|
The lower part of the leg, from the knee down to the ankle consists of two long bones that sit side by side- the thicker tibia and the thinner fibula. The bones are joined together by thick fibrous connective tissue called a "syndesmosis" and are firmly attached to each other with just a small amount of movement between them, allowing for a small amount of rotation of the ankle. A fracture of the fibula occurs when the bony tissue is disrupted or broken. It is a common injury and can occur at any part of the bone, depending on the mechanism of injury or the state of the bone. How does it happen?
A fracture of any bone can occur when the force applied to any point exceeds the strength of the bone at that point. However, as with all fractures, there are common patterns that are seen based on structural points of weakness in the bone and common patterns of movement. A few common ways that the fibula is broken are... Blunt force: If something hits the bone hard enough, it will break on impact. This could include being hit by a ball hard enough or being hit by a car, as this is the site where a car's bumper would reach. Impacts like this that have enough force will often break both the tibia and the fibula at the same time. Skiing accidents where skis hit something suddenly or get stuck can also cause the bones to break at the upper level of the ski boots. Ankle Sprain: When it comes to the fibula, the most common reason for the bone to be broken is during a severe ankle sprain. The ligaments that attach the outside of the foot to the fibula are so strong that when you twist your ankle badly enough, sometimes it is the bone that breaks. This is one of the most commonly missed injuries, partly because the fibula is not a weight-bearing bone. This means that after the initial pain and swelling have subsided, you can still walk on your foot without pain stopping you. It is important to have any severe ankle sprains imaged by X-ray to rule out any fibula fractures. What are the symptoms? In some cases, the symptoms of a fibula fracture will be unmistakable, with severe pain. Sometimes the skin will be broken and there will be bleeding. If the bone has been moved from its usual position, there will be a deformity such as a bump or dip under the skin. For smaller, undisplaced fractures, there will be pain over the bony aspects and a constant, deep pain that is worse when weight-bearing. What is the treatment? Physiotherapists are often the first to notice fractures caused by ankle sprains. Once a fracture has been confirmed, your medical team will decide on the best course of action to allow the bones to heal. This might include surgery to pin the bones together, casting or the use of a moon boot. Following a period of immobilisation, your physiotherapist can help you rehabilitate the surrounding tissues. This will include muscle strengthening, joint mobilisation, balance and control retraining, and a stretching program.
0 Comments
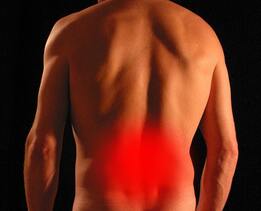
If you've been unlucky enough to suffer from chronic or persistent back pain, chances are that at some stage you've had scans to capture what is happening inside your spine. Magnetic resonance imaging (MRI) is an incredible technology that can provide valuable insights into tissues that otherwise can't be seen. Unfortunately, there are some common misconceptions around what that information means, which can sometimes be unhelpful and even harmful to recovery. Here are a few things you might not realise that can help you understand your MRI... Not all tissues show up on every scan.
Muscle, fascia, or other irritable tissues may not show up on your scan, meaning you may experience a lot of pain but have a completely normal scan. Not all parts of your anatomy will show up from every scan's perspective and some tissue changes might only be evident in certain postures. Age-related changes are normal and may not be related to your pain. Results such as arthritis, disc bulges, and small tears can be concerning. However, it's helpful to note that people who have no painful symptoms can have similar, if not more, age-related changes and these signs may not be related to your pain at all. Severe pain may not be related to severe changes on MRI. Pain is a complex experience, influenced by multiple factors including the sensitivity of the tissues involved, what the brain believes about the pain and what it means, and how long it has been present. MRI is helpful for ruling out severe pathology such as infection, fracture, or malignancy, but it is not always an accurate guide to the source of symptoms. The results of an MRI should always be taken into account as a small part of a bigger clinical picture when guiding treatment. Talk to your physiotherapist for advice on any imaging results you have and what they might mean for your treatment and prognosis. None of the information in this article is a replacement for professional medical advice. Always consult a medical professional for advice on your condition. While there are many benefits to be gained from effective stretching, employing an improper technique can actually result in injury. Here are some tips and guidelines for you to follow when stretching... - Warm up first with an activity such as walking (at least 5 -10 minutes).
- Stretches should be pain-free. You should only feel tension or a tight feeling when stretching. If you feel a sharp pain, this means you're stretching too far. - Don't hold your breath while stretching, keep breathing to ensure the muscle tissues remain oxygenated during the stretch. - Stretch both sides. But if one muscle is tighter than the other, focus on it more until they're both in the same range. - Avoid bouncing at the end of the stretch because it may lead to injury. - Hold stretches for 20-30 seconds, if not longer. A 10 second stretch is not always enough to achieve a lasting effect. - Repeat the stretch 3-5 times with intermittent rest periods in between. - Make sure your body is aligned properly and observe good posture. When to Stretch? Traditionally, stretching has been encouraged before and after any kind of physical activity. However, recent studies show that there is no discerning difference between whether you stretch before exercise/sports or not, both in terms of performance and injury prevention. In some cases, researchers say that it's okay to omit the pre-event stretch since the post-event stretch is much more beneficial. Some of our everyday postures and activities can lead to certain muscles becoming tight while the others sit in a lengthened position. These habitual postures that lead to muscle imbalances then become more and more difficult to correct over time. Many therapists will suggest that stretching all muscles generically isn’t as beneficial as identifying which of your muscles are abnormally tight and developing a targeted stretching regime. Talk to your physiotherapist for advice regarding the best stretching program for your body type, posture and activity levels. What is it? Vertigo, the feeling that you are moving even though you aren’t, is an unpleasant yet common experience caused by a variety of conditions. It may surprise you to learn that in some cases your physiotherapist is able to treat vertigo. The process of telling whether we are moving or not involves many parts of the nervous system, including the inner ear. The vestibulocochlear nerve sends information about head movement to the brain, where it is processed. However, certain conditions can disrupt this process, causing the brain to perceive movement when there is none. Physiotherapists may be able to help with a specific type of vertigo called Benign Paroxysmal Positional Vertigo (BPPV). What are the symptoms?
BPPV, also known as positional vertigo, causes dizziness only when the head moves in certain positions or directions. People with BPPV often experience dizziness and nausea when rolling over in bed or looking upwards, as well as lightheadedness and disturbance of balance. While BPPV can occur for no obvious reason, it is often seen after a recent head trauma, respiratory infection, or aeroplane travel, as these conditions can disrupt the inner ear's normal function. How does it happen? The symptoms of BPPV can be explained by a disruption in the signal sent by the semi-circular canals of the inner ear to the brain. These canals are positioned in different directions and filled with fluid. As the head moves, the fluid in each canal moves differently, depending on the head's orientation. Receptors pick up this movement direction and speed, sending the message to the brain. However, sometimes small calcium crystals in the utricle, where the three semi-circular canals meet, can become dislodged and move into the semi-circular canals, disrupting the fluid and obscuring the messages to the brain. What is the treatment? If your doctor has diagnosed you with BPPV, they or your physiotherapist can show you a series of movements to help dislodge the calcium crystals and move them away from the semi-circular canal. You may also be asked to perform exercises to prevent the crystals from returning. Usually, only one or two treatments are needed for symptom resolution, although some cases may require more. If you think you have vertigo, it is important to be assessed by a medical professional, as there are many conditions that can cause these symptoms and correct diagnosis is necessary before treatment. None of the information in this article is a replacement for proper medical advice. Always see a medical professional for advice on your condition. Maintaining balance is a complex process that your body does automatically. The body uses various systems to maintain balance, where if one system fails, the others can compensate to keep you stable. You may not notice a deterioration in your balance until you're in a challenging situation. Our bodies have three systems that work together to keep us balanced: our vision, our inner ear, and our proprioception (our ability to sense the position and movement of our joints, muscles, and tendons). Our eyes provide visual information about the world around us, while the inner ear helps us maintain our balance by detecting changes in our head's position. Meanwhile, receptors in our joints, muscles, and tendons help us understand where our body is in space and how it is moving.
Poor balance can cause falls, broken bones, and serious injuries. The good news is that you can usually improve your balance with just a little practice. Here are a few quick tips you can try... 1. Maintain good posture. Good posture helps align your body, which is important for balance. Stand up straight with your shoulders back and head up. Avoid slouching or leaning to one side as it can throw off your balance. 2. Practice standing on one leg. Standing on one leg may seem easy, but it can be challenging if you're not used to it. Start near a wall or hold onto a sturdy surface for safety. Gradually try standing on one leg without support. This exercise improves proprioception, which is your body's ability to sense where it is in space. 3. Strengthen your core muscles. Core muscles located in your abdomen, back, and hips help stabilize your body and keep you upright. Strengthening them through exercises like planks, side planks, and bridges can improve your balance. 4. Regularly challenge your balance. Notice what the limits of your balance are and see if you can improve on this gradually every day. Setting small goals for yourself can result in large improvements in your balance over time. Talk to your physiotherapist about creating a personalised program to improve your balance. Your physiotherapist is an expert who can evaluate which aspects of your balance need improvement and how to do it. They can assess which exercises are most appropriate for you, regardless of your fitness level or age. Joint and/or muscle stiffness can be felt in any part of the body. While it may be accompanied by pain, this is not always the case and it can have many different causes. Feelings of stiffness can be easy to ignore, however, they can be a sign that you're at increased risk of injury or pain. Here are a few reasons why you might be feeling a little bit less flexible... Muscle Weakness
Muscle stiffness can be a sign that strength is lacking. Our body will prioritise stability over flexibility if our muscles don't have the ability to provide both. This means that your muscles will be a bit tighter and stiffer to compensate for any weakness. If you are feeling a tight and sore, your physiotherapist can help to identify any muscles that maybe need targeted strengthening to help. Delayed Onset Muscle Soreness (DOMS) Many of us are familiar with post-exercise pain and stiffness. This is a somewhat protective mechanism to help you recover from a bout of increased exercise. This kind of stiffness will be present in muscles that have been used recently and usually lasts for just a day or two. DOMS usually goes away on its own, although it can be quite uncomfortable, it is usually nothing to be too concerned with. Your physiotherapist can help you with tips to avoid DOMS in your regular workouts. Lack of movement Along with muscle weakness, inactivity can lead to joint stiffness. Joints need to move through their full range regularly to maintain their flexibility, as anyone who has kept a joint immobilised in a plaster cast will know! Lack of movement can lead to a reduction of blood flow and nutrients, also impacting joint health. Your physiotherapist can help you to identify any joints that are not moving well and advise you on how to restore joint flexibility. Activities such as Pilates aim to help you move all of your joints through their full range safely and maintain flexibility. Arthritis Stiffness is the hallmark of arthritis, often noticeable as increased stiffness on waking that progresses gradually over time. Pain and stiffness caused by arthritis can often be helped by a targeted muscle strengthening program to help support the joints. Speak to your physio about any tightness or inflexibility and see how they can help you feel your best. We know many of the habits that shape our adult lives are set in childhood. Physical activity is important for a growing body as movement and weight bearing have a large impact on bone strength, muscle and tendon health. Here are some tips to make sure your child is staying as active as possible. 1. Find an activity that suits your child.
Children who are coordinated and excel in competition may find team sports both increase their self-esteem as well as keep them fit. For other children, being a part of a team can be uncomfortable. Less competitive children may prefer a sport where success is measured by improving on their own performance, rather than being compared to other children. Surfing, yoga, martial arts, dancing or gymnastics may be activities that suit your child if competitive and team sports cause them to be discouraged. 2. Do get injuries checked out by a professional and invest in proper rehabilitation. While children do bounce back quickly from injuries, they also may have difficulty expressing pain and discomfort. A niggling pain that won’t go away may cause your child to say “I don’t like sport” rather than realising that they are in pain. Some children may retain worries that they will hurt themselves again because of a previous injury and avoid exercise. Your physiotherapist can help to identify any issues that your child is having and help to resolve them. 3. Set fun and challenging goals for them to complete during their daily routine. As less children are walking and riding to school, try to find ways to fit extra activities into the day. Some fun examples include running a daily long jump competition in the back yard or adding a routine of age appropriate exercises, such as star jumps, hopping, balancing and running on the spot. You can make these exercises part of the night or morning ritual, just like brushing your teeth. What is it? Headache is a generic term for any pain in the cranial region. They can be caused by a variety of factors and there are many different types. A severe headache can stop you in your tracks and be severely debilitating. One kind of headache that is commonly treated by physiotherapists is cervicogenic headache or a headache that originates from the neck. What are the symptoms?
The pain of a cervicogenic headache is usually unilateral (on one side), and often described as a dull or aching pain that can be felt in the neck, head, face or even behind the eyes. It can also be accompanied by other symptoms such as neck stiffness, limited range of motion in the neck, and tenderness in the neck or scalp. How does it happen? Cervicogenic headache is an example of referred pain, where dysfunction of the structures in the neck cause pain to be felt in a different location. The most common reason for this pain to be felt are joint and muscle stiffness around the cervical spine. Tight muscles can develop trigger points that refer pain into the cranial region in a typical pattern. Headaches can also be caused by irritated nerves that originate in the spine and travel into the head. Whiplash following a trauma such as a car accident is known to be a cause of ongoing neck-related headaches. How is it diagnosed? Diagnosis of a cervicogenic headache can be difficult as it needs to be differentiated from other forms of headache such as migraine, tension headaches and sinus headaches. Your physiotherapist will perform a thorough assessment to determine the origins of your headaches. Some signs that headaches are caused by cervical dysfunction include muscle tightness, joint limitations, concurrent neck pain and poor posture. What is the treatment? Treatment for neck-related headaches is aimed at correcting any dysfunction, restoring movement and flexibility to stiff joints and muscles and addressing any postural issues. Travel can be one of the most enjoyable aspects of life. However if a trip away comes with the risk of increased pain and soreness, the excitement can be thoroughly diminished. Some people may avoid travel altogether if their symptoms are exacerbated too much by long periods of sitting in a car or aeroplane. If you are unlucky enough to fall into this category, here are a few tips from your physiotherapist that might help make long trips a little more comfortable, particularly if you tend to suffer from lower back pain... 1. Adjust the seat angle.
If you are able, tilt the seat slightly down towards your feet, not towards your hips. Ideally, your knees should be level with your hips, or even slightly lower. A footrest to lift your knees can also help. 2. Lift the height of the whole seat. This will assist with tip number 1 by lifting the whole body away from the floor. When your hips are less flexed, it is easier for your back to sit comfortably in an upright position. 3. Use a lower back support. Many cars nowadays come equipped with in-built lumbar supports. Often this support is a generic design and not fitted for your specific shape or height. A proper lumbar pillow, or even a rolled towel in the small of the back, can be more effective in maintaining the natural arch of your spine. This eases pressure on your intervertebral discs, spinal ligaments and muscles. Neck discomfort is easier to improve when tips for lower back are implemented first. Some other simple tips to reduce neck pain are as follows... 1. Use a travel pillow. If travelling on an aeroplane, try wearing the pillow backwards or sideways. This assists in supporting the head in a slightly better position when you rest or sleep, which helps to reduce the stress placed on the muscles, ligaments and joints of the neck. 2. Every hour, perform 10 chin tucks. This is easiest to perform correctly if you sit tall and press your chin straight backwards, lengthening the back of your neck. Do not tuck the chin to the chest. This exercise stretches the small postural muscles at the base of the skull, helping to relax them. If you find these tips helpful, continue performing them throughout your travels and enjoy your time away! One of the most impressive healthcare developments in history is the joint replacement. Many people are able to take out a joint that is extremely painful and dysfunctional and give it a whole new lease on life with a surgically inserted prosthesis. The improvements in this type of surgery over recent years have meant that success rates for joint replacement surgery, particularly hip and knee replacements are higher than ever. If you are struggling with joint pain related to arthritis, it can be difficult to know when to start thinking seriously about surgery. Here are a few things to consider before going for that surgical opinion... Don't assume pain is permanent once you hear the word arthritis
Pain is complex and is often not caused by one single thing. Most people will have some amount of arthritis in their joints past the age of 50, whether or not this is what is causing your pain will be unclear without first seeking assessment and treatment. Many people have some level of degeneration in their joints without experiencing much discomfort at all, as a normal part of the ageing process. It's possible that a combination of strengthening and manual therapy could improve your symptoms significantly, even if osteoarthritis is present. A trial of physiotherapy is recommended before surgery in most cases. Pre-surgical strength and fitness are important This means two things. First of all, your strength before surgery will set you up for much better post-operative results. The second thing is that choosing when to have the surgery means not necessarily waiting until the pain is unbearable before going ahead, as time spent in significant pain can reduce your overall strength and fitness while also putting more stress on other joints. Research the risks and side effects While surgical outcomes are continually improving, no surgery comes without risks and some people will have ongoing pain and stiffness even after their operation. It is important to make an informed decision about when and if you should have a joint replacement. If you are considering a joint replacement, speak to your physiotherapist about all the ways they can support you through your journey and help you come to an informed decision about what is right for you. |
Categories
All
|