankle sprain. Ultimately imaging such as X-Rays or an MRI may be required to confirm the diagnosis. Why does correct diagnosis matter? High ankle sprains can take up to two times longer to heal than normal ankle sprains and require more immediate attention. Syndesmosis tears that are left untreated can result in chronic instability and pain, making them vulnerable to further injury in the future. Furthermore, if the separation of the tibia and fibula is severe enough, early surgery to fixate the injury with a screw or a "tightrope" to pull them back together may be required. What is the treatment? As mentioned, severe and unstable tears may require surgery, but most syndesmosis tears will need to be put into a supportive boot for around 4-6 weeks. Following this period a graduated rehabilitation program of strengthening, mobilization, balance, control and agility will need to be commenced before your ankle will be back to its pre-injury level of function. This can take up to 6 months in some cases. What are they? The hamstrings are a large group of muscles located at the back of the thigh. Their job is to bend the knee, extend the hip backwards and stabilise the leg. The muscles can be injured at any point along their length but are most vulnerable where the tendon and muscle fibres join together. This is a common injury for players of all sports that involve running, and particularly those that involve quick movements and kicking. What are the causes?
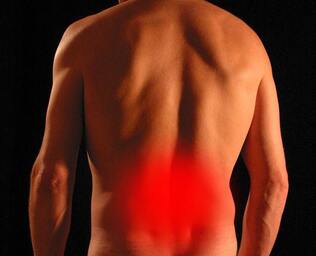
As the hamstrings cross two large joints (the hip and the knee), they need to perform complicated movements, often activating suddenly and with great force. They are often stretched during a fall, a powerful kick of a ball or a sudden take-off. Factors that increase the chance of a tear include poor flexibility, strength or neural mobility. Other factors that contribute to hamstring injuries are muscle imbalances, abnormal lower limb biomechanics, fatigue, and inadequate warm-up. The biggest predictor of a future hamstring tear though, is a previous hamstring injury. What are the symptoms? The most common symptom of a strained or torn hamstring is a sharp pain at the back of the thigh, often immediately after intense activity. There may also be swelling, bruising, difficulty walking and pain with knee movements. Your physiotherapist can confirm that the pain is due to injured hamstrings rather than any other issues, and tell you how bad the strain or tear is. Although not usually required, diagnosis can be confirmed by having an MRI or ultrasound scan. How can physiotherapy help? Once a diagnosis has been made, the first step is to follow the R.I.C.E protocol (Rest, Ice, Compression, Elevation). During the first 48 hours, you should apply ice for 20 minutes every one to two hours to reduce swelling and bruising. Consultation with your physio will include advice about your recovery, and when it is appropriate to return to sport. Your physiotherapist has many techniques that can promote healing and reduce scar tissue formation, which may include ultrasound, deep tissue therapy, electrotherapy and dry needling. Crucially, they will also prescribe you an exercise program to return strength, flexibility and control to your muscles, getting you back to your sport quickly and safely. Due to the high chance of recurrence, rehabilitation is very important and usually takes 6-12 weeks. If the muscle is completely torn, surgery may be required before rehabilitation can start. Your physiotherapist will work with you to help you set goals to get you back to your favourite activities as soon as possible. What is Ankylosing Spondylitis? Ankylosing Spondylitis (AS) is a type of inflammatory, autoimmune arthritis that primarily affects the spine. It is characterised by intermittent pain and progressive stiffness due to the inflammation and eventual hardening of the ligaments that surround the spine. The classic early symptoms of AS are pain and stiffness of the sacroiliac joints, the joints connecting the pelvic bones to the sacrum in the lower back. In the more severe, final stages of the disease, the entire spine can become fused and rigid, often in a flexed, forward posture. As this is an inflammatory disorder, many other systems and joints can also affected. A significant number of people with AS also suffer from irritable bowel syndrome and inflammation of the eye. What causes it?
The cause of Ankylosing Spondylitis is not clear, however there are markers and predisposing factors that may contribute to the development of the condition. Genetics, chronic stress and frequent gastrointestinal infections are among the predisposing factors. Men are affected more often than women and symptoms usually begin between the ages of 17 and 45 years. What are the signs and symptoms? Intermittent back pain and progressive stiffness are the two most common symptoms of Ankylosing Spondylitis. Other tendons and ligaments may be affected, including those in the hands, feet and ribs. Symptoms tend to be worse following periods of rest, particularly first thing in the morning and improve following periods of activity. It is common for people to experience “flare-ups” and “remissions” of symptoms. Some people with AS may experience mild discomfort in the spine from time to time, while others may experience severe and debilitating symptoms at frequent intervals with minimal time in remission. Long term issues with AS include breathing difficulties due to thoracic and rib cage stiffness and severe spinal pain and immobility. Medical treatment focuses on reducing inflammation and slowing the disease process. How can physiotherapy help? Physiotherapy treatment aims to manage pain during flare-ups and maintain optimal posture as the disease progresses. Your physiotherapist will assess your spinal movement and posture as well as strength. If your hands, feet, hips or shoulders are affected, they will also provide you with specific exercises to help maintain mobility and strength in those joints. Many studies have proven the positive benefits of exercise for those with Ankylosing Spondylitis, such as improved rib cage expansion when breathing, and improved posture of the upper back and neck. The benefits of keeping active may seem obvious, yet it can't hurt to be reminded of the many ways exercise can improve your life. Here are a few of our favourite reasons to get moving... 1. Exercise improves energy levels.
Improving your fitness means your body is capable of achieving more for the same energy expenditure. While doing exercise can make you tired in the short term, regular improvements to your fitness will help you get more out of your body each day, with seemingly less effort. 2. Exercise can help to reduce stress. If you are stuck in a state of stress or anxiety, exercise can help you move out of it into a calmer and more relaxed state, improving your mood, concentration and sleep. There are now many studies to support this. 3. Exercise and hobbies can help you build connections and community. Making new friends as an adult can be surprisingly difficult and the importance of connection and community is being recognised more and more as being essential for overall wellbeing. Being part of a team, group or club is a great way to build confidence and meet friends as well as keeping active. 4. Exercise keeps your muscles, tendons, joints and bones healthy. Our bodies are often compared to machinery or car parts. However, there are some crucial differences between our bodies and machines, including the fact that our bodies respond to exercise by becoming stronger and healthier, rather than being worn out. As an example, one of the best ways to prevent osteoporosis is through regular high impact activity, which stimulates bone growth. 5. Exercise can help to reduce injuries. Similar to the previous point, tissues that are used regularly are stronger, more elastic and are less likely to tear or break when under stress. Regular exercise is the best way to keep your body in a healthy state and prevent injuries. Finding the right exercise for you can be tricky, your physiotherapist can help you with suggestions based on your ability and skillset if you need some help. What is Carpal Tunnel Syndrome? The carpal tunnel is a small space where the wrist meets the base of the hand. This space is covered by a thick ligament and creates a small tunnel where various nerves, arteries and tendons pass through from the forearm into the hand. If anything causes this space to be reduced, these structures can become compressed or damaged, particularly the median nerve. This condition is referred to as Carpal Tunnel Syndrome. What are the symptoms?
The hallmark symptoms of carpal tunnel syndrome are pain, tingling or numbness in the hand, usually following a typical pattern over the thumb, index and middle finger. There can also be a reduction in grip strength and wasting of the thumb muscles. Symptoms are usually worse on waking or with repetitive hand movements. Patients might also report difficulty holding items, writing or doing up their buttons. How does it happen? Carpal tunnel syndrome can be caused by anything that reduces the space in the carpal tunnel, including arthritis, the growth of a cyst or compression from everyday activities. The median nerve is particularly vulnerable to compression and is of the most concern as prolonged compression can cause nerve damage and permanent weakness of the hand. How is it treated? There are a few different treatment options for carpal tunnel syndrome. Non-surgical treatment is recommended first, which could include physiotherapy, wearing a splint, cortisone or plasma rich platelet injections to promote nerve healing. The effectiveness of physiotherapy will depend on the cause of your syndrome. If the space of the tunnel has been reduced permanently, such as with arthritis, then surgery is likely to be the most effective treatment. Carpal tunnel surgery is an operation to widen and release the carpal tunnel allowing decompression. This is a common procedure but is not without risks or complications and requires a period of time off work for recovery. For non-surgical cases, altered biomechanics of the arm, the mobility of the median nerve and muscle tightness may all be contributing to symptoms. In this case, physiotherapy can be highly effective, along with a period of rest, possibly splinting and a change in your daily activities. If you have ever suffered from a tendon injury you will know that the recovery can be frustratingly long. Tendons are important tissues of the body, connecting muscles to bones and come in many different shapes and sizes. There are many reasons why tendon injuries can be difficult to treat, as we explain below. Tendon injuries often develop gradually.
Tendons need to be able to transmit forces from muscles to the bones that they attach, however they respond to changes in strength more slowly than muscles do. As muscles become stronger or take on more load, the tendons can fail to keep up with this increased demand becoming painful and damaged. This process can take a while to occur and often changes to tendon tissue has begun long before the pain is noticed. This means that there are likely to be multiple factors to be assessed, including biomechanics and training regimes before the problem can be resolved. Tendons have limited blood supply. Tendons do have their own blood supply, however, it is not abundant as muscles and this can be a factor with healing as all tissues require nutrients for health and to heal. Any condition that compromises circulation, such as diabetes, can predispose tendons to injury and delayed healing. Rest and stretching may not necessarily help. Our instincts in response to tendon pain may not help with recovery. In some cases, stretching can aggravate symptoms and while rest may reduce symptoms, it will not necessarily help with recovery. The best evidence for promoting healthy tendon growth is through addressing poor biomechanics and a tailored strength and loading program. Recovery often relies on adherence to a specific rehab program. One of the biggest barriers to healing tendon pain is that exercises can be easy to do in theory, but hard to do in practice. They can take time and discipline. Your physiotherapist can also help you to find strategies to fit your exercises into your daily routine if you are finding this difficult. Ask your physiotherapist for more information about tendon pain! What is it? The scaphoid is a small bone in the wrist that connects the radius bone in the forearm to the hand, situated near the thumb. Scaphoid fractures are a relatively common wrist injury and are commonly misdiagnosed, as the pain can be similar to a sprained wrist, even when the bone has been broken. Scaphoid fractures are notorious for complications in healing due to low blood supply to the area and how easily their diagnosis can be missed. How does it happen?
A scaphoid fracture is often caused by a fall on an outstretched hand (FOOSH) or a direct blow to the wrist. It is more common in young adults than in children and the elderly. What are the symptoms? Symptoms of a broken scaphoid include wrist pain, swelling, bruising or discolouration of the skin over the injured area and difficulty moving the wrist or hand. As the swelling subsides you might notice pain at the base of the thumb when opening jars or gripping objects. There may also be a deep, dull ache in the wrist that doesn't settle easily. How is it diagnosed? If you suspect that you have a scaphoid fracture, you should consult your physiotherapist or GP who will refer you for an X-ray to confirm if the bone is broken. Occasionally scaphoid fractures will not show up on an X-ray, so if the findings are negative yet your medical team still suspect a fracture, they may wait a week then X-ray again or send you for an MRI or CT scan to double-check. Though these fractures can often be treated without surgery, doctors may recommend surgical intervention for more severe cases or if the bone is not healing well enough on its own. How can physiotherapy help? If you have a scaphoid fracture, your doctor will likely prescribe a splint or cast to ensure the wrist is kept still until healing is complete, usually for a minimum of six weeks. Healing times will vary depending on which part of the bone has been broken. Following the removal of the cast or splint, there is often residual pain, stiffness and muscle weakness. Your physiotherapist can help you restore any deficits as well as resolve any other aches or pains that may have resulted from altered biomechanics. |
Categories
All
|
|
The Physio Nook
197A Scarborough Beach Road Doubleview WA 6018 08 9446 7017 doubleview@thephysionook.com.au |