|
A common fear for people when discussing pain is the idea that their symptoms are 'all in their head' or that they won't be believed by friends, family, therapists or workmates. This fear can be worse when there appears to be no obvious or visible cause for their pain or if it has been present for a long time. What is pain?
Many of the models used in the past to explain pain lead us to believe that the intensity of pain will always be proportional to the severity of an injury. The experience of pain is always real and usually distressing. However, pain is a warning system used by our nervous system to alert us to danger, not a direct indicator of damage done. This is an important distinction, meaning that the experience of pain can be influenced by many different factors and not exclusively tissue damage. How can stress impact pain? Part of the role of your nervous system is to sort through a huge amount of sensory input and interpret it in a meaningful way. When pain is considered to be a serious threat to the body, the intensity of the pain will be worse. This can happen in many situations, such as... -The source of the pain is not well understood, leading to fear that the pain might be something very serious; -The nervous system is in a state of hyper-arousal, such as when you are stressed or tired; -The pain or injury has a significant impact on your quality of life, work, relationships or hobbies; or -The injury occurred through a traumatic event such as a car accident. What does this mean for my treatment? Along with more traditional treatments, we also know that stress reduction strategies, mindfulness and addressing any emotional trauma associated with pain can all help to aid recovery and improve quality of life. Your physiotherapist is a great person to speak to about pain management strategies so you can get the most out of your life while dealing with your pain and injury.
0 Comments
There is more to distance running than you may think. In this article, we offer some words of wisdom from our physiotherapists to help you get the most out of your training and avoid injuries. 1. Choose your shoes carefully:
Repeated stress from running long distances will show up any biomechanical flaws in your body relatively quickly. Choosing the wrong shoes can exacerbate an existing problem causing pain and injury. Your physiotherapist or podiatrist can guide you on what style of shoe will best suit you. 2. Don't neglect your upper body: While running can appear to be a purely leg based activity, increasing the strength and mobility of your upper body can have a surprisingly big impact on your posture, running style, breathing and overall performance. 3. Find time to train strength as well as endurance: Your body is great at finding ways to compensate for weak muscles. However, over time this can lead to overuse injuries of tendons and muscles. Identifying any areas of weakness early and specifically strengthening these muscles can both improve your running technique and efficiency, as well as help keep you injury free. 4. Pace your progress: Entering an event is a great way to set a specific goal and keep you motivated. While trying to increase distances and speed, it is easy to forget to include rest days as a part of your routine. Your body needs time to recover and restore itself just as much as it needs the active portions of your training program. Increasing your speed and distances gradually also allows your body to adapt to new demands without breaking down. 5. Enjoy your training and listen to your body: Your body will often guide you as to when you need to rest and when you can push a little further. Training will be more enjoyable when you are well rested and pain free. Most importantly, if you are able to enjoy your runs, this will help you maintain motivation over a longer period of time, so you can continue for many years to come. Ask your physiotherapist for more tips on how to reach your running goals while staying injury-free. What is it? A broken collarbone, or clavicle, is one of the most commonly broken bones in the body. The clavicle connects the front of the ribcage to the shoulder and is the only bony connection the arm has to the rest of the body. Many muscles attach to the clavicle, including the deltoid and pectoralis Major. How does it happen?
The most common way for this injury to occur is through a fall onto the shoulder. This can happen from a simple fall or sports such as mountain biking or football. It is a common childhood injury but can happen at any age. What are the symptoms? Usually, a broken collarbone will cause moderate to severe pain over the broken area. The patient may have heard or felt a popping or cracking at the time of the injury and there may be an ongoing grinding or creaking with movements of the upper arm. If the skin is not broken there may be bruising and swelling over the painful area. What is the treatment? While very severe cases can be surgically fixed, more often a broken collarbone will be allowed to heal naturally with rest and monitoring. By supporting the arm in a sling and providing pain relief the arm will mend on its own. As with most fractures, there are often other injuries that need to be dealt with at the same time. There are many important structures near the collarbone that can be damaged, including muscles, nerves and blood vessels. In very severe cases, the lung tissue under the collarbone can be damaged causing the lung to collapse. Physiotherapy and recovery: Once a treatment plan has been decided by your medical team, your physiotherapist can help you to return to your pre-injury strength and mobility with a full rehabilitation program. Anterior ankle impingement is a condition where repetitive forces compress and damage the tissues at the front of the ankle, causing pain and inflammation. It is a common injury that can affect people of all ages, however is usually seen in athletes of sports involving repetitive or forceful upward movements of the ankle, such as sprinting, landing from long jump, uphill and downhill running. What are the symptoms?
Pain at the front of the ankle joint is the primary symptom of anterior ankle impingement. This can be felt as an intense, sharp pain occurring with ankle movements or a dull ache in front of the ankle following periods of exercise. Pain can also be felt when putting weight through the ankle while standing, walking or running. Night soreness, stiffness, swelling and reduced ankle flexibility are also common symptoms. How does it happen? Anterior ankle impingement is caused by traumatic or repetitive compression to the structures at the front of the ankle as the tibia and talus move towards each other during ankle movements. The tissues that are affected become damaged and inflamed, causing the pain typical of ankle impingement. Chronic inflammation can lead to further stiffness, exacerbating the impingement process. The most common risk factor for ankle impingement is a previous ankle sprain that was not adequately rehabilitated, as this can result in a stiff or unstable ankle. Another cause of impingement is the growth of small osteophytes or bony spurs around the ankle joint that press against the nearby soft tissues. These can be due to osteoarthritis or grow as a reaction to previous injury. Training errors, muscle tightness, unsupportive footwear and a hypermobile ankle have also been shown to be risk factors for anterior ankle impingement. How can physiotherapy help? Depending on the cause, mild cases of anterior ankle impingement usually recover in one to three weeks with rest and physiotherapy treatment. For more severe impingement, the ankle may require up to six weeks of rest and rehabilitation to recover. In rare cases, surgical intervention will be required to remove any physical causes of impingement such as osteophytes, to restore impingement free movement of the ankle. Your physiotherapist will first identify the cause of your ankle impingement and help you to choose the best course of action to reduce your symptoms. They are able to advise you on the appropriate amount of rest and provide stretches and exercises to restore strength and flexibility to the ankle. Mobilization techniques and range of motion exercises can also reduce stiffness of the ankle, restoring normal joint movement. Balance and proprioception exercises are also included to help prevent further ankle injury. Physiotherapy treatment is definitely the first step before considering surgery. If surgery is required however, your physiotherapist can help you to make a full recovery with a post surgical rehabilitation program. Why are workplace injuries so common? The nature of work is that we are often required to complete the same task for hours. We can also find ourselves faced with time constraints and deadlines that lead to poor postures and taking shortcuts, simply to get the job done. How can they be prevented?
Workplace injuries can happen suddenly, through an accident like a fall or by lifting something too heavy. However, just as many workplace injuries occur over time due to repetitive tasks. Often these conditions begin slowly and take many months to resolve. Here are a few tips to keep yourself pain free in the workplace. Moving Items: It's important to assess any risk before you start. Do you need to ask for help or use an assistive device? Your legs are the strongest part of your body, so ideally you should use them to power your movement, rather than your arms or back. Bending and twisting when lifting is also a common mechanism for injury. It is much safer to lift, then step to turn before putting an object down again rather than twisting on the spot. Also, pushing is a more efficient movement than pulling and is always preferable if you have a choice. Try to push at waist height and keep resistance as close to your body as possible. Office Work: Overuse injuries can occur by always using the same side of your body rather than alternating sides. Practise using both left and right hands for taking phone calls and using your mouse. Be aware of your posture. Good posture isn’t just about having a rigid and upright spine, it’s about being able to let your spine sit comfortably in its natural curves and be able to move in and out of this easily. Stretching can help to counteract positions you find yourself in for long periods, and remember, there's no substitute for regular movement. Set an alarm on your computer or phone every 30 to 45 minutes to stand up and move. A physiotherapist is a great person to speak to about preventing injuries in your workplace, be it about heavy manual work or repetitive, sedentary office work. While pain and stiffness often go together, joint stiffness can occur on its own. Joint stiffness can limit your ability to perform usual tasks, such as turning your head to check behind you while driving. Stiffness can also be a warning sign that a part of the body is vulnerable to future injury. There are many different causes of stiffness and below are some of the reasons why you might not be feeling as flexible as normal. 1. Disuse and lack of movement
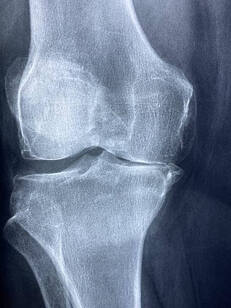
Our bodies are designed to move. When we're not regularly moving our joints through their full range, they can begin to feel ‘tight’. This can be caused by a combination of the capsule that surrounds the joint tightening up and the muscles around the joint shortening and losing flexibility. Stiff and tight muscles can cause you to feel as though your joints are stiff, even if it is only the muscle length that is restricting the movement. Joint mobilizations, manipulation and muscle stretches or massage can have a significant effect in improving the symptoms. The most effective way to maintain full movement is to regularly move joints through their full range, which also helps to keep muscles and joints healthy. Your physiotherapist can advise you on how to best approach this with a targeted set of exercises. 2. Osteoarthritis (OA) OA is a degenerative disease, characterized by a breakdown of the joint surface cartilage and the growth of bony osteophytes around areas of stress. While OA is increasingly common as we age, it is thought that the primary cause is abnormal load and stress to joint surfaces and not simply aging itself. As the space between two joint surfaces become uneven, joints affected by OA can feel stiff or even ‘blocked’. A person with OA will often feel stiff for around 15-20 minutes after being still. Physiotherapy programs to strengthen the muscles surrounding the joints, to help absorb weight-bearing forces, has been shown to have positive results with OA symptoms. 3. Inflammatory Related Stiffness The inflammatory process is characterized by swelling and pain around a specific area. Usually this is a response to damage by the body. As an area swells, this will allow less space for movement and a sensation of stiffness, as anyone who has had sprained an ankle can attest to. Acute inflammation will cause swelling that increases over 24-48 hours and subsides gradually. Autoimmune disorders can cause the body to mistakenly have an inflammatory reaction where there has been no injury, with resulting pain and stiffness. Rheumatoid arthritis and ankylosing spondylitis are two examples of such disorders. Stiffness caused by inflammatory disorders is characterized by a feeling of stiffness after rest, particularly in the morning, that can take longer than 30 minutes to subside. Inflammatory disorders unrelated to injuries are complex in cause and require collaboration with medical teams for best treatment outcomes. Acute injuries are best managed by following RICE protocols (Rest, Ice, Compression, Elevation). What is it? Your knee moves freely backwards and forwards; however, the thought of it moving from side to side probably makes you cringe. This is because the knee joint has sturdy ligaments either side of it that prevent sideways movement and we instinctively know that a lot of force would be required to shift it in this direction. The ligaments on either side of the knee are called the collateral ligaments and they each work to provide stability and restrict the knee’s movement into a sideways direction. The medial collateral ligament (MCL) is found on the inside of the knee and acts to prevent the knee bending inwards towards your other leg. How does this injury occur?
The typical mechanism for this injury is a force that drives the lower leg inwards. This can occur from an awkward landing from a height, or when twisting with a foot fixed on the ground or from an external force hitting the outside of the knee, such as with a football or rugby tackle. What are the symptoms? MCL tears typically create pain and swelling quite specifically on the inside of the knee. The severity of the pain and swelling will be related to the amount of ligament fibres damaged. Larger tears may also make the knee feel unstable or loose. A grading system is used to classify the severity of the injury and help to guide treatment. Grade 1 indicates that a few ligament fibres have been torn and grade 3 is used for a complete tear of the ligament with associated joint laxity. Very severe MCL tears may also involve injury to the medial meniscus and anterior cruciate ligament (ACL) and can require surgical repair. However, most MCL sprains can be managed well with physiotherapy. Grade 1 and 2 MCL sprains take between 3-8 weeks to fully heal and a complete rehabilitation program is strongly recommended to prevent future injury. How can physiotherapy help? In the early stages of the injury, treatment is focused on pain and swelling management, while allowing the body to start the healing process. This is best managed thought the R.I.C.E. principles (Rest, Ice, Compression and Elevation). Following any injury, it is natural for muscles to waste a little and the damaged tissues to lose what we call proprioception, the ability to sense their position in space. This loss of muscle strength and proprioception can contribute to future injury if not restored with a proper rehabilitation program. Physiotherapy also aims to restore movement to the joint and support the ligament while healing to ensure that it is strong and healthy, and the scar tissue forms in an organized fashion, which makes the new ligament as strong as it can be and protects against future tears. What is the labrum of the shoulder? The shoulder is a remarkably mobile joint, however this flexibility comes with the cost of less stability. The glenohumeral joint, where the upper arm meets with the shoulder blade is a ball and socket type joint. The surface area of the ‘socket’ part of the joint (the glenoid fossa) is much smaller than the ball part of the joint (the head of the humerus). A fibro-cartilaginous ring called a labrum surrounds the edge of the glenoid fossa which acts to increase both the depth and width of the fossa. This labrum provides increased stability and is also the attachment for a part of the biceps muscle via a long tendon. The labrum can provide flexibility and stability that a larger glenoid fossa might not be able to, however being a soft structure it is prone to tearing which can be problematic. What causes the labrum to tear?
The most common way the labrum is torn is through a fall onto an outstretched arm or through repetitive overhead activities such as throwing or painting, as the repeated stress on the labrum can cause it to weaken and tear. Suspected labral tears can be diagnosed in a clinic by your physiotherapist through a series of tests, however, an MRI is usually required to fully confirm the presence of a labral tear. Labral tears are classified into different grades, which are determined by their location and severity. This grading is used as a guide to help determine the correct treatment. What are the symptoms of a labral tear? A labral tear is often associated with other injuries, such as a rotator cuff tear, which can make the clinical picture a little confusing. Commonly there will be pain in the shoulder that is difficult to pinpoint and the pain will be aggravated by overhead and behind the back activities. Severe labral tears can lead to instability and can also be related to dislocations of the shoulder. How Can Physiotherapy Help? The severity and grade of the labral tear will guide treatment. Smaller tears can be treated with physiotherapy that is aimed at increasing strength and control of the shoulder. Other tears may require surgical repair after which physiotherapy is an important part of treatment to rehabilitate the shoulder. A serious injury of the knee is a tearing of the ACL (Anterior Cruciate Ligament). This ligament is important for stability of the knee and may need to be repaired surgically. The primary function of the ACL is to keep the bottom surface of the knee joint from sliding forwards during movement. An unrepaired knee may feel unstable or give way suddenly. Not all ACL injuries require surgery and some may heal well with proper rehabilitation, however for those who do need surgery, there is a significant rehabilitation period afterwards. What does the surgery consist of?
Each surgeon will have a slightly different technique for surgery. The most common approach is the arthroscopic approach, which uses a small camera and allows the surgeon to make only small incisions into the knee. They will then replace the torn ligament with either a graft from a tendon or ligament at another part of the body or using a synthetic graft. How long does rehabilitation take? Full rehabilitation following surgery can take 9 to 12 months and is divided into different stages. As surgeons can have different protocols for their approaches to surgery, time frames will vary for everyone. Initially after surgery, the graft will be quite weak while a new blood supply is being established. It can take up to 12 weeks before the graft is at its strongest point and evidence suggests that it may never have the strength of the original ligament. In the early stages, rehabilitation will be focused on restoring movement to the joint and strengthening the muscles around the knee without putting any undue stress on the graft. As the graft begins to heal and strengthen, rehabilitation can progress to include stability and control exercises and gradually build up to a complex program that prepares the knee for a full return to sport. The path to full rehabilitation from a knee reconstruction can be a long and bumpy one, however, there are high success rates with this surgery, particularly when followed up with full physiotherapy rehabilitation. What is Sever’s Disease? Sever’s disease is a condition that causes pain in the heel of children and adolescents. While it can be quite painful, it is a self-limiting condition that doesn’t usually cause any long-term problems. Sever’s disease is quite common and is the leading cause of heel pain in children and young adolescents. Also known as calcaneal apophysitis, Sever’s disease is an inflammation of the growth plate of the heel. A growth plate is the area of bone where new bone is produced in the growing skeleton and is often weaker than other bony areas. Repeated or excessive stress on this area can cause it to become and inflamed and painful. What are the symptoms?
Children might complain of heel pain that is worse when walking, running or jumping. This may be present following an increase in activity or after a growth spurt. Pain may also be felt when walking on heels. Why does this happen? The achilles tendon attaches to the back of the heel, just next to the growth plate and puts force through this area during movement. If this force becomes too great, the growth plate can become irritated, starting a painful inflammatory process. While increased activity is a predisposing factor, other things may also contribute, such as reduced movement of the ankle, abnormal foot movements when walking and tight calf muscles. It is also possible that Sever’s disease can appear with no obvious cause. What is the treatment? While this is a self-limiting disorder that will go away on its own as the skeletal system completes growth, it can be quite painful and this may impact your child’s activity levels and gait pattern. To prevent any long-term issues from adaptations or changes in activity levels, your physiotherapist can work with your child to find solutions that allow maximum movement with minimum pain. Most of the time, simple education and relative rest or ceasing of aggravating activities are effective. Studies have also found that properly fitted orthotics can help reduce pain while maintaining activity. Physiotherapists can also address any factors which may have caused excess stress in this region, such as abnormally tight muscles or poor gait patterns. They can also advise of pain-relieving treatments and alternative forms of exercise if necessary. None of this information is a replacement for proper medical advice. Always see a medical professional for advice on your injury. |
Categories
All
|
|
The Physio Nook
197A Scarborough Beach Road Doubleview WA 6018 08 9446 7017 doubleview@thephysionook.com.au |