|
For most of us, the hours we spend sleeping are simply a time for rest and recovery. However, you might be surprised to learn that your sleeping position can have a significant impact on your body, particularly if you already have an injury. Here are some tips to help to stay pain free overnight. Back pain tips:
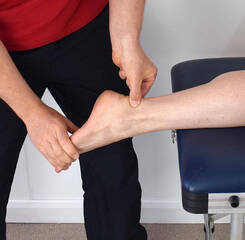
For sufferers of back pain, finding a comfortable position at night can be difficult. The natural curves of the spine need to be maintained and supported throughout the night. Ideally, your body should be held in a position of minimal stress while sleeping. This means that all your joints and muscles are resting in a neutral position A mattress that is too soft might feel comfortable to begin with, but over time will let you sink into it too much, meaning the curve of the lower spine will be lost. Waking up with a stiff or sore back could be a sign that you are using the wrong mattress. A mattress that is too firm can also mean your spine is held in a flattened position, which is both uncomfortable during the night and when you wake up. For many people, sleeping on their side keeps their spine in a more natural alignment than sleeping on their back, especially if they put a pillow between your knees. If you do sleep on your back, placing a pillow under your knees can help to maintain your lumbar spinal curve throughout the night. This can also help to reduce hip and knee pain. Neck pain tips: The neck is often the most vulnerable part of the body if your sleeping setup is not ideal. Side sleepers may let their neck fall excessively to the side with a pillow that is too low or have their neck elevated too much by having their pillows too high. If you find yourself putting your arm under your pillow while you sleep, it is likely that your pillow is too low. Having your shoulder in this position overnight can put unnecessary stress on the structures around the shoulder joint and should be avoided if possible. Stomach sleeping can also put additional pressure on your neck as it is turned to the side for long periods. Hip pain tip: Side sleepers often spend their nights with one leg crossed over their body. This can place extra pressure on the structures on the side of the hip, such as tendons and bursa and can impact the health of these tissues as the compression reduces the blood flow to the area. Placing a pillow under your knee while sleeping on your side in this position can help to maintain a neutral alignment of your hip. Speak to your physiotherapist for more advice on how to improve your sleeping posture and find out if your sleeping setup is right for you.
0 Comments
An essential component of physiotherapy treatment is your home exercise program. All physiotherapists know that patients who complete their exercises will have better outcomes from their treatment, however it can be difficult to find time to complete them. Here are a few tips that can help you to fit your exercises into your weekly routine. Plan when to complete them
Making a plan might sound simple, but the expression 'failing to plan is planning to fail' has some truth to it. Physiotherapy exercises are specifically targeted towards weak and tight muscles. The exercises are likely to be a little difficult and uncomfortable. Setting a particular time aside in advance to complete them can help you overcome any resistance to getting them done. Ask your physio to prioritise them Your physiotherapist might give you a combination of exercises to complete. If you're struggling to find time to complete them all, ask your physiotherapist to rank the exercises in order of importance, this can help you to make sure you complete the most important ones when you are short of time. Set triggers as reminders You can use small every day tasks as reminders to remind you to complete your exercises. Some examples include boiling the kettle, brushing your teeth or as a final task before getting into bed. Use positive reinforcement Combining a task you don't enjoy with one that you do is a great way to motivate yourself. You can either pair your exercises with something you love such as watching an episode of your favourite tv show or give yourself a reward once they are completed. Either way, the more positive associations you make with completing your home exercise program, the less barriers you make to completing them! Want more tips? Ask your physiotherapist for their top tips and tricks for fitting your exercise program into your day. Strains and sprains are words that are used almost interchangeably when describing injuries, however they each have quite distinct meanings. The most straightforward explanation is that a “strain” refers to an injury in a muscle or tendon, while a “sprain” refers to an injury to a ligament. Here we describe what that means and how we treat strains and sprains differently. Ligaments are fibrous tissues that connect and hold bones to other bones at your joints. These are very strong parts of your anatomy and provide large amounts of support and stability to the body.
Some ligaments are so strong that sometimes a bone will break before the ligament will tear. When ligament fibres do tear, the nearby joint can feel unstable as it has lost some of its structural support. A torn ligament will usually become painful and swollen, it may appear red and warm to touch and occasionally there will be some bruising. The pain will be worse with movement or if the ligament is placed under more stress. Occasionally, if a ligament has torn all the way through, the pain will not be as severe as it is with a partial tear. Your physiotherapist can grade the severity of a ligament sprain, which will help guide treatment and expected recovery times. Muscle strains are easy to confuse with ligament sprains, however, there are a few tell-tale differences. Following a muscle tear, it is more likely that you’ll feel weakness rather than instability. The pain will also be isolated over the muscle, rather than near a joint. An injury to a ligament will be tender over the site of the ligament and special tests can be done to test for any joint laxity. Treatment is also slightly different as sprains will need more support and will sometimes even need to be taped or braced, whereas muscle strains will benefit from gentle movements earlier. In both cases, following the basic principles of rest, ice, compression and elevation is great advice in the early stages of any injury. Applying heat is not recommended until at least two or three days after the injury. It is important to seek a professional opinion when recovering from both a strain and a sprain. It is very easy to re-injure an area while it's healing if undertaking too much activity too early and without correct rehabilitation. Speak to your physiotherapist for more information. If you've ever started a new hobby or activity and noticed your balance isn’t quite up to scratch, it can be quite a disturbing discovery. Balance is an important part of many activities and if it's not being challenged regularly, it's easy for it deteriorate without you noticing. What is balance?
Keeping your balance refers to a state where your centre of gravity is maintained over your base of your support, preventing you from falling. Your body is always working hard to keep this equilibrium without you realising it. Balance is controlled by many systems that work together, including the visual, vestibular, proprioceptive and musculoskeletal systems. What is proprioception? Proprioception refers to the awareness of your body’s position in space. The central nervous system gains sensory input from the muscles, skin and tendons and interprets this information, creating a sense of where your body is positioned. This is how you know your foot is flat and ready to take your weight when you step, without needing to look at it. You may not have heard of proprioception before, but it is vital to keep you from falling and can be improved. How can I test my balance? Your physiotherapist is able to assess your balance more extensively, however here are a few quick tests you can do at home to see if your balance can be improved. Stand with two feet together and close your eyes. Try again, this time standing on one foot with your eyes open. Close your eyes only once you have found a steady posture with your eyes open. To increase difficulty, stand on an uneven surface, like a pillow on the floor. Aim to balance for at least 30 seconds in each of these postures. If you can't have a chat with your physiotherapist and see if your balance can be improved. They will also be able to offer you some practical tips on how to reduce falls and injuries. Running is a great way to stay in shape, manage stress and increase your overall health. However, it’s not without potential drawbacks. While generally being a low-risk activity, there are a few injuries that commonly affect runners. As running is a repetitive impact activity, injuries can develop slowly and if left too long, then be difficult to treat. Here are three of the most common conditions faced by runners... 1. Runner’s Knee:
Runner's knee is a persistent pain on the inside of the knee caused by the dysfunctional movement of the knee-cap during movement. The knee-cap ideally sits in the centre of the knee and glides smoothly up and down as the knee bends and straightens, in a process described as tracking. If something causes the kneecap to track abnormally, the surface underneath can become worn, irritated and painful. The pain might be small to start with, however left untreated, can make running too painful to continue. 2. Shin Splints: Shin splints (medial tibial stress syndrome) is a common condition characterised by a recurring pain on the inside of the shin. While the cause of this condition is not always clear, it is usually due to repeated stress where the calf muscles attach to the tibia (shin bone). Why this becomes painful is likely due to a combination of factors that can be identified by your physiotherapist to help you get back on track as soon as possible. 3. Achilles Tendonitis (tendinopathy): The achilles tendon is the thick tendon at the back of the ankle that attaches the calf muscles to the heel bone. The amount of force that this tendon can absorb is impressive and is vital in providing the propulsive force needed for running. If the stresses placed on the tendon exceed its strength, the tendon begins to break down and become painful. Your physiotherapist is able to assess any factors that may contribute to this issue, including footwear, training errors and any biomechanical concerns. Seeing a physiotherapist is an important investment in your health and recovery from pain or injury. Here are a few tips to help get the best outcomes from your treatment sessions... 1. Know what your goals are and ask questions.
If you are clear on what you hope to achieve through physiotherapy, this can help you and your therapist to work together to direct treatment towards these goals. Understanding your condition also plays an important part in recovery, it means that you can make better choices to protect your body and and allow it to heal, and you will know better how to prevent future injuries. Before each treatment, it can help to take a few moments mentally to prepare some questions and consider what your short and long-term goals might be. 2. Do your exercises. Targeted home exercises are almost always an essential part of your recovery as they help your body to support itself through healing and recovery. Exercising is an important way to help correct biomechanical imbalances and reduce excess stress on body structures, as well as helping tissues to strengthen as they recover. 3. Follow your therapist's recommendations. Throughout your recovery, your therapist will guide you as to which activities you should avoid and how much rest to take. Return to sport and activity should be gradual, so as not to stress the body too much too soon when it is still healing. Rest is just as important a part of recovery as strengthening. Following the advice given by your therapist can ensure that you don't injure yourself again and that you get the most out of your body. 4. Be patient with your progress. It can be frustrating waiting for your body to heal. Returning to sport too early or giving up on treatment are common mistakes that lead to further injury or impaired healing. Recovery takes time, a general rule is often that the longer a condition has been present, the longer it will take to resolve. If there is a part of your condition or injury that you are struggling to understand, be sure to seek clarification with your physiotherapist. Two-way communication is key. Our muscles obviously play an important role in the movement of our body. Without them, we wouldn’t be able to bend our elbow or straighten our leg. As our muscles are soft and designed for flexibility, they are also prone to injury and if you have ever torn a muscle, you know that they can be very painful. In the period following a muscle tear, there are a few mistakes we often see people make that can make their injury worse and delay healing times. Here are a few of the most common mistakes we see... 1. Stretching
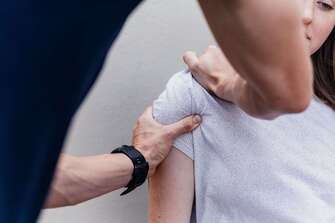
After a muscle tear, the damaged fibres slowly begin to heal and reattach to each other. This process can be quite fragile and during the early stages, aggressive stretching of recovering tissue can impair healing or even lead to more tearing. While gentle stretching a few days after the injury can have a positive effect, you should check with your physiotherapist to ensure you’re not stretching too far and causing further damage. 2. Applying H.A.R.M. Most of us are aware of the acronym R.I.C.E (rest, apply ice, compress the area and elevate) as the recommended treatment in the early stages of an acute injury. The acronym H.A.R.M is less well known and is used to remember the things you shouldn’t do after an injury. This stands for applying heat, drinking alcohol, running or massage. All of these activities can increase swelling, pain and increase the damage of the injury in the first 48-72 hours. 3. Failing to see a physiotherapist The diagnosis of a muscle tear might seem straightforward, however, there might be more going on than you realise. Many conditions can mimic a muscle tear, or you may have suffered a tear due to an underlying weakness or pathology. Having a physiotherapist confirm your muscle tear and identify any other issues is vital to ensuring you recover fully. Your physiotherapist is also able to identify any factors that could lead to further injury and is able to help restore your tissue to its previous level of strength and function. 4. Returning to sport too early One of the most confusing things about muscle tears is that they often become less painful while the tissues are still not completely healed. Many people suffer another tear simply because they return to sport too early. While you may feel as though your tissues are back to full strength, the muscle fibres can still be healing and vulnerable to further injury. It is important to test your injury gradually, starting with gentle exercise and building up to more high intensity activities. Your physiotherapist is able to guide you with a full rehabilitation program. This can help to restore strength, flexibility and control to your damaged muscle, keeping you injury free for the future. What is it? The AC (acromioclavicular) joint is a thick fibrous joint that connects the top of the shoulder blade to the outer end of the collarbone. The joint is required to be strong and supportive and is the primary way in which weight-bearing forces are transferred from the arm to the rest of the skeleton. The joint is connected by three strong ligaments, the acromioclavicular, corococlavicular and corocoacromial ligaments. How does this injury occur?
The primary mechanism that will cause this joint and its ligaments to be injured is a force that separates the shoulder away from the collarbone, usually in a downwards direction. This can occur from a fall into the ground where the top of the shoulder hits the ground first, a rugby tackle or a fall onto an outstretched hand. As with all injuries, there are many variations in severity and a grading system has been developed to classify AC joint injuries. What are the symptoms? After an AC joint injury, there is usually immediate pain on the top of the shoulder, often with swelling and bruising. There is usually some loss of movement of the shoulder and pain from putting weight through the arm or carrying heavy objects. In severe cases, there is a visible lump on top of the shoulder known as a ‘step deformity’, where an obvious height difference can be seen between the top of the shoulder and the collar bone. There is frequently pain felt when reaching across the body, such as when putting on a seatbelt. To confirm the diagnosis, your physiotherapist can perform some clinical tests and sometimes an X-ray can help to grade the severity of the injury. The classification that would be given to you by your physiotherapist or doctor helps to determine the optimal course of action for each injury. There are different classification systems, some use four grades and the other six. Injuries with a smaller number of ligament fibres being torn are given a lower grade classification, going upwards as further damage is incurred. Injuries classified as higher grades will require surgical repair. How can physiotherapy help? The role of physiotherapy in this case is to ensure the joint is supported and given a chance to heal naturally while maintaining strength and movement of the shoulder girdle. This is done initially by providing support to the joint. You may need to have your arm supported in a sling or brace for some of this time, or your physiotherapist can show you some taping techniques to add support. Most AC joint sprains take around six weeks to fully heal, although some patients report ongoing shoulder problems years later. For this reason, a comprehensive rehabilitation program is very important. More severe sprains or total separations may require surgery to stabilise the joint and treat any associated fractures. Surgical repair will also require a proper rehabilitation program afterwards. Osteitis Pubis is a medical term used to describe sports-related groin pain. Osteitis means ‘bone inflammation’, while pubis refers to the specific bone that is affected: the pubic bone. Osteitis pubis is usually an overuse injury that can sometimes be triggered by a specific event. It is characterized by pain deep within the front of the pubic bone, caused by inflammation. The area of the pubic bone affected is specifically known as the pubic symphysis. This type of injury is common in load-bearing athletes such as runners. Other people commonly affected include soccer players and footballers, due to their frequent kicking actions. How does it happen?
Instability around the pelvic region is the primary cause of Osteitis Pubis, particularly if the instability occurs at the connection between the two sides of the pubic bones at the front of the body. The pelvis carries the weight of the upper body and is responsible for providing stability when walking, running and kicking. This means that the joint can become irritated and inflamed. What are the signs and symptoms? Osteitis pubis is aggravated by weight-bearing activities, with running and kicking being the two main culprits. Pain is usually experienced on one side, however both sides can be affected. The pain is usually located at the front of the pelvis and may progress into the hip and groin area as it becomes more severe. Sufferers of Osteitis Pubis may have a history of a previous groin strain, as well as lower back pain. They may also have a history of a sports hernia in the hip area. As with most inflammatory conditions, the pain may be worse when in use, better when resting, and worse overnight into the morning. How can Physio help? Your physiotherapist can help this condition in several ways and will aim to get you back to your pre-injury sporting level. During the assessment, your physio will look at many different things to determine the cause of the condition. Muscle length, muscle strength and muscle control will all be assessed. Your posture in standing, walking and running can also be assessed to determine any irregularities. Your physio will ask you to rest from sports for some time to allow some bony healing to occur. They will then progress you through a rehabilitation program aimed at getting you back to sport. This rehab program will retrain your muscles to stabilise the pelvis when walking, running and kicking. The muscles will also need to have relatively equal flexibility to help stabilize the pelvis. Your physio will give you specific exercises to target the strength and flexibility of these muscles. Finally, your physio will progress you to running or kicking, and allow you to gradually return to sport over a 3 to 6 month period. The "socket" of the shoulder joint is surrounded by a ring of flexible connective tissue, known as a labrum. This labrum increases the stability of the shoulder while allowing the joint to stay flexible. The long head of the biceps tendon has an attachment directly into the labrum, which is often a point where injuries occur. A tear of the labrum can occur in many locations, however the most common is at the point where the biceps tendon attaches. Usually, this tear follows a typical pattern and is referred to as a superior labrum tear, anterior to posterior (SLAP tear). How do they happen?
SLAP tears can be caused by trauma such as a fall onto an outstretched hand or can develop over time through repeated stress. Repetitive overhead activities such as throwing or painting can also gradually weaken the labrum over time and lead to a tear. What are the symptoms? Often if a SLAP tear develops over time, patients can be unaware they have sustained an injury at all and there is no significant impact on their pain or function. Pre-existing SLAP tears can however place more tension on the long head of the biceps tendon, leading to overuse disorders of that tendon as a secondary complication. When the tear occurs through a sudden action or trauma, symptoms can be more noticeable. Patients often notice pain deep in the shoulder joint with overhead shoulder movements, a feeling of weakness or a loss of power or accuracy with throwing activities. Some people may feel a popping or clicking sensation and occasionally the shoulder feels like it "gives way". In severe tears, the shoulder might feel unstable and be at increased risk of dislocation. How can physiotherapy help? Your physiotherapist can help diagnose a SLAP tear and send you for scans if needed. SLAP tears are graded by severity from 1 to 4 as a way to guide treatment. Physiotherapy is usually recommended as a trial for all tears before considering surgical repair and in many cases can effectively help patients return to their previous activities, symptom free. If physiotherapy is unsuccessful, surgical repair with a full rehabilitation program is then recommended. Surgery will either repair the tear or reattach the biceps tendon to the humerus (tenodesis). Following surgery, a period of rest in a sling is required before rehabilitation can begin. |
Categories
All
|
|
The Physio Nook
197A Scarborough Beach Road Doubleview WA 6018 08 9446 7017 doubleview@thephysionook.com.au |